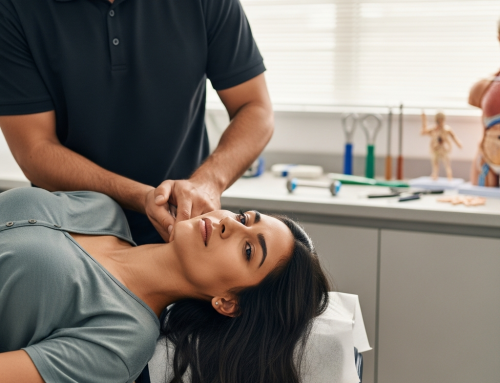
8 Signs a Neck Injury After a Car Accident Needs Care in Irving

You’re sitting at that red light on Highway 183, probably thinking about what to grab for dinner, when you hear the screech of brakes behind you. Your stomach drops. You brace yourself, but there’s nothing you can do – *WHAM.*
The impact isn’t terrible. Your car lurches forward a bit, maybe kisses the bumper of the vehicle ahead. You sit there for a moment, heart pounding, doing that mental inventory we all do: “Am I okay? Do I hurt anywhere?” Your neck feels… fine. Maybe a little stiff, but nothing dramatic. You exchange insurance info, drive home, and figure you dodged a bullet.
Fast forward to tomorrow morning. You wake up and – holy moly – turning your head to check the alarm clock feels like someone’s jabbing a hot poker into your neck. Or maybe it’s three days later when that nagging headache just won’t quit, no matter how much ibuprofen you throw at it.
Here’s the thing about car accidents (and trust me, we see this all the time at our clinic): your body is basically a really sophisticated shock absorber, and sometimes it takes a while for all the systems to report back about what actually happened during impact. Your neck, in particular, is like that friend who says “I’m fine, I’m fine” after clearly twisting their ankle, only to be hobbling around three days later asking for help.
The tricky part? Knowing when that post-accident neck discomfort is just your body working through some temporary soreness versus when it’s something that needs actual medical attention. Because let’s be honest – nobody wants to be that person who rushes to urgent care for every little ache and pain. But you also don’t want to be the person who ignores something that could turn into a bigger problem down the road.
And if you’re living in Irving, you’ve got plenty of options for care… which can actually make the decision even more overwhelming. Do you wait it out? Call your regular doctor? Head to an urgent care center? The paralysis of choice is real, especially when you’re dealing with pain and probably some lingering stress from the accident itself.
What makes neck injuries particularly sneaky is that they don’t always announce themselves with obvious, dramatic symptoms. Sure, sometimes you get the classic whiplash presentation – immediate pain, stiffness, the whole nine yards. But other times? The signs are more subtle. That persistent headache that feels different from your usual tension headaches. Shoulder pain that seems unrelated but actually isn’t. Even things like difficulty concentrating or sleeping problems can be your neck’s way of waving a red flag.
Here’s what we’ve learned from working with countless patients who’ve been in your exact situation: there are specific warning signs that shouldn’t be ignored, even if they seem minor at first. Some of these signs show up immediately, others take their sweet time making an appearance. Some are obvious, others… well, you might not even connect them to your accident initially.
The good news? Most neck injuries from car accidents – even the ones that need treatment – respond really well to the right care when caught early. We’re not talking about major surgery or months of complicated treatment here. Often, it’s about getting ahead of inflammation, preventing scar tissue from forming in problematic ways, and giving your body the support it needs to heal properly.
But timing matters. A lot.
What you’re going to learn in this article are the eight specific signs that your post-accident neck discomfort has crossed the line from “normal post-crash soreness” to “this needs professional attention.” We’ll talk about what each sign actually means (because understanding the “why” helps you make better decisions), when timing becomes critical, and what your options look like right here in Irving.
You’ll also discover why some seemingly unrelated symptoms – like that weird dizziness when you stand up or the fact that you’ve been more irritable than usual – might actually be connected to your neck injury. Sometimes our bodies express trauma in ways that surprise us.
Most importantly, you’ll finish reading this with a clear sense of what warrants a phone call versus what can wait, and what questions to ask when you do seek care.
Your Neck Wasn’t Built for Car Crashes
Think of your neck like a carefully balanced stack of building blocks – seven vertebrae cushioned by discs, held together by ligaments, and powered by muscles that work around the clock. It’s actually pretty remarkable engineering… until a 2,000-pound vehicle suddenly changes direction and your head doesn’t get the memo.
When your car stops abruptly (or gets hit), your body travels with the vehicle, but your head? It keeps going. Then it snaps back. This whiplash motion – and yeah, that’s the actual medical term too – can happen even in seemingly minor fender-benders. You don’t need to be going highway speeds for your neck to take a beating.
The Tricky Thing About Neck Injuries
Here’s what’s confusing about neck injuries after car accidents: they’re sneaky. Really sneaky. You might walk away from the crash feeling fine, maybe a little shaken up but basically okay. You exchange insurance information, maybe grab coffee on the way home, tell your spouse you’re “totally fine.”
Then you wake up the next morning and feel like you’ve been hit by a truck. Which… well, you kind of were.
This delayed reaction happens because your body floods with adrenaline during traumatic events. It’s like nature’s own painkiller, masking injuries for hours or even days. Your fight-or-flight response is so focused on keeping you alive and moving that it basically tells your pain receptors to take a number and wait in line.
Why “Just a Little Stiff” Can Be Misleading
Your neck does a lot more than just hold your head up (though at roughly 10-12 pounds, that’s no small feat). It houses part of your spinal cord, protects major blood vessels, and contains nerve pathways that control everything from your shoulder movement to your ability to feel your fingertips.
When these structures get jostled around – even gently – the effects can ripple out in ways you wouldn’t expect. That tingling in your pinky finger? Could be your neck. Those headaches that started three days after the accident? Probably your neck too.
The Anatomy of Impact
During a rear-end collision, your neck goes through what doctors call a “double trauma.” First, your head gets thrown backward (hyperextension), then it whips forward (hyperflexion). It’s like being on the world’s worst carnival ride, except it happens in milliseconds.
The soft tissues – muscles, ligaments, tendons – stretch beyond their normal range. Sometimes they tear. The vertebrae might shift slightly out of alignment. The discs between your vertebrae can bulge or herniate. And those tiny joints in your neck? They can get inflamed and angry.
What’s particularly frustrating is that these injuries often don’t show up on initial X-rays. Soft tissue damage is invisible to standard imaging, which is why emergency rooms sometimes miss neck injuries entirely. You’re not imagining things if you’re told “everything looks normal” but you feel anything but normal.
The 24-48 Hour Window
Most neck injuries from car accidents start making themselves known within the first day or two. Your body’s natural inflammatory response kicks in, swelling increases, and muscles start to spasm as they try to protect the injured area. It’s like your neck goes into defensive mode – which actually makes things more painful in the short term.
This is why that “wait and see” approach can be problematic. By the time you’re really hurting, the inflammatory cascade is already in full swing. Getting ahead of it with proper treatment can make a huge difference in how quickly you recover.
When “Minor” Isn’t Actually Minor
Insurance adjusters love to use the word “minor” when describing fender-benders. But here’s the thing – even low-speed collisions can cause significant neck injuries. Studies show that meaningful soft tissue damage can occur at impact speeds as low as 6-8 mph. Your neck doesn’t care how much damage there is to your bumper.
The relationship between vehicle damage and injury severity? It’s surprisingly weak. You can walk away from a dramatic-looking crash with nothing more than bruises, or develop chronic neck problems from what looks like a parking lot tap.
That’s why paying attention to how you feel – really feel – matters more than what the cars look like afterward.
When to Stop Waiting and Start Acting
Look, I get it. You’re probably sitting there thinking “maybe it’ll just go away” – and honestly? Sometimes minor aches do fade. But here’s the thing your insurance adjuster won’t tell you: neck injuries have this sneaky habit of getting worse before they get better, especially when you ignore them.
If you’re experiencing any combination of those warning signs we talked about, don’t wait more than 72 hours to see someone. I know, I know – you’ve got work, kids, that presentation due Friday… but here’s a reality check. Untreated neck injuries can turn into chronic pain that lasts months or even years. That “I’ll tough it out” mentality? It might cost you way more than a few hours at the doctor’s office.
Finding the Right Care in Irving (It’s Not All Created Equal)
Not every healthcare provider knows how to properly assess car accident injuries. You want someone who understands the biomechanics of what happens when your body gets thrown around like a rag doll in a metal box.
Start with your primary care doctor if the symptoms seem mild – they can rule out serious issues and refer you appropriately. But if you’re dealing with severe pain, numbness, or any neurological symptoms, head straight to an urgent care center or ER. The emergency room at Baylor Scott & White Irving or Texas Health Harris Methodist are both solid choices if you need immediate attention.
For ongoing care, look for providers who specifically mention auto accident injuries or whiplash treatment. Physical therapy places like ATI Physical Therapy or Benchmark Physical Therapy have seen this stuff countless times. They won’t look at you funny when you explain that your neck hurts when you check your blind spot.
What to Say (and What NOT to Say) at Your Appointment
Here’s where people mess up constantly. They downplay their symptoms because they don’t want to seem dramatic. Stop that. Right now.
Be specific about your pain – is it sharp, dull, burning, aching? Does it shoot down your arm or stay put? When is it worst – morning, evening, when you turn your head? Your doctor isn’t psychic, and “it just hurts” doesn’t give them much to work with.
But here’s the flip side – don’t exaggerate either. Insurance companies are watching, and if your story doesn’t add up, they’ll use it against you. Stick to the facts, be honest about your limitations, and don’t feel guilty about needing help.
One more thing… never, ever say “I feel fine” if you don’t. I’ve seen too many people say this at the scene or even at their first doctor’s visit, only to have symptoms show up days later. Adrenaline is a hell of a drug, and it can mask serious injuries for quite a while.
The Documentation Game (Trust Me on This)
Start keeping a pain journal immediately – and I mean immediately. Not next week when you remember, not when the insurance adjuster asks for it. Today.
Write down your pain level (1-10 scale), what activities make it worse, how your sleep is affected, whether you need help with daily tasks. Take photos if you have visible bruising or swelling. Keep track of any medications you’re taking and whether they help.
This isn’t just busywork – it’s evidence. Insurance companies love to claim that your injury isn’t “that bad” or that it was pre-existing. Your detailed records become your defense against their tactics.
Insurance Realities (The Stuff They Don’t Advertise)
Your insurance might try to rush you into accepting a settlement before you know the full extent of your injuries. Don’t do it. Once you sign that paper, you’re done – even if you develop complications later.
Most policies cover immediate medical care after an accident, but the process can be confusing. Don’t let insurance hassles keep you from getting treatment. Many healthcare providers will work with you on payment plans or accept letters of protection while your claim is pending.
Moving Forward Without Making Things Worse
While you’re waiting for appointments or between treatments, avoid activities that aggravate your symptoms. That means no aggressive stretching (I don’t care what your neighbor told you), no heavy lifting, and definitely no “working through the pain.”
Ice for acute pain and swelling, gentle heat for muscle stiffness – but nothing extreme. And please, resist the urge to crack your own neck. Leave that to the professionals who actually know what they’re doing.
The bottom line? Your health isn’t worth gambling with. When in doubt, get checked out.
When Your Body Plays Hide and Seek with Pain
Here’s the thing that trips up almost everyone after a car accident – your neck might feel perfectly fine for hours, even days. You’re walking around thinking you dodged a bullet, maybe even bragging to your spouse about how tough you are… and then Wednesday morning hits like a freight train.
This delayed onset thing? It’s not your imagination playing tricks. Your body pumps out adrenaline and endorphins during trauma – nature’s own pain medication cocktail. But when that wears off (usually 24-72 hours later), suddenly you’re wondering if someone replaced your pillow with concrete blocks overnight.
The solution isn’t to panic every time you feel stiff after an accident. Instead, pay attention to patterns. Are you reaching for ibuprofen more often? Finding weird positions to get comfortable? These subtle shifts often tell the real story before the obvious pain kicks in.
The “I’m Fine” Trap That Costs You Later
We’ve all been there – someone asks how you’re feeling after the accident, and you automatically say “fine” because… well, that’s what we do. But here’s what actually happens: you start modifying your behavior without realizing it.
Maybe you’re turning your whole body instead of just your head when backing out of parking spaces. Or you’ve unconsciously started sleeping with an extra pillow. Your brain is already compensating for something your conscious mind hasn’t acknowledged yet.
This is where things get expensive – both physically and financially. Insurance companies love it when you say you’re “fine” right after an accident. That casual comment can come back to haunt you when symptoms develop later and you’re trying to get treatment covered.
The smarter approach? Be honest but measured. “I feel okay right now, but I know symptoms can develop later” protects you legally while being truthful. And actually – schedule that check-up even if you feel fine. It’s easier to prevent a problem than fix one that’s been brewing for weeks.
When Dr. Google Becomes Your Worst Enemy
Look, we all do it. Something feels off with your neck, so you start searching symptoms online at 2 AM. Suddenly you’re convinced you have either a minor muscle strain or you’re dying – there’s no middle ground in internet medicine.
The real problem with this approach isn’t just the anxiety spiral (though that’s bad enough). It’s that you start treating symptoms based on guesswork instead of getting proper evaluation. You might be icing when you should be applying heat, or pushing through pain when rest is what’s needed.
Here’s what actually helps: write down your symptoms instead of searching them. What makes it worse? Better? What time of day is roughest? This gives your doctor real information to work with, rather than a list of things you read online that may or may not apply to your situation.
The Insurance Maze That Makes Everything Harder
Nobody warns you about this part – dealing with insurance after a neck injury can be more exhausting than the injury itself. They’ll want documentation for everything, question whether your treatment is “necessary,” and generally make you feel like you’re asking for a kidney when you just want your neck to stop hurting.
The secret weapon here is documentation from day one. Photos of vehicle damage, contact info for everyone involved, and yes – that medical evaluation even if you feel fine. Keep a simple diary of symptoms, treatments, and how you’re functioning day to day.
And here’s something most people don’t know: in Irving, you typically have two years to file a personal injury claim, but waiting makes everything harder. Evidence disappears, memories fade, and insurance companies get more skeptical about delayed claims.
When Your Support System Doesn’t Get It
This might be the hardest part of all. Your neck injury isn’t visible like a cast or crutches would be. Family and friends might start with sympathy, but after a few weeks of you moving carefully or declining activities, you might hear things like “aren’t you better yet?” or “maybe you just need to push through it.”
The isolation can be worse than the physical pain sometimes. People don’t understand that neck injuries mess with sleep, concentration, even your mood – because when you hurt, everything else gets harder.
Finding others who’ve been through similar experiences helps enormously. Whether that’s support groups, online communities, or just being honest with friends about what you’re actually dealing with – connection beats suffering in silence every time.
What to Expect During Recovery – The Real Timeline
Let’s be honest here – everyone wants to know the magic number. How long until I feel normal again? When can I stop worrying about this ache in my neck?
The truth is… it depends. I know that’s not the answer you want to hear, but neck injuries are surprisingly individual. Some people bounce back in a couple of weeks, while others deal with lingering effects for months. It’s not necessarily about how “bad” the accident was either – sometimes a minor fender bender can cause more issues than what looks like a serious crash.
Generally speaking, minor soft tissue injuries might resolve in 2-6 weeks with proper care. More significant injuries? We’re looking at several months, possibly longer. But here’s what I want you to remember – improvement doesn’t always happen in a straight line. You might feel great one day and terrible the next. That’s actually pretty normal, especially in the first few weeks.
Your body is essentially doing construction work – repairing damaged tissues, reducing inflammation, restoring normal movement patterns. And just like any construction project, there are good days and setbacks.
Working with Healthcare Providers
If you’re dealing with persistent neck pain after an accident, you’ll probably work with several different professionals. Think of it as assembling your personal recovery team.
Your primary care doctor might be your starting point, but don’t be surprised if they refer you to specialists. Orthopedic doctors focus on bones and joints, while neurologists deal with nerve-related issues. Physical therapists – they’re often the MVPs of neck injury recovery. They’ll teach you exercises, help restore movement, and give you strategies for managing pain.
Sometimes you might see a pain management specialist, especially if you’re dealing with chronic issues. And yes, some people benefit from alternative treatments like chiropractic care or acupuncture. The key is finding what works for your specific situation.
One thing I always tell people – be an active participant in your care. Ask questions. If something doesn’t make sense, say so. If a treatment isn’t helping after a reasonable amount of time, speak up. You know your body better than anyone else.
When to Seek Immediate Care
Most neck injuries from car accidents aren’t medical emergencies, but there are some red flags that mean you need to get checked out right away – not tomorrow, not next week, but now.
Severe headaches that keep getting worse… numbness or tingling that spreads down your arms… difficulty moving your arms or hands normally… confusion or memory problems… nausea and vomiting that won’t stop. These could signal more serious injuries that need immediate attention.
Also, if your neck pain suddenly becomes much worse, or if you develop new symptoms days or weeks after the accident, don’t ignore it. Sometimes injuries reveal themselves gradually as swelling goes down or as your body compensates in different ways.
Managing Expectations and Mental Health
Here’s something nobody talks about enough – dealing with a neck injury after a car accident isn’t just physical. It’s mentally and emotionally exhausting too.
You might find yourself anxious about driving again. Maybe you’re frustrated because you can’t do normal activities without pain. Perhaps you’re worried about work, bills, or how this affects your family. These feelings? Completely normal and valid.
The uncertainty is probably the hardest part. Will this get better? Am I going to deal with this forever? What if the insurance company doesn’t cover my treatment? It’s okay to feel overwhelmed – this is a lot to handle.
Consider talking to a counselor or therapist who understands trauma and chronic pain. Many people find it helpful to connect with support groups, either in person or online, where they can talk to others who’ve been through similar experiences.
Moving Forward with Confidence
Recovery from a neck injury isn’t always linear, and it requires patience – both with your body and with the process. Some days will be better than others, and that’s okay.
Focus on what you can control – following your treatment plan, doing prescribed exercises, getting enough sleep, eating well, and managing stress. These might seem like small things, but they add up to make a real difference in how you heal.
Remember, seeking help isn’t a sign of weakness – it’s smart. Whether that’s medical care, legal advice about your accident, or emotional support, getting the right help early often leads to better outcomes down the road.
You Don’t Have to Navigate This Alone
Here’s what I’ve learned after years of helping people through post-accident recovery – your body has an amazing way of sending you messages, and those eight warning signs we’ve talked about? They’re not suggestions you can ignore. They’re your body’s way of saying, “Hey, I need some help here.”
I get it though. You’re probably sitting there wondering if you’re overreacting. Maybe you’re thinking, “It’s just a little stiffness” or “I don’t want to be dramatic.” But here’s the thing – there’s absolutely nothing dramatic about taking care of yourself after trauma. Your neck went through something intense, and it deserves attention.
You know what’s actually dramatic? Letting a treatable injury turn into months of chronic pain because you waited too long. I’ve seen it happen, and it breaks my heart every time. Someone comes in six months later, frustrated and exhausted, saying “I wish I’d come in sooner.”
The truth is, early intervention can be the difference between a few weeks of targeted treatment and years of managing symptoms. Your neck – with all those delicate vertebrae, muscles, and nerves – responds so much better when we catch problems early. It’s like tending to a small crack in your windshield before it spreads across the whole thing.
And honestly? You’ve already been through enough. The accident, dealing with insurance, maybe missing work… the last thing you need is to add “ignoring my health” to that list. You deserve to feel good in your own body again.
I also want you to know that seeking help doesn’t make you weak or high-maintenance. It makes you smart. It makes you someone who values their quality of life and isn’t willing to just “tough it out” indefinitely. There’s real wisdom in recognizing when you need support.
Here in Irving, we understand that every accident is different, every person is different, and every recovery looks different too. What matters isn’t comparing your experience to anyone else’s – it’s listening to what your body is telling you right now.
Whether you’re dealing with that nagging headache that won’t quit, numbness that’s got you worried, or pain that’s making simple tasks feel impossible… you don’t have to just endure it. There are real solutions, proven treatments, and people who genuinely care about getting you back to feeling like yourself.
Ready to Feel Better?
If any of those warning signs resonated with you – or if you’re just tired of wondering “what if” – I’d love to talk with you. No pressure, no sales pitch… just an honest conversation about what’s going on and how we might be able to help.
Give us a call or stop by when you’re ready. Sometimes the hardest part is just picking up the phone, but I promise we’ll make everything else as easy as possible. You’ve been taking care of everyone else’s needs – insurance companies, work, family. Now it’s time to take care of yours.
You matter. Your comfort matters. And you absolutely deserve to feel good again.