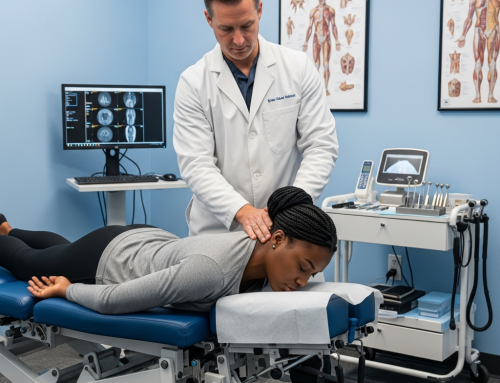
9 Questions to Ask a Personal Injury Doctor After a Motor Vehicle Accident
The metal crunch still echoes in your ears. Your hands won’t stop shaking – not from the cold, but from that split second when everything changed. One moment you’re thinking about what to make for dinner, the next you’re standing on the side of the road watching a tow truck load up what used to be your reliable Tuesday morning commute companion.
You’ve done the immediate stuff, right? Called 911, exchanged insurance information, took those blurry photos with hands that wouldn’t quite cooperate. The police officer was nice enough, the other driver seemed genuinely sorry, and everyone keeps saying “thank God it wasn’t worse.” But here’s the thing nobody prepared you for: that weird feeling creeping in a few hours later.
Maybe it’s your neck feeling a little… off. Or your lower back sending you subtle reminders that something’s not quite right. Could be that headache that won’t budge, or just this general sense that your body went through something it wasn’t designed for. Cars are built to crumple and absorb impact – humans, well, we’re a bit more complicated.
And then someone mentions seeing a doctor. Actually, scratch that – *everyone* mentions seeing a doctor. Your sister calls, your coworker stops by your desk, even your neighbor who witnessed the whole thing suggests it. But here’s where it gets tricky… what kind of doctor? Your family doc is booked solid for three weeks. The ER seems like overkill if you’re walking around. Urgent care feels like the medical equivalent of a band-aid.
Enter the personal injury doctor – a phrase that might sound a little intimidating if you’ve never needed one before. You’re not “injured injured,” right? You’re not on a stretcher or wearing a cast. But here’s what I’ve learned after years of helping people navigate this exact situation: the definition of “injury” after a car accident is way broader than most of us realize.
Your body absorbed forces it was never meant to handle. Think about it – you were traveling at whatever speed (let’s say 35 mph), and suddenly… zero. That energy has to go somewhere, and unfortunately, it goes through you. Sometimes the effects show up immediately – sometimes they’re like that friend who shows up to the party fashionably late.
The truth is, most people have no idea what questions to ask when they’re sitting across from a personal injury specialist for the first time. You’re probably dealing with insurance calls, car rental logistics, and that lovely bureaucratic dance that follows any accident. The last thing you need is to walk out of a medical appointment wishing you’d asked better questions.
That’s exactly what happened to my friend Sarah last year. Rear-ended at a red light, nothing dramatic. She saw a doctor, got checked out, felt pretty good about things. But three months later? Still dealing with headaches that wouldn’t quit and a stiff neck that made her feel about thirty years older. When she finally found the right doctor – and asked the right questions – she discovered she’d been dealing with a mild traumatic brain injury that nobody had properly evaluated.
I’m not trying to scare you here. Most people recover completely from motor vehicle accidents, especially with the right care early on. But the key phrase there is “right care.” And getting the right care means knowing what to ask for, understanding what’s normal versus what’s a red flag, and making sure you’re working with someone who actually gets it.
Because here’s the thing – you shouldn’t have to become a medical expert overnight. You shouldn’t have to figure out the difference between a chiropractor and an orthopedist while you’re still processing what happened. And you definitely shouldn’t have to wonder if that nagging discomfort is just “part of getting older” or something that deserves attention.
So let’s talk about the questions that actually matter. The ones that’ll help you understand what’s happening in your body, what your treatment options really look like, and how to protect yourself both medically and legally. Because the better questions you ask upfront, the better chance you have of getting back to feeling like… well, like yourself again.
The Hidden Complexity of Car Accident Injuries
You know how sometimes you bump your knee on a coffee table, and it doesn’t hurt until the next morning? Car accidents are like that… except multiply the delayed reaction by about a thousand.
The thing is, when you’re in a motor vehicle accident, your body experiences forces it was never designed to handle. Think of it like this – imagine you’re holding a raw egg while riding a roller coaster that suddenly stops. That egg? That’s basically every soft tissue, joint, and organ in your body during impact.
What makes this especially tricky is that adrenaline is an incredibly effective painkiller. Right after an accident, you might feel completely fine – even energized. Your body’s basically running on its own natural morphine. But once that wears off (and it will), you start feeling things you didn’t even know got hurt.
Why “I Feel Fine” Doesn’t Always Mean You Are
Here’s something that catches a lot of people off guard: some of the most serious car accident injuries don’t announce themselves right away. It’s counterintuitive, I know. We’re used to pain being our body’s alarm system – touch something hot, feel pain immediately, pull your hand away.
But soft tissue injuries, concussions, and even some spinal issues can be sneaky. They’re like that friend who seems totally fine at the party but texts you the next day saying they’re never drinking again. The damage happened, but the full impact takes time to reveal itself.
Whiplash is probably the most famous example of this delayed-onset situation. Your head snaps forward and back (or side to side) faster than your muscles can react to protect your neck. The actual injury might happen in milliseconds, but the inflammation, muscle spasms, and pain can take hours or even days to develop.
The Personal Injury Doctor Difference
Now, you might be wondering – can’t I just see my regular doctor? Well, you could. But here’s the thing: treating car accident injuries is kind of like being a detective and a mechanic at the same time.
Personal injury doctors specialize in understanding how accidents happen and what that means for your body. They know that a rear-end collision creates different injury patterns than a T-bone crash. They’re trained to look for subtle signs of problems that might not show up on a standard exam.
Think of it this way – you wouldn’t take your car to just any mechanic after an accident, right? You’d want someone who specializes in collision repair, someone who knows how to spot frame damage that isn’t immediately visible. Personal injury doctors are like the collision specialists for your body.
Documentation: More Important Than You Think
Here’s where things get a bit… well, clinical. But stick with me because this matters for your recovery and any potential insurance claims.
Personal injury doctors don’t just treat you – they document everything. Every symptom, every test, every treatment plan gets recorded in detail. This isn’t just good medicine (though it is that too). It’s also protection for you down the road.
Insurance companies – and I’m not trying to villainize them here, they’re just doing their job – will question everything. They’ll want proof that your injuries are real, that they’re related to the accident, and that your treatment is necessary. Without proper documentation, you might find yourself in the frustrating position of having real symptoms but no way to prove they’re connected to your accident.
The Treatment Philosophy Difference
Regular doctors are trained to treat symptoms and get you back to baseline health. Personal injury doctors think bigger picture. They’re not just asking “How do we stop the pain?” They’re asking “How do we restore this person to their pre-accident quality of life?”
That might mean considering how your injuries affect your job, your hobbies, your sleep, your relationships. They understand that healing from a car accident isn’t just about fixing what’s broken – it’s about helping you reclaim your normal life.
Actually, that reminds me… many people don’t realize that car accident injuries can affect things like concentration, mood, and energy levels. Your personal injury doctor will be looking for these connections too, not just the obvious physical symptoms.
What to Bring to Your First Appointment (Beyond the Obvious)
Sure, you’ll grab your insurance cards and ID – everyone knows that. But here’s what most people forget: bring a written timeline of everything that happened after the accident. I’m talking about when the pain started, when it got worse, what positions make it better or worse… even if it seems minor.
Your doctor isn’t psychic. That nagging headache you dismissed as stress? Write it down. The shoulder stiffness that didn’t show up until day three? Crucial information. Think of yourself as a detective gathering evidence – because honestly, that’s exactly what you’re doing.
Also – and this might sound weird – bring someone with you if possible. After trauma, your brain isn’t always firing on all cylinders. You might forget half of what the doctor says, or miss important details about follow-up care. A second set of ears? Invaluable.
How to Describe Your Pain (When Words Feel Inadequate)
“It hurts” tells your doctor almost nothing useful. Pain has personality – is it sharp like a knife? Dull and achy like you’ve been carrying heavy boxes all day? Does it throb with your heartbeat or feel like someone’s squeezing you in a vice?
Here’s a trick from experienced patients: use the 1-10 pain scale, but be honest about your baseline. If you’re someone who rarely complains about pain, your “6” might be another person’s “9.” Tell your doctor this context.
Keep a pain diary between appointments. Note what makes it worse (sitting too long, cold weather, stress), what helps (heat, certain positions, movement), and how it changes throughout the day. Your neck might feel fine in the morning but turn into a brick by afternoon – that pattern tells a story.
Red Flags That Mean “Call Back Immediately”
Your doctor should give you a clear list of warning signs that require immediate attention. Don’t just nod politely – write these down and ask for clarification.
For head injuries, you’re looking for things like persistent vomiting, confusion that gets worse, or severe headaches that don’t respond to medication. With neck and back injuries, watch for numbness or tingling that travels down your arms or legs, sudden weakness, or bowel/bladder changes.
But here’s what they might not tell you: trust your gut. If something feels “off” in a way you can’t quite articulate, that’s worth a phone call. You know your body better than anyone else.
The Insurance Documentation Game (Play It Smart)
Every appointment generates paperwork that might matter later – not just for your current treatment, but potentially for legal proceedings. Ask for copies of everything. Treatment notes, test results, referral letters… all of it.
Your doctor’s office probably has a patient portal where this stuff lives digitally. Set it up immediately. Screenshots of your treatment timeline could become incredibly important if your case drags on for months or years.
Also, ask about something called “maximum medical improvement” – the point where you’ve healed as much as you’re going to heal. This becomes crucial for insurance settlements, and you want to understand what it means before you reach that point.
Questions That Separate Good Doctors from Great Ones
Here’s where you dig deeper than “Will I get better?” Ask about your specific restrictions – can you lift your toddler? Drive long distances? Sleep on your side? The devil’s in these details.
Push for timelines, even rough ones. “When might I expect to see improvement?” isn’t a guarantee you’re seeking – it’s planning information you need for work, childcare, daily life.
And this one’s important: “What happens if I’m not improving as expected?” Great doctors have backup plans. They think three moves ahead, like chess players. If physical therapy isn’t cutting it after six weeks, what’s next? Injections? Different imaging? Specialist referrals?
Building Your Medical Paper Trail
Every conversation matters now. After each appointment, send a follow-up email summarizing what you discussed. Something simple: “Just confirming that we talked about starting physical therapy twice weekly and that I should call if the headaches worsen.”
This isn’t about being difficult – it’s about creating a documented record of your care. Memory fades, especially when you’re dealing with pain and stress. But emails? They stick around forever, creating a timeline that insurance companies and potentially lawyers can follow.
Your future self will thank you for this attention to detail. Trust me on this one.
The Insurance Maze – When Your Doctor’s Recommendations Hit a Wall
Here’s what nobody tells you about car accident injuries: your doctor might recommend the perfect treatment plan, but your insurance company? They’re playing a completely different game.
You’ll walk out of that appointment feeling hopeful – finally, someone has a plan to get you better. Physical therapy twice a week, maybe some imaging, perhaps a specialist referral. Then reality hits when you call to schedule that first PT session and hear those dreaded words: “We need prior authorization.”
The solution isn’t to give up (though you’ll want to). Ask your doctor’s office about their prior authorization process upfront. Many practices have dedicated staff who handle insurance battles – they know which codes to use, which documentation insurance companies demand. If your doctor seems fuzzy on insurance details, that’s actually a red flag. The best injury docs have this process down to a science because they deal with it every single day.
When Your Body Doesn’t Follow the Textbook Timeline
Your doctor says you should be feeling better in 6-8 weeks. Week 10 rolls around and you still can’t turn your head without wincing. Now what?
This is where a lot of people panic – and honestly, rightfully so. You start wondering if something’s seriously wrong, if you’re being dramatic, or if your doctor missed something important. The truth is, healing is messy and unpredictable, especially after trauma.
Don’t suffer in silence or assume you’re “failing” somehow. Schedule that follow-up appointment even if it feels too soon. Come prepared with specifics: “I still can’t lift my left arm above shoulder height” is infinitely more useful than “I still hurt.” Keep a pain diary if you need to – it sounds tedious, but patterns emerge that you might miss otherwise.
And here’s something your doctor should tell you but might not: sometimes the initial treatment plan needs a complete overhaul. That’s not a failure of medicine – it’s just how bodies work sometimes.
The Documentation Dilemma That Haunts Legal Cases
If you’re thinking about a personal injury claim (or already pursuing one), there’s this weird tension between getting better and… well, proving how hurt you were. It feels wrong to focus on your pain when you’re trying to heal, but inadequate documentation can torpedo your case later.
Your doctor needs to understand this balance. Ask them directly: “How detailed should I be about my symptoms? What should you be documenting for potential legal purposes?” A good injury doctor will know exactly what you mean – they’ve walked this tightrope with hundreds of patients.
Be honest about everything, even the weird stuff that seems unrelated. That headache that started three days after the accident? That sudden anxiety when driving? Your sleep problems? All of it matters, both medically and legally. Your body doesn’t compartmentalize trauma the way insurance forms do.
When Multiple Specialists Start Contradicting Each Other
You know what’s worse than having no answers? Having three different doctors give you three different answers. The orthopedist says your back pain is muscular. The neurologist thinks it might be nerve-related. Your primary care doctor suggests it’s stress.
This isn’t uncommon – it’s actually pretty typical with complex injuries. Bodies are complicated, and car accidents create complicated problems. The key is finding one doctor who can serve as your quarterback, someone who communicates with your other providers and helps synthesize all the different opinions.
Ask your primary injury doctor: “Who’s coordinating my care? How do you communicate with my other specialists?” If they look blank or give you a vague answer, you might need to be your own advocate here. Request that all your doctors send reports to each other. Create a simple timeline of your treatments and share it with each provider.
The Financial Reality Check
Let’s be brutally honest – medical care after an accident gets expensive fast. Even with insurance, you’re looking at copays, deductibles, and those sneaky “balance billing” charges that show up months later.
Before you agree to any treatment plan, ask the hard money questions: “What’s this going to cost me out of pocket? Are there payment plans? If insurance denies something, what are my options?”
Some doctors’ offices offer payment plans or sliding scale fees for accident victims. Others work directly with personal injury attorneys on a lien basis – meaning you don’t pay until your case settles. These aren’t conversations anyone wants to have when they’re hurt and scared, but avoiding them makes everything worse later.
The best injury doctors understand the financial stress their patients face. If your doctor seems annoyed or dismissive when you bring up cost concerns… maybe it’s time to find someone who gets it.
What’s Realistic? Setting the Right Expectations
Let’s be honest – healing isn’t like the movies where someone gets in a massive car wreck and walks away with just a tiny bandage on their forehead. Real recovery takes time, and it’s rarely a straight line from injured to completely better.
Most soft tissue injuries (think whiplash, muscle strains, minor sprains) start showing improvement within a few days to a week, but that doesn’t mean you’re good as new. You might feel better one day, then wake up stiff and sore the next. That’s… actually pretty normal. Your body’s doing this complex healing dance, and sometimes it stumbles a bit.
For more significant injuries – fractures, disc problems, or anything requiring surgery – you’re looking at weeks to months. I know that sounds overwhelming when you just want to get back to your regular life. But here’s the thing: your doctor isn’t trying to string you along. They’re giving you realistic timelines based on how bodies actually heal, not how we wish they’d heal.
The tricky part? Every person heals differently. Your coworker might’ve bounced back from their fender-bender in two weeks, while you’re still dealing with headaches a month later. That doesn’t mean something’s wrong with you – it just means you’re… well, you’re not your coworker.
The Follow-Up Dance (And Why It Matters)
Your initial visit is just the opening act. Most personal injury cases involve a series of follow-ups, and yes, this can feel tedious when you’re juggling work, insurance calls, and trying to get your car fixed.
Typically, you’ll see your doctor again within a week or two of your first visit. They’re checking if your treatment plan is working, if new symptoms have popped up (which happens more often than you’d think), and whether you need any adjustments to your care.
During these follow-ups, don’t just nod and say “fine” when they ask how you’re doing. This is your chance to mention that weird shooting pain that started yesterday, or that your sleep has been terrible, or that you can’t turn your head to check your blind spot anymore. These details matter – both for your recovery and for any legal proceedings.
Some patients need weekly visits initially, others might space them out to every few weeks. It depends on your specific injuries and how you’re responding to treatment. Don’t worry if your schedule looks different from what you expected… your body gets to set the pace here, not your calendar.
When Things Don’t Go According to Plan
Sometimes – and I hate that this happens – recovery hits unexpected bumps. Maybe that nagging back pain isn’t improving like it should. Or perhaps you develop new symptoms weeks after the accident (yes, that’s a real thing that can happen).
This doesn’t mean your doctor missed something or that you’re “broken.” Car accidents can trigger a cascade of issues that don’t always show up immediately. Your body might compensate for one injury by overusing other muscles, creating new problem areas. It’s like when you favor one leg after hurting your ankle – suddenly your hip starts aching too.
If your recovery stalls or takes an unexpected turn, your doctor might recommend additional imaging, refer you to a specialist, or adjust your treatment plan. This isn’t failure – it’s medicine adapting to what your body is telling them.
Planning for the Paperwork Mountain
Here’s something nobody warns you about: the documentation. Oh my goodness, the documentation. You’ll need medical records for insurance claims, possibly for legal proceedings, and definitely for your own peace of mind.
Keep a simple log of your symptoms, treatments, and how you’re feeling day-to-day. Nothing fancy – even notes in your phone work. “Tuesday – headache all morning, physical therapy at 2pm, felt looser afterward but tired.” This kind of record can be incredibly helpful later, especially if there are disputes about your treatment or recovery timeline.
Your doctor’s office will handle the official medical documentation, but having your own record helps you remember details during appointments and gives you a clearer picture of your progress (or lack thereof).
Most importantly? Be patient with yourself. Recovery isn’t a race, and there’s no prize for pushing through pain just to get back to “normal” faster. Your body has been through something traumatic – give it the time and care it needs to heal properly.
You know what? Getting injured in a car accident is like being thrown into a world you never asked to enter. One minute you’re just driving to work or picking up groceries, and the next… everything’s different. Your body hurts in ways you didn’t know were possible, insurance companies are calling, and suddenly you’re supposed to become an expert on medical terminology and legal processes.
It’s overwhelming – and that’s putting it mildly.
But here’s something I’ve learned from working with countless people who’ve been exactly where you are right now: you don’t have to navigate this alone. Those questions we talked about? They’re not just items to check off a list. They’re your roadmap to getting the care you actually need, not just the care that’s convenient for everyone else.
The right doctor won’t rush you through these conversations. They won’t make you feel silly for asking about that weird tingling in your fingers or whether it’s normal to feel this exhausted three weeks after the accident. Actually, the best ones? They’ll be relieved that you’re asking these questions. It shows you’re taking your recovery seriously.
And let’s be honest about something else – your body might not bounce back the way it used to. Maybe you’re in your twenties and thought you were invincible, or maybe you’re older and worried this is just “one more thing” to deal with. Either way, getting proper medical attention isn’t about being dramatic or trying to “milk” the situation. It’s about giving yourself the best possible chance to heal.
Sometimes people tell me they feel guilty for taking up the doctor’s time with questions, especially when they’re not sure if something is “worth mentioning.” But here’s the thing – that’s exactly what these appointments are for. Your discomfort matters. Your sleep problems matter. That anxiety you’re feeling when you get behind the wheel? That matters too.
The documentation you create now, the relationships you build with the right medical professionals, the questions you ask… they’re all investments in your future self. The person who’ll be living in your body five, ten, twenty years from now deserves your advocacy today.
Look, I get it if you’re feeling tired of appointments and paperwork and all the administrative chaos that follows an accident. But don’t let that exhaustion keep you from getting the care you need. Your recovery isn’t just about healing from this specific injury – it’s about maintaining your quality of life going forward.
If you’re reading this and thinking, “I wish I had someone who really understood what I’m going through,” – well, that’s exactly why we’re here. We’ve seen how the right medical support can completely change someone’s recovery trajectory. We’ve also seen what happens when people try to tough it out alone.
You deserve comprehensive care from professionals who listen to your concerns and take your recovery seriously. If you’re ready to start asking the right questions and getting the answers you need, we’d love to help. Sometimes the hardest part is just making that first call – but once you do, you’ll have a team in your corner who genuinely cares about getting you back to feeling like yourself again.