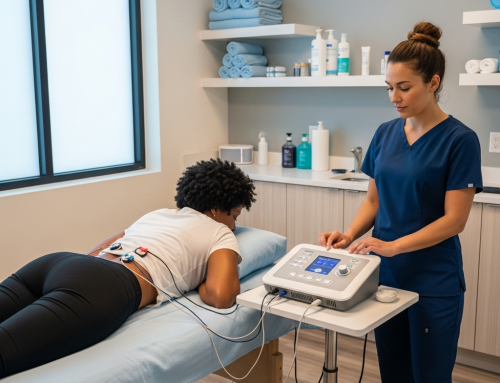
Car Wreck Doctor for Post-Accident Rehab in Farmers Branch
You’re sitting at that red light on Josey Lane, probably checking your phone or thinking about dinner plans, when WHAM – some distracted driver plows into your rear bumper. Your heart’s racing, your neck feels… weird, and suddenly you’re dealing with insurance companies, tow trucks, and that nagging worry that something’s not quite right with your body.
Sound familiar?
If you live in Farmers Branch – or really anywhere in the Dallas area – chances are pretty good you’ve either been in a fender bender yourself or watched it happen to someone you love. And here’s what nobody tells you in those first chaotic moments after impact: the real challenge isn’t getting your car fixed. It’s figuring out what to do when your body starts sending you those uncomfortable little messages days or weeks later.
You know the ones I’m talking about. That stiff neck that won’t loosen up no matter how many hot showers you take. The headaches that seem to come out of nowhere. That weird ache in your lower back that wasn’t there before the accident but now greets you every morning when you roll out of bed.
Here’s the thing – and this might surprise you – your body is incredibly good at masking injury in those first few hours after a crash. Adrenaline’s a powerful drug, and it can make you feel invincible right when you need to exchange insurance information and file police reports. But once that chemical high wears off? That’s when reality sets in.
I’ve talked to countless people who walked away from accidents thinking they were fine, only to find themselves three weeks later unable to turn their head without wincing or struggling to concentrate at work because of persistent headaches. It’s frustrating, it’s scary, and worst of all… it’s completely unnecessary if you know what to do.
The truth is, post-accident injuries – especially the soft tissue kind that don’t show up on X-rays – have this sneaky habit of getting worse before they get better. Without proper treatment, that minor neck strain can turn into chronic pain that follows you around for months or even years. What starts as a little stiffness becomes a life-altering problem that affects everything from your sleep to your mood to your ability to play with your kids.
But here’s the good news (because there absolutely is good news): the right medical care, started at the right time, can make all the difference between a full recovery and a lifetime of managing pain.
That’s where specialized car wreck doctors come in – and if you’re in Farmers Branch, you’ve got some excellent options that too many people don’t know about. These aren’t your typical family medicine docs who see everything from strep throat to diabetes. We’re talking about physicians who understand exactly what happens to your body during a collision, who know how to spot the subtle signs of injury that other doctors might miss, and who have the expertise to create treatment plans that actually work.
Think of it like this: if your car’s transmission started making weird noises, you wouldn’t take it to just any mechanic, right? You’d find someone who specializes in transmissions. Same principle applies to your body after an accident.
Over the next few minutes, we’re going to walk through everything you need to know about finding the right post-accident care in Farmers Branch. I’ll share what to look for in a car wreck specialist, how to navigate the often-confusing world of insurance coverage (spoiler alert: it’s probably better than you think), and most importantly, how to give yourself the best possible chance of getting back to feeling like… well, like yourself again.
Because here’s what I really want you to understand: that accident – whether it happened yesterday or last month – doesn’t have to define how you feel for the rest of your life. With the right care, from the right doctor, at the right time, you can absolutely get back to normal.
And honestly? Sometimes people tell me they end up feeling even better than they did before the accident, once they finally address issues they’d been ignoring for years.
Ready to learn how to make that happen?
When Your Body Becomes a Crime Scene
After a car accident, your body isn’t just injured – it’s evidence. Every ache, every stiff joint, every weird tingling sensation is telling a story about what happened in those split seconds when physics took over. But here’s the thing that catches most people off guard: the immediate aftermath rarely tells the whole story.
Think of it like this… you know how sometimes you don’t realize you’ve burned your hand on the stove until minutes later? Your nervous system was too busy dealing with the immediate threat to send you the “ouch” memo. Car accidents work similarly, except instead of a brief delay, we’re talking days or even weeks before your body fully processes what just happened.
The adrenaline that floods your system during a crash is like nature’s own painkiller. It’s incredibly effective at masking injuries – which is why you might walk away from a fender-bender feeling fine, only to wake up the next morning moving like you aged thirty years overnight.
The Hidden Damage Nobody Talks About
Most people think car accident injuries are pretty straightforward. Broken bones, cuts, maybe a concussion if things got really bad. But the reality? The most common injuries are actually the sneaky ones – the soft tissue damage that doesn’t show up on X-rays and takes its sweet time revealing itself.
Your spine, for instance, is basically a complex tower of blocks held together by muscles, ligaments, and discs. When a car suddenly stops (or gets stopped for it), your spine experiences forces it was never designed to handle. Even at relatively low speeds – we’re talking 5-10 mph – your neck can whip back and forth with surprising violence.
Here’s what’s counterintuitive: the severity of the accident doesn’t always correlate with the severity of your injuries. I’ve seen people walk away from dramatic crashes with minor bumps and bruises, while others develop chronic pain after seemingly minor incidents. It’s frustrating and doesn’t make logical sense, but that’s how our bodies work sometimes.
Why Your Regular Doctor Might Miss Things
This is going to sound harsh, but your family doctor – as wonderful as they might be – probably isn’t the right person to handle your post-accident care. It’s not their fault, really. Medical school doesn’t spend much time on the biomechanics of car crashes or the subtle ways trauma manifests weeks after the fact.
Think about it this way: you wouldn’t ask a general contractor to fix your car’s transmission, right? Different expertise, different tools, different approach entirely. Car wreck doctors are specialists who understand how the human body responds to sudden acceleration, deceleration, and impact forces. They know what to look for when standard tests come back “normal” but you’re still hurting.
The Insurance Company Dance
Let’s be honest about something most people don’t realize until they’re in the middle of it – insurance companies have their own agenda, and it’s rarely aligned with your long-term health and wellbeing. They want to close your case quickly and cheaply. Can’t really blame them; they’re a business, not a charity.
But here’s where things get tricky… if you don’t establish a clear medical record early on, connecting your symptoms to the accident becomes much harder down the road. It’s like trying to prove a recipe caused food poisoning three weeks later – possible, but significantly more complicated.
Beyond the Physical: When Your Brain Gets Shaken
One of the most overlooked aspects of car accidents is how they affect your brain. Even without a direct head impact, the sudden jarring motion can cause what’s essentially a mild traumatic brain injury. You might notice you’re more forgetful, easily frustrated, or having trouble concentrating. These aren’t character flaws or signs you’re “getting old” – they’re legitimate medical symptoms that deserve attention.
The brain is remarkably delicate, floating in fluid like an egg yolk in its shell. When that shell gets rattled hard enough… well, things can get scrambled even without obvious external damage.
What makes this particularly challenging is that cognitive symptoms often develop gradually and can be subtle. You might just feel “off” without being able to pinpoint exactly what’s wrong. Family members sometimes notice changes before you do, which can be unsettling but is actually pretty normal given how these injuries work.
Finding the Right Doctor in Farmers Branch – What Most People Miss
Here’s something insurance companies won’t tell you: not every doctor understands car accident injuries. You could walk into your regular physician’s office with whiplash, and they might send you home with ibuprofen and a “wait and see” approach. That’s… not going to cut it.
Look for doctors who specifically mention “motor vehicle accidents” or “personal injury” on their websites. In Farmers Branch, you want someone who sees these cases regularly – not as a side note to their family practice. Ask directly: “How many car accident patients do you treat monthly?” If they hesitate or give you a vague answer, keep looking.
And here’s a insider tip: the best post-accident doctors often work with multiple specialists under one roof. Physical therapists, chiropractors, massage therapists… it’s like having a whole rehab team without the hassle of coordinating between different offices across town.
Your First Appointment – Come Prepared (Trust Me on This)
Most people show up to their first appointment thinking the doctor will just “figure it out.” Wrong move. Your pain levels, symptoms, and limitations change daily after an accident – sometimes hourly. Start a simple pain journal from day one, even if it’s just notes in your phone.
Rate your pain 1-10 at different times of day. Note what makes it worse (sitting? turning your head? getting out of bed?). Document those weird symptoms too – the ones you think might not be related. That foggy feeling? The sudden mood changes? The fact that you can’t concentrate like you used to? Write it all down.
Bring every single piece of paperwork from the accident. Police reports, insurance claims, even photos from the scene. Your doctor needs the full picture – how fast were you going? Did you see the impact coming? Were you wearing a seatbelt? These details actually matter for your treatment plan.
The Insurance Dance – Playing the Game Right
Here’s where things get tricky… and frankly, a bit frustrating. Your car insurance might cover medical expenses through PIP (Personal Injury Protection), but there are usually limits and specific rules. Some policies require you to start treatment within 14 days of the accident. Others have caps on chiropractic visits or massage therapy sessions.
Don’t assume your doctor’s office will handle all the insurance coordination – they won’t. Stay on top of your claim numbers, approval requirements, and coverage limits. I’ve seen people miss out on beneficial treatments simply because they didn’t understand their own policy.
And if the other driver was at fault? That’s a whole different ballgame. Their insurance company will eventually (hopefully) cover your medical bills, but you might need to pay upfront and get reimbursed later. Make sure your chosen doctor’s office is comfortable with lien arrangements if needed.
Red Flags – When to Run (Not Walk) Away
Not all post-accident care is created equal, and unfortunately, some providers see dollar signs instead of patients. Be wary of any doctor who immediately suggests months of treatment without examining you first. Or pushes expensive equipment rentals and supplements before addressing your actual symptoms.
High-pressure tactics are another warning sign. Good doctors explain your options and let you decide. They don’t insist you commit to a 12-week program on your first visit or make you feel guilty for wanting a second opinion.
Also watch out for offices that seem more focused on your insurance coverage than your actual condition. Questions about your policy limits shouldn’t come before questions about your pain levels.
Making Treatment Work in Your Real Life
Let’s be honest – you’ve got work, family, responsibilities that don’t pause because you were rear-ended on 635. Look for flexible scheduling and doctors who understand this reality. Some Farmers Branch clinics offer early morning or evening appointments specifically for working professionals.
Don’t skip appointments because you’re “feeling better” – post-accident injuries are sneaky. You might feel fine one day and wake up the next morning barely able to move. Consistency in treatment often prevents these setbacks better than any medication.
And here’s something most people don’t think about: find a clinic that’s actually convenient to your daily routine. If you have to drive across town during rush hour for every appointment, you’ll start finding excuses to skip them. Sometimes the “good enough” doctor who’s five minutes from your office beats the “perfect” doctor who’s 30 minutes away.
Your recovery isn’t just about getting back to where you were before the accident – it’s about preventing long-term issues that could affect you for years to come.
The Insurance Maze – When Your Claim Feels Like a Full-Time Job
Let’s be honest – dealing with insurance after a car accident is about as fun as a root canal. You’re already hurting, and now you’ve got adjusters calling every other day asking the same questions… it’s exhausting.
The biggest hiccup? Getting pre-authorization for treatment. Your doctor recommends physical therapy three times a week, but your insurance company wants to debate whether twice is “sufficient.” Meanwhile, your neck feels like someone’s tightening a vise every morning.
Here’s what actually works: Document everything. I mean everything. Keep a daily pain journal – sounds tedious, but it becomes gold when you’re fighting for coverage. Take photos of visible injuries (even if they seem minor). Save every medical report, every receipt, even parking stubs from doctor visits.
And here’s something most people don’t know – you can request a peer-to-peer review if your claim gets denied. Your doctor can literally talk to their doctor and explain why you need that treatment. It’s not guaranteed, but it works more often than you’d think.
When Your Body Doesn’t Follow the Timeline
This one gets me every time… People come in expecting to feel better in two weeks because that’s what they’ve seen in movies. Real recovery? It’s messier than that.
Some days you’ll wake up feeling almost normal. Then – boom – the next day you can barely turn your head. It’s not in your imagination, and it doesn’t mean you’re “not healing properly.” Soft tissue injuries are notorious for this rollercoaster pattern.
The solution isn’t pushing through the pain (please don’t do that). Instead, learn to read your body’s signals. Good pain versus bad pain – your rehab team will teach you the difference. Good pain feels like a muscle working hard. Bad pain is sharp, shooting, or makes you want to protect that area.
Track your symptoms, but don’t obsess over them. Notice patterns – maybe you’re worse on rainy days, or after sitting at a desk for hours. These aren’t random; they’re clues your treatment team can use.
The Emotional Rollercoaster Nobody Talks About
Here’s something that catches people off guard – the emotional aftermath. You might find yourself getting anxious every time you drive past the intersection where it happened. Or maybe you’re just… angry all the time.
Post-accident anxiety is real, and it can actually slow down your physical healing. When you’re constantly tense, your muscles can’t relax enough to recover properly. It’s like trying to heal a cut while constantly picking at it.
Don’t try to tough it out alone. Most good rehab clinics have counselors or can refer you to someone who specializes in trauma. And honestly? Sometimes just knowing that irritability and sleep problems are normal parts of recovery helps more than you’d expect.
Working Around Work (The Impossible Puzzle)
This is where things get really tricky. Your doctor says you need to avoid heavy lifting, but you work in a warehouse. Or you’re supposed to do exercises three times a day, but you’re stuck in meetings from sunrise to sunset.
The key is being upfront with your employer about your limitations – and yes, I know that feels risky. But here’s the thing: most workplace injuries happen when people try to push through restrictions they haven’t communicated. Document everything you tell your supervisor, and ask HR about modified duties.
For exercise compliance… let’s get creative. Can you do neck stretches during conference calls? Some exercises in your car during lunch? Your rehab team can help modify routines to fit your actual life, not some ideal version where you have unlimited time.
When Progress Stalls (And It Will)
There comes a point in almost every recovery where you hit a wall. You’ve been doing everything right – attending appointments, doing your exercises, following restrictions – but suddenly you’re not getting better. Sometimes you even feel worse.
This is normal. Healing isn’t linear, despite what those motivational recovery charts suggest. Your body might be working on deeper issues now, or you might need to switch up your treatment approach.
The solution isn’t to panic or give up. It’s to communicate with your team. Maybe you need a different type of therapy, or perhaps it’s time to address sleep issues that are interfering with recovery. Sometimes the plateau is actually your body’s way of consolidating the progress you’ve made.
Trust the process, but don’t suffer in silence. Your recovery is a conversation, not a monologue.
What to Expect During Your First Few Weeks
Let’s be honest – you’re probably feeling pretty overwhelmed right now. Between insurance calls, car repairs, and that nagging pain in your neck… it’s a lot. And now you’re wondering what recovery actually looks like.
Here’s the thing: every person heals differently. I know that’s not the concrete timeline you’re hoping for, but it’s the truth. Some folks bounce back from whiplash in a few weeks, while others need months of consistent care. Your body’s going to set the pace, not your calendar.
That said, most of our patients start noticing some improvement within the first 2-3 weeks of treatment. Nothing dramatic – maybe you can turn your head a little further, or that sharp pain becomes more of a dull ache. Small wins, but they matter.
During those initial visits, your car wreck doctor will likely focus on reducing inflammation and restoring basic movement. Think gentle adjustments, maybe some soft tissue work, and yes… probably some exercises you’ll need to do at home. (I know, I know – homework when you’re already hurting isn’t fun.)
The Reality Check You Need
Here’s what no one tells you: recovery isn’t a straight line. You’ll have good days and bad days – sometimes back-to-back. Tuesday you might feel like you’re finally turning a corner, then Wednesday morning you wake up feeling like you got hit by that car all over again.
This doesn’t mean you’re not healing. It’s actually completely normal.
Your body is essentially rewiring itself after trauma. Muscles that were protecting injured areas need to learn to relax again. Your nervous system – which went into high alert during the accident – needs time to calm down. Even your sleep patterns might be off, which affects everything else.
Most car accident injuries involve some combination of soft tissue damage, joint misalignment, and muscle tension. The good news? These respond well to conservative treatment. The less good news? It takes time. We’re talking weeks to months, not days.
Your Treatment Plan Will Evolve
Your first treatment plan isn’t set in stone – think of it more like a GPS route that recalculates based on traffic conditions. Your car wreck doctor will adjust the approach as your body responds and heals.
Initially, you might be coming in 2-3 times per week. That frequency usually decreases as you improve, transitioning to maintenance care or specific strengthening phases. Some patients graduate to once-weekly visits, others might need intensive therapy for a longer period.
The key is staying consistent, even when you’re having a good day. (Actually, especially when you’re having a good day.) Skipping appointments because you feel better is like stopping antibiotics mid-course – it can set back your progress.
Building Your Support Network
Recovery happens best when you’ve got a solid team around you. Your car wreck doctor is obviously central, but you might also work with massage therapists, physical therapists, or other specialists depending on your specific injuries.
Don’t forget about the non-medical support either. Family and friends who understand that some days you just can’t do everything you used to… they’re invaluable. You might need help with grocery shopping, house cleaning, or even just someone to drive you to appointments when your neck isn’t cooperating.
Preparing for the Long Game
I wish I could tell you that six weeks from now, you’ll be completely back to normal. Some people are – but many aren’t, and that’s okay too. Planning for a longer recovery doesn’t mean you’re being pessimistic; you’re being realistic.
This might mean adjusting work responsibilities temporarily, asking for help with physical tasks, or even modifying your exercise routine. The patients who do best are the ones who give themselves permission to heal at their body’s pace, not society’s expectations.
Your car wreck doctor will help you navigate decisions about when to return to full activities, how to modify your daily routine, and what warning signs to watch for. They’ll also work with you on preventing future problems – because once you’ve been through this, the last thing you want is a setback.
Remember, seeking proper care after a car accident isn’t just about feeling better today. You’re investing in your long-term health and mobility. That’s pretty important stuff, and it deserves the time and attention it takes.
Taking the Next Step Forward
Look, nobody plans for their life to get turned upside down by a car accident. One minute you’re driving to work, thinking about what you’ll have for lunch… the next minute, everything changes. Your back aches when you get out of bed. Your neck feels like it’s made of concrete. And that headache? It’s become your unwelcome daily companion.
But here’s what I want you to know – and this comes from watching hundreds of people navigate this exact situation – you don’t have to accept this as your new normal. Those nagging pains, that stiffness that makes you feel twenty years older, the way you now hesitate before lifting anything heavier than a coffee cup… none of that has to be permanent.
The truth is, your body has an incredible capacity to heal – it just needs the right support. Think of it like this: if your car got damaged in the accident, you wouldn’t just live with a dented bumper and hope it eventually fixed itself, right? You’d take it to someone who knows exactly how to restore it. Your body deserves that same level of expert care.
What makes all the difference is finding healthcare providers who truly understand post-accident injuries. We’re talking about doctors who know that whiplash isn’t just “a little neck pain that’ll go away on its own.” Physical therapists who understand that your shoulder injury might be connected to that lower back discomfort you’re feeling. Specialists who recognize that healing isn’t just about treating symptoms – it’s about getting you back to being… well, you.
And let’s be honest about something else – dealing with insurance companies, medical appointments, and all the paperwork? It’s exhausting when you’re already dealing with pain. The right medical team handles those headaches for you, so you can focus on what really matters: getting better.
I’ve seen people who thought they’d never golf again sink that perfect putt six months after their accident. Moms who couldn’t lift their toddlers without wincing, now chasing them around the playground again. Office workers who dreaded their morning commute because sitting hurt so much, now actually enjoying their drive to work.
The thing is, every day you wait is another day you’re not feeling like yourself. Your family notices when you’re hurting, even when you try to hide it. Your work suffers when you’re distracted by discomfort. Your sleep gets interrupted by those middle-of-the-night aches that make you toss and turn.
You deserve better than that. Actually, let me put it differently – you deserve to feel like yourself again.
If you’re reading this and thinking, “That sounds like exactly what I’m going through,” then please… don’t wait another week hoping things will magically improve. Reach out to a car wreck doctor who specializes in post-accident rehabilitation. Ask questions. Get that evaluation you’ve been putting off.
Your future self – the one who wakes up without pain, who can hug their kids without hesitation, who doesn’t think twice about reaching for something on a high shelf – that person is counting on the decision you make today.
You’ve already survived the hardest part. Now let’s get you thriving again.