How Is Head Trauma From a Car Accident Diagnosed in Irving?

You’re driving down MacArthur Boulevard after a long day at work, maybe grabbing dinner from that Thai place you love, when suddenly – BAM. The world goes sideways, airbags explode, and everything becomes a blur of sirens, flashing lights, and concerned voices asking if you’re okay.
“I’m fine,” you tell everyone. Your car might look like an accordion, but you walked away. You’re talking, you’re moving, you even declined the ambulance ride because, honestly, you just want to get home and forget this whole nightmare happened.
But here’s the thing – and this is something most people don’t realize until it’s too late – your brain might not be as “fine” as the rest of you feels.
See, when it comes to head trauma from car accidents, what you can’t see can absolutely hurt you. While you’re focused on that sore neck or the bruise blooming across your chest from the seatbelt (thank goodness for that seatbelt, by the way), your brain might be dealing with its own invisible injuries. And unlike a broken bone that shows up crystal clear on an X-ray, brain injuries… well, they’re trickier. Sneakier.
I’ve talked with countless people here in Irving who thought they dodged a bullet after their accident, only to find themselves dealing with persistent headaches weeks later, or struggling to concentrate at work, or feeling like they’re in a fog that just won’t lift. One woman told me she couldn’t understand why she kept forgetting her kids’ names – names she’d been saying every day for years. That’s when it hit her: maybe she wasn’t as “fine” as she thought.
The tricky part about head trauma is that it doesn’t always announce itself with dramatic symptoms. Sure, sometimes there’s obvious blood or a clear loss of consciousness. But more often? It’s subtle. It’s that nagging headache you blame on stress. It’s feeling more tired than usual. It’s getting frustrated because words aren’t coming as easily as they used to.
And if you’re dealing with this in Irving, you’re actually in a pretty good spot – we’ve got some excellent medical facilities here that know exactly how to spot what others might miss. But here’s what nobody tells you: knowing where to go and what to expect can make all the difference between getting the help you need quickly… or spending weeks wondering why you don’t feel like yourself.
The thing is, diagnosing head trauma isn’t like checking for a broken arm. Your doctor can’t just look at you and say, “Yep, there it is.” It’s more like being a detective, piecing together clues from how you’re feeling, what happened during the accident, and yes – some pretty sophisticated testing that might sound intimidating but really isn’t.
Maybe you’re reading this because you’re dealing with something similar right now. Or perhaps someone you love had an accident recently and you’re worried about them (even though they keep insisting they’re fine). Either way, you’re smart to be asking these questions. Because when it comes to your brain – that incredible, irreplaceable control center for literally everything you do – being informed isn’t just helpful. It’s essential.
What I want to share with you is exactly how doctors here in Irving approach diagnosing head trauma after car accidents. We’re going to talk about the different types of tests they might recommend (and why they’re not as scary as they sound), what symptoms actually matter versus what’s probably just normal post-accident stress, and – perhaps most importantly – when you should stop telling yourself you’re fine and actually get checked out.
Because here’s what I’ve learned after years of seeing people navigate this: the sooner you understand what’s happening in your head after an accident, the sooner you can start feeling like yourself again. And isn’t that what we all want? To get back to being… well, us?
So let’s figure this out together. Your future self will thank you.
The Tricky Nature of Brain Injuries
Here’s the thing about head trauma – it’s nothing like what you see in the movies. You know those scenes where someone gets knocked out, wakes up with a small bandage, and they’re perfectly fine? Yeah, that’s not reality. The brain is more like a delicate computer floating in protective fluid inside your skull. When your car suddenly stops but your brain keeps moving… well, that’s when things get complicated.
Think of it this way – imagine shaking a bowl of Jell-O really hard. The Jell-O might look fine from the outside, but inside? There could be microscopic tears and damage you can’t see. That’s essentially what happens to brain tissue during a car accident, even when there’s no visible injury to your head.
Why Symptoms Don’t Always Show Up Right Away
This part honestly confuses a lot of people – and for good reason. You’d expect that if something’s wrong with your brain, you’d know immediately, right? Not necessarily.
The brain has this weird quirk where it can compensate for damage initially. It’s like when you sprain your ankle but the adrenaline keeps you walking normally for a while. Your brain might mask symptoms for hours, days, or even weeks after an accident. I’ve seen patients walk away from crashes feeling completely normal, only to develop severe headaches, memory problems, or concentration issues later.
Actually, that reminds me of something important – the brain doesn’t have pain receptors. The headaches you feel after head trauma? They’re coming from the blood vessels, muscles, and tissues around your brain, not the brain tissue itself. Kind of wild when you think about it.
The Spectrum of Head Injuries
Car accidents don’t just cause one type of head injury – they’re more like… a troublemaker with multiple tools in their toolkit. You might deal with
Concussions are probably what most people think of first. They’re like your brain getting shaken up in its protective casing. Sometimes there’s no loss of consciousness at all – you just feel “off” afterward.
Contusions are basically brain bruises. If your head hits something hard (like a window or steering wheel), the brain can actually bruise against the inside of your skull. These show up on imaging, unlike many concussions.
Then there are the more serious injuries – things like traumatic brain injuries (TBI) that can affect everything from your personality to your ability to form new memories. These aren’t just medical emergencies; they can change someone’s entire life trajectory.
The Invisible Challenge
Here’s what makes diagnosing head trauma so tricky in Irving’s emergency rooms and clinics – many brain injuries are essentially invisible. A broken arm? Easy to see on an X-ray. A brain injury? Not so much.
Standard CT scans and MRIs can miss subtle brain injuries, especially the microscopic tears in brain tissue that we call diffuse axonal injury. It’s like trying to spot a small tear in a complex piece of fabric – unless you know exactly where to look and have the right tools, you might miss it entirely.
This is why doctors have started using more sophisticated diagnostic approaches. They’re looking at everything from balance tests to cognitive assessments, because sometimes the only way to detect brain damage is by seeing how it affects function.
The Time Factor Nobody Talks About
Something that catches people off guard is how head trauma can evolve over time. What starts as a mild headache can develop into something much more serious. Or the opposite – symptoms that seem terrifying initially might resolve completely with proper rest and treatment.
Your brain has this amazing ability to rewire itself (neuroplasticity is the fancy term), but it also means that the full extent of an injury might not be apparent for weeks or months. It’s like assessing damage to a house after an earthquake – some cracks show up immediately, while others develop as the structure settles.
This is exactly why medical professionals in Irving take a methodical, often cautious approach to head trauma diagnosis. They’re not just looking at how you feel today – they’re trying to predict and prevent problems that might emerge down the road. Because when it comes to your brain, it’s always better to be overly careful than to miss something that could affect you for years to come.
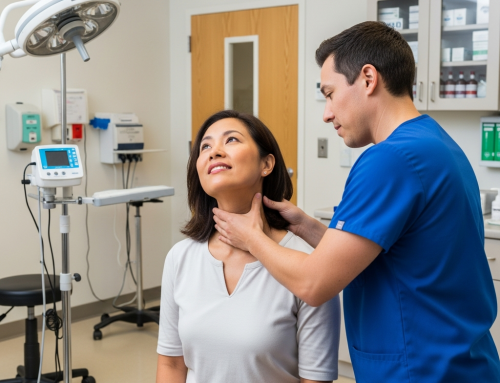
What to Expect During Your Initial Assessment
You know that feeling when you’re trying to describe a headache to someone who’s never had one? That’s often what patients face when they first arrive at an emergency room or urgent care after a car accident. The good news is that medical professionals in Irving are trained to look beyond what you’re able to articulate.
The first thing they’ll do is check your Glasgow Coma Scale score – don’t worry, it sounds scarier than it is. They’re basically testing how alert you are by asking you to open your eyes, speak, and move on command. Think of it as a quick mental status check. If you’re reading this and understanding it, you’re probably doing just fine on that front.
Here’s something most people don’t realize: even if you feel “fine,” medical staff will likely keep you under observation for several hours. Head injuries are sneaky – symptoms can show up 24 to 48 hours later. It’s like that bruise that doesn’t appear until the next day, except with potentially more serious consequences.
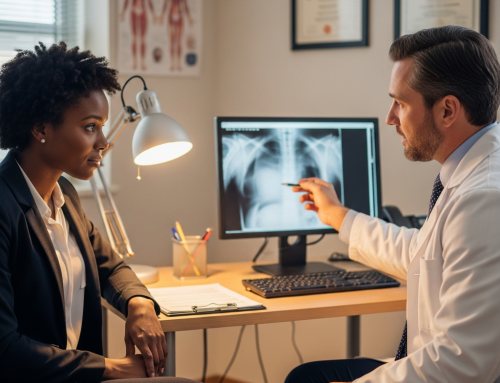
The Imaging Decision Tree (And Why Timing Matters)
Not everyone needs a CT scan immediately – actually, there’s a whole decision-making process that doctors use. They follow something called the Canadian CT Head Rule, which sounds official because, well, it is. But here’s the practical translation: if you lost consciousness for more than five minutes, vomited more than twice, are over 65, or have certain types of memory loss, you’re getting that scan.
The timing of when you get imaging can be crucial. If it’s been less than six hours since your accident, a CT scan might not show certain types of bleeding yet. Sometimes doctors will repeat scans 12-24 hours later if your symptoms change or worsen. Don’t be alarmed if they want to scan you again – it’s actually good medicine.
Here’s an insider tip: if you’re claustrophobic, mention it upfront. Most facilities can give you something to help you relax, or they might use an “open” CT scanner if available. The last thing anyone wants is for you to panic halfway through the scan.
Neurological Testing That Goes Beyond the Basics
You’ve probably seen those “follow my finger” tests in movies, but real neurological assessments are much more thorough. Your doctor might ask you to walk heel-to-toe in a straight line (harder than it sounds when your brain’s been rattled), or they’ll test your reflexes with that little rubber hammer.
One test that catches people off guard is the cognitive assessment. They might ask you to remember three words, then distract you with math problems, then ask for those words again. Or they’ll have you draw a clock showing a specific time. These aren’t trick questions – they’re genuinely checking how different parts of your brain are functioning.
Red Flags That Mean “Get Back to the Hospital Now”
Even after you’ve been cleared to go home, your brain needs monitoring. Write these warning signs down on your phone right now – seriously, your short-term memory might not be at 100% for a while.
If your headache gets progressively worse (not just different, but actually more intense), if you start vomiting repeatedly, or if you become unusually drowsy or confused, don’t wait until morning. These could signal increasing pressure in your skull, which is a medical emergency.
Changes in personality or behavior are equally important. If your family says you’re acting “off” or if you feel like you’re not quite yourself, trust that instinct. Sometimes the people closest to us notice subtle changes before we do.
The Follow-Up Plan Nobody Talks About
Here’s what often gets glossed over: recovery from head trauma isn’t always linear. You might feel great for a few days, then have a rough patch. That doesn’t mean you’re getting worse – healing isn’t always smooth sailing.
Most doctors will want to see you again within a week, even if you’re feeling fine. This isn’t just a formality… your brain might still be settling down from the initial injury. Think of it like checking on a sprained ankle – you wouldn’t just ignore it after the first day, right?
Keep a simple log of how you’re feeling each day. Note your energy levels, any headaches, sleep quality, and mood changes. This information becomes incredibly valuable if you need additional treatment or if you’re dealing with insurance claims later on.
When Symptoms Don’t Show Up Right Away
Here’s what nobody tells you about head trauma – sometimes your brain decides to be sneaky about it. You walk away from that fender-bender on Highway 183 feeling fine, maybe a little shaken up, but basically okay. Then three days later? You can’t remember where you put your coffee mug… again. And again.
This delayed onset thing trips up so many people. Your adrenaline was pumping after the accident, masking symptoms that are now creeping in like unwelcome houseguests. The solution isn’t to panic (though honestly, who doesn’t?). Instead, keep a simple symptom journal on your phone. Just quick notes – “headache at 2pm,” “felt dizzy getting up,” “forgot Sarah’s name for a second.”
Sounds obsessive? Maybe. But when you’re sitting in Dr. Martinez’s office in Irving and she asks about your symptoms, you’ll have actual data instead of that vague “I just feel… off” feeling.
The Insurance Maze Nobody Warns You About
Let’s be real – dealing with insurance after a car accident feels like trying to solve a Rubik’s cube while riding a unicycle. They want documentation for everything, but getting that CT scan scheduled feels impossible when you can barely focus long enough to make the appointment.
Here’s what actually works: call your insurance company first thing in the morning when your brain is freshest. Have your accident report number ready, and don’t be afraid to ask them to repeat things. Actually, ask them to email you a summary of what diagnostic tests they’ll cover – your memory might not be reliable right now, and that’s completely normal.
Pro tip from someone who’s been there? If you’re dealing with the other driver’s insurance, they might try to rush you into accepting a quick settlement before you’ve had proper neurological testing. Don’t. Brain injuries can take weeks to fully manifest, and you deserve thorough evaluation.
When Family Members Don’t Get It
This one’s tough. Your spouse keeps asking if you’re “better yet” because you look fine on the outside. Your kids are frustrated because you forgot about soccer practice… again. And honestly? You’re starting to wonder if you’re making it all up.
You’re not making it up.
Brain injuries are invisible disabilities, and they’re real even when people can’t see them. Consider bringing a family member to your diagnostic appointments in Irving – not just for support (though that helps), but so they can hear directly from the doctor about what’s happening in your brain.
Sometimes families need education about traumatic brain injury just as much as patients do. Ask your healthcare provider about resources for loved ones, or look into support groups at places like the Brain Injury Association of Texas.
The “Am I Going Crazy?” Phase
Here’s something doctors don’t always prepare you for – the psychological impact of not trusting your own brain. When you can’t remember conversations you had yesterday or you’re getting lost driving to places you’ve been a hundred times… it’s terrifying.
That anxiety? It’s not helping your healing process, but it’s completely understandable. Consider this: your brain is like a computer that got jostled around. Some files might be temporarily corrupted, but that doesn’t mean the whole system is broken.
Practical solution: establish routines and external memory aids while your brain heals. Use your phone’s calendar religiously. Set reminders for everything – medications, appointments, even meals. It’s not giving up; it’s giving your brain space to recover.
Finding the Right Specialists in Irving
Not all doctors understand traumatic brain injury, and that’s frustrating when you’re already dealing with cognitive symptoms. You might see your primary care doctor first, but if they seem dismissive or suggest you just “rest and you’ll be fine,” advocate for yourself.
Irving has some excellent neurologists and neuropsychologists, but getting in can take weeks. Don’t let that stop you from making the appointment now. In the meantime, document everything and consider seeing a physician who specializes in concussion management.
The key is finding someone who takes your symptoms seriously – even the weird ones, like how bright lights suddenly bother you or how you can’t handle being in crowded places anymore. Those aren’t character flaws; they’re neurological symptoms that deserve proper attention and treatment.
What to Expect During the Diagnostic Process
Let’s be real – getting a head injury diagnosis isn’t like getting a strep throat test where you know the results in ten minutes. The whole process can feel frustratingly slow when you’re dealing with symptoms that are genuinely scary.
Most people walk into the ER thinking they’ll get a quick scan and clear answers. But here’s the thing… brain injuries don’t always show up immediately, and doctors need time to piece together the full picture. You might have blood work, imaging, and neurological tests spread across several hours – or even multiple visits.
If your symptoms are mild, you could be looking at a few hours in the emergency room. More complex cases? That timeline stretches to days of testing and observation. I know it’s nerve-wracking, but this thoroughness is actually working in your favor.
The Waiting Game (And Why It Matters)
Here’s something that catches a lot of people off guard – sometimes the most important diagnostic tool is time itself. Concussion symptoms can be sneaky little things that don’t show their true colors for 24-48 hours after impact.
Your doctor might send you home with instructions to watch for worsening symptoms. This doesn’t mean they’re brushing you off or missing something critical. They’re being smart about it, actually. Many mild traumatic brain injuries reveal themselves gradually, and that observation period is crucial data.
You’ll probably get a list of “red flag” symptoms to watch for – things like repeated vomiting, severe confusion, or seizures. Keep that list handy, and don’t hesitate to come back if anything changes. Trust me, medical professionals would much rather see you again for peace of mind than miss something important.
Understanding Your Results
When those test results start coming in, the language can feel overwhelming. “Mild traumatic brain injury” sounds terrifying, but remember – in medical terms, “mild” refers to the initial severity, not how you’re feeling right now.
CT scans might come back “normal” even when you’re definitely not feeling normal. That’s actually pretty common with concussions. The absence of bleeding or swelling on imaging doesn’t mean your symptoms aren’t real or significant – it just means you’re dealing with a different type of brain injury.
MRI results can be more detailed, but even these sophisticated scans don’t catch everything. Your symptoms and how you’re functioning day-to-day often tell the more complete story than any single test result.
Your Recovery Roadmap
Once you’ve got a diagnosis, the next question everyone asks is: “How long until I’m back to normal?” And honestly? That’s the million-dollar question that doesn’t have a one-size-fits-all answer.
Most people with mild head injuries start feeling better within a few weeks to a few months. But recovery isn’t always linear – you might have good days followed by rough patches. That’s completely normal, even though it’s incredibly frustrating.
Your healthcare team will likely set you up with follow-up appointments, maybe with a neurologist or concussion specialist. These aren’t just check-the-box visits… they’re opportunities to adjust your treatment plan based on how you’re actually healing, not how textbooks say you should be healing.
Building Your Support Network
You’re probably going to need some help navigating this – and that’s okay. Head injuries affect everything from your ability to concentrate at work to managing household tasks that used to be second nature.
Consider connecting with others who’ve been through similar experiences. There are support groups, both in-person and online, where you can talk to people who actually understand why grocery shopping suddenly feels overwhelming or why bright lights make you want to hide under a blanket.
Moving Forward Realistically
The hardest part might be accepting that recovery happens on its own timeline, not yours. You might need to modify work schedules, take breaks from activities you love, or ask for help with things you’ve always handled independently.
This isn’t permanent – though it might feel like it some days. Most people do get back to their normal lives, but it often looks different than the straight line from injury to complete recovery that we all hope for.
Keep track of your symptoms, be patient with yourself, and stay connected with your medical team. Recovery is rarely perfect or predictable, but with the right support and realistic expectations, you’re setting yourself up for the best possible outcome.
You know what strikes me most about head trauma after car accidents? It’s how sneaky it can be. You walk away from that fender-bender thinking you’re fine – maybe a little shaken up, sure – but your brain might be quietly dealing with something much more serious. And honestly? That’s exactly why getting proper medical attention isn’t just smart… it’s essential.
The thing is, your brain doesn’t always send up obvious red flags right away. Those headaches that start three days later, the way you can’t quite concentrate at work, that strange dizziness when you stand up – these aren’t just “normal” stress responses. They’re your body’s way of waving a white flag, asking for help.
The Peace of Mind Factor
Here’s what I’ve learned from talking to countless people who’ve been through this: the worst part isn’t always the physical symptoms. It’s the uncertainty. The wondering. The lying awake at night thinking, “Is this normal, or should I be worried?”
Getting a thorough evaluation – whether that’s a CT scan, MRI, or even just a comprehensive neurological exam – doesn’t just diagnose potential problems. It gives you answers. And sometimes, those answers are reassuring. Sometimes they reveal something that needs attention. But either way? You’re not left wondering anymore.
Your Support System Matters
I can’t stress this enough – you don’t have to navigate this alone. Whether it’s your primary care doctor, a neurologist, or specialists at local Irving medical centers, there are people whose entire job is helping folks like you figure out what’s going on. They’ve seen it all, they understand the complexities of head trauma, and they genuinely want to help you feel better.
And here’s something that might surprise you: most medical professionals understand that car accidents are traumatic in more ways than one. The good ones won’t rush you, won’t dismiss your concerns, and won’t make you feel like you’re overreacting. Because honestly? When it comes to your brain, there’s no such thing as overreacting.
Moving Forward
The reality is that early intervention makes a huge difference with head injuries. The sooner any issues are identified and addressed, the better your outcomes tend to be. It’s like catching a small leak in your roof before it becomes a major problem – much easier to fix, much less disruptive to your life.
But beyond the medical stuff… taking care of yourself after an accident is an act of self-respect. You matter. Your wellbeing matters. The people who care about you want to see you healthy and thriving, not struggling with symptoms that could be addressed.
If you’re reading this and thinking, “Maybe I should get checked out,” trust that instinct. Whether it’s been a few days or a few weeks since your accident, it’s not too late. Your future self will thank you for taking that step.
Ready to get some answers? Our team understands exactly what you’re going through, and we’re here to help you figure out the next best step for your health. Give us a call – no pressure, just real people who care about helping you feel like yourself again.