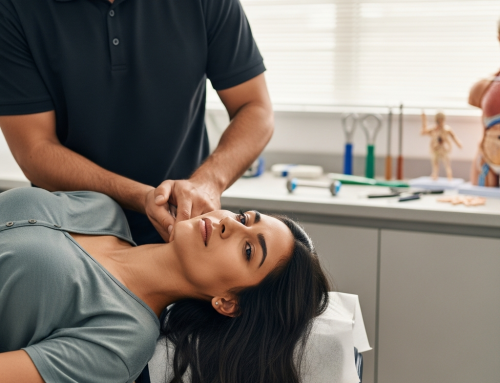
How Is Whiplash From a Car Accident Diagnosed in Irving?
The light turned green, you eased forward through the intersection, and then – WHAM. The world lurched sideways as another driver plowed into your passenger side. Your head snapped like a rag doll, your neck twisted in ways it definitely wasn’t designed for, and suddenly you’re sitting there in your crumpled car thinking, “What the hell just happened?”
If you’re reading this, chances are good that scenario hits a little too close to home. Maybe it wasn’t a side impact – maybe someone rear-ended you while you were stopped at a red light, or perhaps you had to swerve to avoid a deer and ended up in a ditch. The details don’t matter as much as what came after: that creeping realization that something’s not quite right with your neck.
Here’s the thing about whiplash – and I’ve seen this countless times in my years working with accident victims – it’s sneaky. Really sneaky. You might walk away from that crash feeling okay, maybe a little shaken up but nothing major. Then you wake up the next morning and can barely turn your head to check your blind spot. Or maybe the pain hits you three days later while you’re reaching for something on a high shelf. Your body’s been through trauma, and sometimes it takes a while to send up the distress signals.
That’s where things get tricky, especially here in Irving where we’re all juggling busy lives, demanding jobs, and family responsibilities. You’re probably thinking, “Do I really need to see a doctor? It’s just a sore neck. I don’t have time for this.” Trust me, I get it. Medical appointments are expensive, time-consuming, and honestly… kind of scary when you don’t know what to expect.
But here’s what I wish someone had told me after my own fender-bender years ago: getting properly diagnosed isn’t just about documenting your injuries for insurance purposes (though that’s important too). It’s about understanding what’s actually happening in your body so you can heal properly – and avoid those lingering issues that can plague you months or even years down the road.
You see, whiplash isn’t just one thing. It’s actually an umbrella term that covers a whole range of neck injuries, from simple muscle strains to more complex ligament damage or even herniated discs. The pain you’re feeling? That could be coming from anywhere – your muscles, your joints, your nerves, or some combination of all three. And without proper diagnosis, you’re basically flying blind when it comes to treatment.
I’ve watched too many people try to tough it out, hoping their neck pain would just… disappear. Some get lucky. Others? Well, they end up dealing with chronic headaches, persistent neck stiffness, or that nagging shoulder pain that never quite goes away. The worst part is, many of these long-term problems could have been prevented with the right care early on.
Living in Irving, you’ve got options – more medical facilities than you can shake a stick at, from urgent care clinics to specialized orthopedic practices. But knowing where to go and what to expect? That’s where things get overwhelming. Do you start with your family doctor? Head straight to the emergency room? What about those imaging tests everyone talks about – which ones do you actually need?
And let’s be real about the elephant in the room: dealing with insurance companies. They’re going to want documentation, medical records, proof that your injuries are legitimate. Having a proper diagnosis isn’t just about your health – it’s about protecting your financial future too.
In the next few minutes, we’re going to walk through everything you need to know about getting a whiplash diagnosis right here in Irving. We’ll talk about what actually happens during those medical appointments (spoiler: it’s not as intimidating as you think), which tests your doctor might recommend and why, and how to navigate the local healthcare system without losing your sanity.
More importantly, we’ll cover the red flags that mean you need medical attention right now – not next week, not when it’s convenient – because some neck injuries don’t announce themselves with obvious symptoms. Your future self will thank you for reading this.
What Actually Happens When Your Neck Gets Whipped Around
Think of your neck like a garden hose with a bowling ball balanced on top. When your car suddenly stops but your body keeps moving forward – that’s your head (the bowling ball) whipping back and forth on your neck (the hose). Except, you know, with muscles, ligaments, and nerves that weren’t designed for that kind of violent motion.
The thing is, whiplash isn’t really one injury – it’s more like a constellation of problems that happen when your neck gets yanked beyond its normal range of motion. Your cervical spine (that’s the fancy term for your neck bones) has seven vertebrae stacked up like Jenga blocks, and they’re held together by a complex web of muscles, ligaments, and tendons. When everything gets stretched, twisted, or compressed in ways it shouldn’t… well, that’s when things start to hurt.
Why Your Body Doesn’t Always Send the Memo Right Away
Here’s something that catches a lot of people off guard – you might walk away from a fender bender feeling totally fine, only to wake up the next morning feeling like you got tackled by a linebacker. This delayed reaction isn’t in your head (pun intended).
Your body’s pretty smart about managing crisis situations. Right after an accident, adrenaline floods your system, acting like nature’s painkiller. Plus, inflammation takes time to build up – think of it like how a twisted ankle doesn’t reach peak swelling for several hours. Your neck tissues might be damaged, but the full extent of that damage doesn’t always announce itself immediately.
Sometimes symptoms don’t show up for 24-48 hours, which is why doctors always recommend keeping an eye on how you feel in the days following an accident, even if you initially felt okay.
The Tricky Thing About Neck Injuries
Your neck is basically the highway between your brain and the rest of your body. All those nerves running through your cervical spine don’t just control neck movement – they branch out to your shoulders, arms, and hands. So whiplash can cause symptoms that seem completely unrelated to your neck at first glance.
You might experience headaches (because neck muscles connect to your skull), shoulder pain, tingling in your fingers, or even dizziness. It’s like when you have a computer problem – sometimes the issue is with the hard drive, but the symptom shows up as a frozen screen. The source and the symptom aren’t always in the same place.
What Makes Diagnosis Challenging
Here’s where things get a bit frustrating for patients – and honestly, for doctors too. Unlike a broken bone that shows up clear as day on an X-ray, soft tissue injuries like whiplash are masters of hide-and-seek. Standard X-rays are great at spotting fractures or major structural problems, but they can’t see muscle strains, ligament sprains, or inflamed tissues.
This means your doctor has to be part detective, piecing together clues from your symptoms, physical examination, and sometimes more advanced imaging. It’s not that they don’t believe you when you say you’re in pain – it’s that the tools for visualizing soft tissue damage are more complex and sometimes less definitive.
Beyond Just “Neck Pain”
The symptoms of whiplash can be surprisingly varied, which is part of what makes diagnosis tricky. Sure, neck pain and stiffness are the obvious ones, but you might also deal with
– Headaches that seem to start at the base of your skull – Shoulder blade pain that makes it hard to concentrate at work – Arm pain or numbness that has you wondering if something’s seriously wrong – Fatigue that goes beyond just being tired from dealing with insurance companies – Difficulty concentrating (sometimes called “whiplash brain fog”)
Some people even experience jaw pain or ringing in their ears. Your body is an interconnected system, and when one part gets disrupted, the effects can ripple outward in unexpected ways.
The key thing to remember? Every person’s whiplash experience is different. What affects your coworker one way after their accident might affect you completely differently. That’s not weird or wrong – that’s just how individual our bodies and healing processes are.
Getting Ready for Your Whiplash Evaluation
Here’s something most people don’t realize – how you prepare for your whiplash diagnosis can actually affect the accuracy of your results. I always tell patients to keep a detailed pain journal starting immediately after their accident. And I mean detailed. Note when the pain is worst (often it’s first thing in the morning), what makes it better or worse, and any weird symptoms you might brush off as unrelated.
That tingling in your fingers? Write it down. The headaches that seem to come out of nowhere? Document them. Sleep problems, difficulty concentrating, even feeling more irritable than usual – it all matters. Your doctor needs the full picture, not just “my neck hurts.”
Actually, that reminds me… many patients worry they’ll sound dramatic or be labeled as complainers. Trust me, whiplash is tricky precisely because symptoms can seem scattered or delayed. Your medical team has seen it all before.
What to Expect During Physical Examination
The physical exam for whiplash isn’t just about your neck – though that’s obviously the main event. Your doctor will check your range of motion, asking you to slowly turn your head side to side, up and down. Don’t push through severe pain to “prove” you’re tough. This isn’t a fitness test.
They’ll also check your reflexes, muscle strength, and examine your shoulders and upper back. Whiplash has this sneaky way of affecting areas you wouldn’t expect. Sometimes the pain radiates down to your shoulder blades or causes tension headaches that feel completely separate from your neck injury.
Here’s a tip most people miss: mention any changes in your grip strength or coordination. Can you still open jars easily? Having trouble with buttons or your phone’s touchscreen? These details help doctors understand if nerve function has been affected.
Imaging Tests – When and Why
Not everyone with whiplash needs an MRI right away, despite what you might think. X-rays are usually first – they’re quick, relatively inexpensive, and rule out fractures or major structural problems. But here’s the thing about whiplash: it’s primarily a soft tissue injury, which means regular X-rays might look completely normal even when you’re in significant pain.
If your symptoms persist beyond a few weeks or you’re experiencing neurological symptoms like numbness, tingling, or weakness, that’s when your doctor might order an MRI. This gives us the detailed view of your muscles, ligaments, and discs that we need.
CT scans fall somewhere in between – they’re sometimes used if there’s concern about more complex injuries, especially if you hit your head during the accident or lost consciousness.
Specialized Tests You Might Encounter
Sometimes standard imaging isn’t enough to get the full picture. Dynamic X-rays – where you’re asked to bend your neck forward and backward during the X-ray – can reveal instability that wouldn’t show up otherwise. It sounds scarier than it is, and you’re in complete control of the movement.
Nerve conduction studies might come up if there’s concern about nerve damage. These measure how well electrical signals travel through your nerves. They’re not particularly comfortable – think of it like getting multiple small shocks – but they provide crucial information about nerve function.
Red Flags That Need Immediate Attention
While most whiplash injuries heal with proper treatment, there are certain symptoms that mean you need to be seen immediately – like, drop everything and go to the ER immediately. Severe headaches that keep getting worse, vision changes, difficulty swallowing, or numbness/tingling that’s spreading or getting more intense.
If you’re having trouble staying awake, feeling confused, or experiencing nausea and vomiting hours or days after your accident, don’t wait. These could indicate a more serious injury that needs urgent evaluation.
Working with Irving’s Medical System
Irving has several excellent facilities for whiplash diagnosis, but here’s something that might save you time and frustration: call ahead and ask specifically about their experience with car accident injuries. Some urgent care centers are fantastic for basic evaluation, while others might refer you out immediately.
If you’re dealing with insurance (and let’s face it, you probably are), ask about getting copies of all your medical records and imaging results. Having your own complete file makes it much easier if you need to see specialists or get a second opinion later. Most places can put everything on a CD or secure online portal – just ask when you check out.
The key is being your own advocate while staying organized and honest about your symptoms. Your recovery starts with getting an accurate diagnosis.
When the Insurance Company Becomes Your Biggest Headache
Here’s what nobody tells you about whiplash diagnosis – dealing with insurance can be more painful than your actual neck injury. They’ll want documentation for everything, and I mean *everything*. That “I feel fine” comment you made at the accident scene? Yeah, they’ve got that recorded.
The solution isn’t to panic, but to be strategic. Start documenting your symptoms immediately, even if they seem minor. Keep a daily symptom diary – when pain flares up, what makes it worse, how it affects your sleep. Insurance adjusters love concrete data, and honestly… your memory of day three isn’t going to be crystal clear when you’re filing paperwork three weeks later.
The “But You Look Fine” Problem
This one’s brutal. Whiplash doesn’t come with a cast or visible bruising, so everyone – including some medical professionals – might minimize what you’re experiencing. Your boss expects you back at work, your family doesn’t understand why you can’t turn your head to check blind spots while driving.
The trick is finding a doctor who specializes in soft tissue injuries and actually *listens*. Not every physician has extensive experience with whiplash – it’s not exactly the most glamorous specialty. Look for someone who uses comprehensive diagnostic tools, not just a quick physical exam. And don’t be afraid to advocate for yourself. If a doctor dismisses your symptoms, get a second opinion. Your pain is real, regardless of what shows up on initial X-rays.
The Waiting Game That Tests Your Sanity
Whiplash symptoms can take 24-72 hours to fully develop. Sometimes longer. This delay creates a perfect storm of doubt – both in yourself and from others. You might start questioning if you’re really hurt, especially when that first day you felt… okay, maybe?
Actually, that reminds me of what one of my patients told me – she almost didn’t seek treatment because she felt “dramatic” for complaining about pain that didn’t start immediately. Don’t fall into this trap. The delayed onset is *classic* whiplash behavior. Your body was in shock, adrenaline was pumping, and your muscles were compensating in ways you couldn’t feel initially.
Schedule that medical appointment even if you’re not sure you need it. It’s easier to cancel an unnecessary appointment than to explain to insurance why you waited a week to seek treatment.
When Multiple Doctors Give Different Opinions
Oh, this one’s fun. Doctor A says it’s mild strain, take some ibuprofen. Doctor B wants extensive imaging. Doctor C mentions potential TMJ complications. You’re sitting there like, “Guys, it’s the same neck we’re all looking at.”
Different medical specialties focus on different aspects of whiplash. Your primary care doctor might focus on immediate pain management, while an orthopedist is thinking about structural damage, and a neurologist is considering nerve involvement. None of them are necessarily wrong – they’re just looking through different lenses.
The solution? Ask each doctor to explain their specific concerns and recommendations. Write it down (trust me, you won’t remember everything). Then find a healthcare provider who can coordinate your care and help you make sense of potentially conflicting advice. Sometimes that’s a physiatrist – they specialize in the whole picture of injury recovery.
Fighting the “It’s All in Your Head” Battle
Here’s the harsh reality – some people will think you’re exaggerating. Maybe it’s the insurance adjuster, maybe it’s your employer, maybe it’s that one family member who has opinions about everything. Chronic pain from whiplash can last months, and not everyone understands that.
Document everything, but also… give yourself permission to not justify your pain to everyone. Focus your energy on working with medical professionals who take your symptoms seriously. Join support groups if you need validation from people who actually get it. And remember – the goal isn’t to prove how much pain you’re in, it’s to get better.
The Treatment Maze
Physical therapy, chiropractic care, massage therapy, injections, medications – the treatment options can feel overwhelming. Plus, everyone has an opinion about what worked for their cousin’s neighbor’s sister.
Start with conservative treatments, but don’t suffer unnecessarily. If basic physical therapy isn’t helping after a reasonable trial period, speak up. Some people need more intensive intervention. Others respond better to alternative approaches. Your treatment plan should evolve based on your actual progress, not some predetermined timeline.
The key is finding providers who communicate with each other and with you about what’s working and what isn’t.
What to Expect During Recovery
Here’s the thing about whiplash – it’s not like a broken bone where you can point to an X-ray and say “there, it’ll be healed in six weeks.” Your neck is a complex system of muscles, ligaments, and joints that all need time to calm down and repair themselves. And honestly? That timeline can be frustratingly unpredictable.
Most people start feeling better within a few days to a couple of weeks. But – and this is important – “feeling better” doesn’t necessarily mean “completely healed.” You might have days where you wake up thinking you’ve turned a corner, only to have your neck remind you otherwise by afternoon. That’s completely normal, even if it’s annoying as hell.
Some folks deal with symptoms for several months. I know that sounds daunting, but it doesn’t mean you’ll be miserable the whole time. Recovery tends to happen in waves – good days and not-so-good days, with the good ones gradually outnumbering the bad ones.
Your Treatment Plan Moving Forward
Your doctor will likely start you with conservative treatments first. Think of it as giving your body the best possible environment to heal itself. This usually means a combination of rest (but not complete immobility – that actually makes things worse), ice or heat therapy, and gentle movement as tolerated.
Physical therapy often becomes your best friend during recovery. A good PT will teach you exercises that feel almost ridiculously simple at first… but trust the process. Those gentle neck stretches and posture corrections? They’re doing more work than you realize. You’re basically retraining your muscles to support your head properly again.
Pain medication might be part of the equation too. Don’t be a hero about this – if your doctor prescribes something to help manage the pain, use it wisely. Being in constant pain actually slows down healing because your muscles stay tense and guarded.
When to Be Concerned
Most whiplash follows a predictable pattern of improvement, but there are some red flags that mean you need to get back to your doctor sooner rather than later. If your pain is getting significantly worse instead of gradually better, that’s worth a conversation. Same goes for new symptoms like tingling in your arms, severe headaches that won’t respond to usual treatments, or any numbness.
Memory problems or difficulty concentrating that persist beyond the first week or two? Don’t brush those off as stress. Sometimes whiplash can affect more than just your neck, and your doctor needs to know about these changes.
The Insurance Dance
Let’s talk about something nobody warns you about – dealing with insurance companies. Whether it’s your auto insurance, health insurance, or the other driver’s insurance, you’re probably going to spend more time on the phone than you’d like. Keep detailed records of everything: every doctor visit, every treatment, every day you miss work because of symptoms.
Insurance companies often want to settle quickly, sometimes before you fully understand the extent of your injuries. While I can’t give legal advice, I can tell you that many people benefit from consulting with a personal injury attorney, especially if your symptoms are affecting your work or daily life significantly.
Getting Back to Normal Activities
The million-dollar question everyone asks: “When can I get back to my regular routine?” The honest answer is that it depends on what your regular routine looks like. If you work at a desk, you might be able to return to work fairly quickly with some modifications – maybe a different chair, frequent breaks to move around, or working from home temporarily.
If your job involves physical labor or you’re an athlete, the timeline will likely be longer. Your body needs time to rebuild strength and trust in movement again. Pushing too hard too fast often leads to setbacks that end up extending your recovery time.
Start slowly with activities you enjoy. Maybe that means shorter gym sessions with lighter weights, or taking breaks during long drives. Your neck will let you know when it’s ready for more – you just have to listen to it.
The key is patience with yourself. Recovery isn’t always linear, and that’s okay. Some days will feel like progress, others might feel like you’re moving backward. Both are normal parts of the healing process, frustrating as that might be.
Getting that proper diagnosis after a car accident… it’s honestly one of the best things you can do for yourself. I know it feels overwhelming when you’re dealing with insurance calls, car repairs, and – oh yeah – trying to figure out if that nagging neck pain is actually something serious. But here’s the thing: your body’s been through trauma, even if it was “just” a fender-bender.
Trust What Your Body Is Telling You
You know that feeling when something’s just… off? Maybe you woke up the day after your accident and couldn’t turn your head quite right. Or perhaps it took a few days for the stiffness to really set in. That’s your body sending you a message, and it’s worth listening to.
The diagnostic process we’ve talked about – from those initial physical exams to X-rays, MRIs, and sometimes CT scans – isn’t just medical protocol. It’s your roadmap to understanding what’s actually happening in your neck and spine. Because here’s what I’ve learned: guessing about whiplash is like trying to fix your car engine by listening to it from the driveway. You might get lucky, but you’re probably missing something important.
You’re Not Being Dramatic
Let me say this clearly – seeking medical attention after a car accident doesn’t make you dramatic or weak. I’ve seen too many people brush off their symptoms, thinking they should just “tough it out.” Then three months later, they’re dealing with chronic headaches, shoulder pain, or that frustrating brain fog that makes work feel impossible.
The medical professionals in Irving – whether you’re seeing your primary care doctor, visiting an urgent care center, or working with a specialist – they’ve seen this before. They understand that whiplash isn’t always obvious right away, and they know how to look for the signs your body might be trying to hide.
Your Recovery Starts With Knowledge
Getting an accurate diagnosis is like having a good map before you start a road trip. You wouldn’t drive from Dallas to Denver without knowing which highways to take, right? Same principle applies here. Understanding exactly what’s injured, how severe the damage is, and what your treatment options look like – that’s how you set yourself up for the best possible recovery.
And recovery… it’s not just about the physical stuff. When you know what you’re dealing with, you can make informed decisions about work, exercise, even simple daily activities. No more wondering if that shooting pain is normal or if you should be worried.
We’re Here When You’re Ready
Look, navigating healthcare after an accident can feel like learning a new language while you’re already stressed and hurting. If you’re feeling lost in the process – whether you need help understanding your diagnosis, exploring treatment options, or just want someone to explain what all those medical terms actually mean – that’s exactly what we’re here for.
You don’t have to figure this out alone. Sometimes having someone in your corner who understands both the medical side and the very human side of recovery makes all the difference. Give us a call when you’re ready to take that next step toward feeling like yourself again.