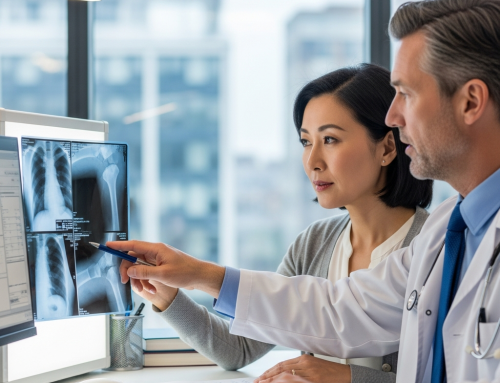
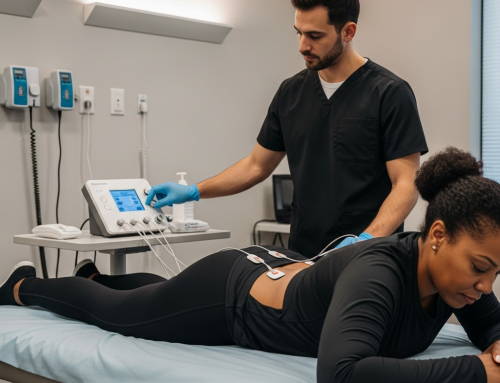
You’re sitting at a red light, maybe scrolling through your phone or adjusting the radio, when BAM – someone rear-ends you. Your head snaps forward, then back against the headrest. For a moment, you’re stunned. Then comes that rush of adrenaline as you check if everyone’s okay, exchange insurance info, and deal with the aftermath.
But here’s the thing that catches most people off guard… you feel fine. Maybe a little shaken up, sure, but physically? You’re good. You tell the paramedics you don’t need to go to the hospital. You drive home, grateful it wasn’t worse.
Fast forward to the next morning – or sometimes even a few days later – and suddenly you can barely turn your head to check your blind spot. That dull ache in your neck has blossomed into something that makes you wince every time you look over your shoulder. Welcome to the sneaky world of delayed-onset neck injuries.
Why Your Body Plays Hide and Seek After an Accident
Here’s what nobody really prepares you for: your body is kind of a liar in the immediate aftermath of a car accident. All that adrenaline flooding your system? It’s basically nature’s morphine, masking pain and making you feel invincible when you’re actually anything but. It’s like your body’s way of getting you through the crisis, but the bill comes due later.
I’ve seen this scenario play out countless times – and honestly, I’ve lived it myself. That moment when you realize something’s not right, but you’re second-guessing yourself because you felt “fine” right after the accident. You start wondering if you’re being dramatic, if it’s all in your head, or if you should just tough it out.
The truth is, neck injuries from car accidents are incredibly common, even in what seem like minor fender-benders. Your neck – this delicate structure that’s basically holding up a bowling ball (your head) on top of your spine – takes a beating when forces suddenly change direction. And unlike a broken bone that’s obviously broken, neck injuries can be subtle, sneaky little things that announce themselves gradually.
The Stakes Are Higher Than You Think
Now, before you start spiraling into worst-case-scenario thinking, let me be clear – most neck injuries from car accidents do heal with proper care. But here’s why paying attention to the early warning signs matters so much: what you do in those first few days and weeks can make the difference between a full recovery and dealing with chronic pain down the road.
Think about it this way – if you sprained your ankle, you’d probably rest it, ice it, maybe see a doctor. But with neck pain after an accident, people often just… carry on. They go to work the next day, sleep in weird positions trying to get comfortable, and hope it goes away on its own. Sometimes it does, but sometimes those early symptoms are your body’s way of waving a red flag.
The thing that really gets me is how many people dismiss their symptoms because they don’t fit the dramatic movie version of a neck injury. You know, where someone’s in a neck brace immediately after the accident? Real life is messier than that. Real neck injuries often start small – a little stiffness here, some tension there – before potentially developing into something more serious.
What You’re About to Learn (And Why It Matters)
In this article, we’re going to walk through seven key signs that your neck might be injured after a car accident. Some of them are obvious – the kind of pain that makes you immediately think “something’s wrong.” But others? They’re trickier. They might seem unrelated to your neck, or they might feel so minor that you brush them off.
I’ll help you understand what each sign might mean, when it typically shows up (because timing matters more than you’d think), and most importantly – when you should stop wondering and start seeking help. We’ll also talk about why some symptoms can take days or even weeks to appear, because understanding that timeline can save you a lot of unnecessary worry… or help you catch something before it gets worse.
Because here’s what I want you to walk away knowing: trusting your body’s signals isn’t being dramatic. It’s being smart.
Your Neck Wasn’t Built for This
Think about it – your neck is basically seven small bones stacked like building blocks, held together by muscles, ligaments, and a whole lot of hope. It’s designed to let you nod “yes” to that second slice of pizza and shake your head “no” when your friend suggests karaoke. But a car accident? That’s like asking a delicate wine glass to survive a rock concert.
The thing is, your cervical spine (fancy doctor talk for your neck bones) weighs about as much as a bowling ball – around 10 to 12 pounds. Under normal circumstances, those neck muscles handle this weight just fine. But when a car suddenly stops and your body doesn’t… well, that’s when physics becomes very personal.
The Whiplash Phenomenon Everyone Talks About
You’ve probably heard the term “whiplash” thrown around, and honestly, it’s one of those words that sounds almost too simple for what actually happens. Picture cracking a whip – that sharp, sudden motion at the end? Your head does something eerily similar during a collision.
Here’s where it gets counterintuitive though. You’d think the worst damage happens during the initial impact, right? Actually, it’s often the rebound that gets you. Your head snaps forward, then – like a rubber band – whips back in the opposite direction. Sometimes this whole terrible dance happens in less than half a second.
What’s really frustrating (and I hear this from patients all the time) is that you might feel totally fine right after the accident. Your adrenaline is pumping, you’re focused on insurance information and whether everyone’s okay… Meanwhile, those tiny tears in your muscles and ligaments are just getting started.
Beyond the Obvious: Hidden Damage You Can’t See
This is where car accidents get sneaky. Sure, you might have visible bruises from the seatbelt or a bump on your forehead from the airbag. But neck injuries? They’re often invisible troublemakers.
Your cervical discs – think of them as shock absorbers between your vertebrae – can get compressed, bulged, or even herniated. It’s like having a jelly donut that gets squeezed too hard, and now the filling is pushing out where it shouldn’t be. Not a pretty picture, but unfortunately accurate.
Then there are the facet joints (the little connectors between your vertebrae) that can get irritated or inflamed. And don’t get me started on the muscles… some tighten up like they’re protecting Fort Knox, while others decide to just give up entirely.
The Nervous System Gets Involved Too
Here’s something that surprises a lot of people – your neck isn’t just about bones and muscles. It’s basically Grand Central Station for nerves heading to your arms, shoulders, and even parts of your head. When things get jostled around in there, you might end up with symptoms that seem completely unrelated to your neck.
That tingling in your fingers? Could be your neck. Headaches that won’t quit? Yep, possibly neck-related too. It’s like when you have one light switch that mysteriously controls three different rooms – sometimes the connections aren’t what you’d expect.
Why Some People Bounce Back and Others Don’t
This part always puzzles patients, and honestly? It puzzles doctors sometimes too. Two people in the same accident, similar ages, similar builds… one feels better in a week, the other is dealing with pain months later.
Age plays a role – sorry, but those over 40 tend to have a tougher time recovering. Previous neck problems make you more vulnerable too. But here’s the kicker: sometimes it just comes down to how your individual body responds to trauma. Some people’s tissues heal like they have a personal construction crew working overtime. Others… well, their crew apparently takes a lot of coffee breaks.
The position you were in during impact matters enormously. Looking over your shoulder when you got hit? That twist adds a whole extra layer of complexity to the injury pattern.
The Inflammation Factor
After any trauma, your body launches what’s basically an internal emergency response. Inflammation rushes to the scene like EMTs, which is helpful for healing but also creates swelling and pain. Sometimes this response is perfectly proportional to the injury. Other times… it’s like calling in the National Guard to handle a minor fender-bender.
This inflammatory response can take hours or even days to fully kick in, which explains why you might wake up the morning after an accident feeling like you aged 20 years overnight.
What to Do in Those First Critical Hours
You know that moment right after the crash when your adrenaline’s pumping and you’re thinking “I’m fine, I’m totally fine”? Yeah, that’s exactly when you need to slow down and pay attention to your body. Don’t just brush off that slight stiffness – it’s your neck’s way of waving a little red flag.
First things first: ice is your friend, but only for the first 48 hours. We’re talking 15-20 minutes at a time, with a thin towel between the ice pack and your skin. After that? Switch to heat. I can’t tell you how many people get this backwards and wonder why they’re still hurting a week later.
Here’s something most people don’t know – sleeping position becomes absolutely crucial after a neck injury. Ditch the fluffy pillow that seemed so comfortable yesterday. You want something that keeps your neck in neutral alignment… think of it like keeping your head in the same position it would be if you were standing upright.
The Movement Prescription (Yes, Really)
This might sound counterintuitive, but gentle movement is actually better than complete rest. I’m not talking about doing yoga headstands here – just simple, slow neck rotations and shoulder rolls. The key word is *gentle*. If it hurts, back off immediately.
Try this: Every hour or so, slowly turn your head left and right, like you’re shaking your head “no” in slow motion. Then nod up and down – again, slowly. Roll your shoulders backward five times, then forward five times. These tiny movements help prevent your muscles from seizing up completely.
Actually, that reminds me of something important – avoid the temptation to crack or pop your neck. I know it feels like it might provide relief, but you could actually make things worse if there’s already inflammation or instability.
When to Sound the Medical Alarm
Look, I get it. Nobody wants to be that person who rushes to the ER over every little ache. But with neck injuries, there are some red flags that mean you need professional help *now*, not later.
If you’re experiencing any numbness or tingling in your arms or hands – even if it comes and goes – that’s your cue to get checked out immediately. Same goes for any weakness in your grip or difficulty with fine motor tasks like buttoning your shirt.
Severe headaches that weren’t there before the accident? Don’t wait it out. And if you feel dizzy or nauseous… well, those could be signs of a concussion or other complications that definitely need medical attention.
Documentation That Actually Matters
Here’s something they don’t teach you in driver’s ed: Start a pain journal right away. I’m serious about this one. Write down how you’re feeling every morning and evening – pain level on a scale of 1-10, what movements hurt, how your sleep was affected.
Take photos too, even if you don’t see obvious bruising right away. Sometimes swelling and discoloration show up days later, and you’ll want that visual record for insurance purposes. Trust me on this – I’ve seen too many people struggle with claims because they didn’t document things properly from the start.
The Recovery Timeline Reality Check
Everyone wants to know: “How long until I feel normal again?” The honest answer? It varies wildly. Some people bounce back in a few days, others deal with lingering effects for months. Whiplash is notorious for being unpredictable that way.
What I can tell you is that most people see significant improvement within 2-4 weeks if they’re proactive about treatment. But – and this is important – don’t push through severe pain thinking you’re being tough. That’s actually counterproductive and can extend your recovery time.
Building Your Support Team
You might need more than just your regular doctor for this one. A good physical therapist who specializes in auto injuries can work wonders, especially if you start treatment within the first week or two. They know specific techniques for addressing the unique trauma pattern that car accidents create.
Consider massage therapy too, but make sure your therapist has experience with injury recovery. You want therapeutic work, not just relaxation (though honestly, a little relaxation wouldn’t hurt either).
The bottom line? Listen to your body, document everything, and don’t try to tough it out alone. Your neck has been through a trauma – give it the care and attention it needs to heal properly.
The “I Feel Fine” Trap
Here’s what happens more often than anyone wants to admit: you walk away from that fender bender feeling perfectly normal. Maybe a little shaken up, sure, but nothing hurts. Fast-forward 12 hours… and suddenly you can’t turn your head without wincing.
This delayed pain thing? It’s not in your head. When your body goes through trauma – even what seems like minor trauma – it floods with adrenaline and endorphins. These natural painkillers are incredibly effective at masking injury symptoms. Think of them as your body’s emergency response team, keeping you functional when you need to exchange insurance information and deal with tow trucks.
The solution isn’t to assume every minor accident will result in injury, but don’t dismiss symptoms that show up later either. Keep a simple pain diary on your phone for the first week after any collision. Rate your neck stiffness, headaches, or weird sensations on a scale of 1-10. If patterns emerge or things get worse, that’s your cue to seek medical attention.
When Insurance Companies Play Hardball
Let’s talk about something nobody warns you about – dealing with insurance adjusters who act like neck injuries from car accidents are somehow… optional? You’ll hear phrases like “soft tissue injuries heal on their own” or “these symptoms are often psychological.”
This is where things get frustrating fast. You’re dealing with real pain, real limitations, and someone who’s never met you is questioning whether your injury is “legitimate.” Insurance companies have financial incentives to minimize claims – that’s just business reality.
Document everything. And I mean everything. Take photos of vehicle damage (even minor dents can indicate significant force). Keep records of every symptom, every doctor visit, every physical therapy session. Get copies of all medical reports. That headache you’re having? Write it down. The fact that you can’t look over your shoulder while driving? Document it.
Consider getting evaluated by a healthcare provider within the first few days after any accident, even if you feel fine initially. Having that baseline medical record can be crucial if symptoms develop later.
The “Tough It Out” Mentality Problem
Maybe it’s cultural, maybe it’s personal pride, but there’s this weird stigma around neck injuries from car accidents. People worry they’ll be seen as dramatic or money-grabbing if they seek treatment for something that doesn’t show up on X-rays immediately.
Here’s the thing – your cervical spine (that’s your neck) contains some pretty important stuff. Seven vertebrae, multiple muscle groups, ligaments, nerves that control sensation in your arms and hands… it’s not exactly something you want to mess around with.
Whiplash isn’t just “a little soreness.” The sudden back-and-forth motion can cause microscopic tears in muscles and ligaments, irritate nerve roots, and even affect the small joints between vertebrae. These injuries can take weeks or months to fully heal, and without proper treatment, they sometimes don’t heal correctly at all.
Navigating the Medical Maze
Finding the right healthcare provider can feel like solving a puzzle blindfolded. Your primary care doctor might refer you to physical therapy. The physical therapist might suggest you see an orthopedist. The orthopedist orders an MRI that comes back “normal” even though you’re still in pain…
Sound familiar? Different healthcare providers have different areas of expertise. Your family doctor is great for many things, but they might not be the best choice for evaluating complex neck injuries. Consider starting with providers who specifically work with automotive injuries – they understand the mechanics of what happens to your body during a collision and know what to look for.
Don’t be afraid to advocate for yourself. If a provider dismisses your symptoms or suggests that pain lasting more than a few days is “unusual,” get a second opinion. You know your body better than anyone.
The Return-to-Normal Pressure
Friends, family, even healthcare providers sometimes push the “just get back to your regular activities” advice pretty hard. While movement is generally good for healing, there’s a difference between gentle activity and pretending nothing happened.
You might need to modify your workout routine, ask for help with household tasks, or take breaks during your workday. This isn’t permanent, but it’s necessary. Pushing through significant pain often leads to longer recovery times and can sometimes cause additional injury.
The goal isn’t to become sedentary – it’s to find that sweet spot where you’re moving enough to promote healing without aggravating the injury.
What You Can Realistically Expect in the Days Ahead
Here’s the thing nobody tells you about neck injuries after a car accident – they don’t follow a neat, predictable timeline. You’re probably wondering if you’ll wake up tomorrow feeling worse, or if this nagging ache is going to stick around for weeks. Both scenarios? Completely normal.
Most people experience peak pain and stiffness 24-48 hours after the accident. It’s like your neck is on a delayed reaction – initially shocked into numbness, then slowly realizing what just happened. Don’t panic if you felt okay yesterday but can barely turn your head today. Your body’s just… processing.
Mild whiplash typically improves within a few days to two weeks with proper care. You might feel stiff in the mornings, notice some tenderness when checking your blind spot, but overall things should be moving in the right direction.
Moderate injuries – where you’re dealing with significant pain, muscle spasms, or headaches – often take 2-6 weeks to resolve. This is where patience becomes your best friend (and your worst enemy, honestly). Some days you’ll feel great, others you’ll wonder if you’re actually getting better at all.
More severe cases can linger for months, especially if there’s nerve involvement or you’re dealing with disc issues. I know that sounds scary, but remember – even the more stubborn injuries do heal with the right approach and professional guidance.
When to Worry (And When Not To)
You’re going to second-guess every twinge, every new ache – that’s completely human. But here’s when you should actually be concerned: if your pain is getting significantly worse after the first few days, if you develop new neurological symptoms (numbness, tingling, weakness in your arms), or if you’re having trouble with basic functions like sleeping or concentrating.
Sharp, shooting pains down your arms? That’s worth a phone call to your doctor. Mild soreness that comes and goes? Pretty standard territory.
The tricky part is that stress and anxiety can actually make neck pain worse. You’re already dealing with insurance calls, car repairs, maybe missed work… it’s a lot. Your neck muscles are holding all that tension too. Sometimes what feels like your injury getting worse is actually just your nervous system staying on high alert.
Your Next Steps (The Practical Stuff)
First things first – document everything. Take photos of your car, keep track of your symptoms day by day. I know it feels tedious, but future you will thank present you if this becomes an insurance headache.
Week 1-2: Focus on gentle movement and pain management. Ice for the first 48 hours if there’s swelling, then switch to heat. Those over-the-counter pain relievers? They’re your friend right now. Sleep with proper neck support – maybe invest in a cervical pillow if your regular one isn’t cutting it.
Week 2-4: This is typically when you’ll want to consider physical therapy, especially if things aren’t improving as expected. Don’t wait for pain to become unbearable – early intervention usually means better outcomes.
Some people benefit from chiropractic care, others from massage therapy. There’s no one-size-fits-all approach, which can be frustrating when you just want someone to tell you exactly what to do.
Working with Healthcare Providers
Here’s something important – not all healthcare providers are created equal when it comes to car accident injuries. You want someone who understands the specific mechanics of what happens to your neck in a collision, not just general neck pain.
Come prepared with specifics: when does it hurt most? What movements trigger pain? How’s your sleep? Rate your pain levels throughout the day. The more detailed you can be, the better they can help you.
And don’t feel like you need to suffer in silence or “tough it out.” Pain serves a purpose – it’s information. Listen to it, respect it, but don’t let it run your life.
The Mental Game
Nobody talks about this enough, but car accidents mess with your head too. You might find yourself tensing up every time you drive, or feeling anxious about your recovery. That’s not weakness – that’s your brain trying to protect you from future harm.
Take it one day at a time. Some days will be better than others, and that’s okay. Healing isn’t linear, despite what we’d like to believe. Your neck – and the rest of you – will get through this.
You know, after covering all these warning signs, I keep thinking about how isolating it can feel when your body just… isn’t cooperating after an accident. One day you’re fine, the next you’re wincing every time you turn to check your blind spot or struggling to get comfortable at night. It’s frustrating – especially when people around you seem to think you should be “over it” by now.
Here’s what I’ve learned from years of working with people who’ve been through this: your body is trying to tell you something important. Those headaches that won’t quit? The stiffness that makes you move like a robot? The weird tingling in your fingers that comes and goes? None of that is “just in your head” or something you should power through.
Trust What You’re Feeling
The thing about neck injuries – and honestly, trauma in general – is that they don’t follow a neat timeline. You might feel okay immediately after the accident (hello, adrenaline), only to wake up three days later feeling like you’ve been hit by… well, a car. Or symptoms might creep up slowly, so gradually that you start questioning whether they’re even related to the accident.
But here’s the reality: your neck is an intricate network of muscles, ligaments, nerves, and vertebrae. When it gets jolted around – even in what seems like a “minor” fender-bender – things can get knocked out of alignment in ways that don’t show up on a quick X-ray. Sometimes the most significant injuries are the ones you can’t see.
You Don’t Have to Figure This Out Alone
I think one of the hardest parts about dealing with post-accident symptoms is feeling like you need to be your own detective. Googling symptoms at 2 AM, wondering if that new pain is connected to the old pain, trying to decide if you’re being dramatic or if something’s actually wrong…
The truth is, you shouldn’t have to navigate this maze by yourself. Whether you’re dealing with obvious red flags like severe pain and numbness, or more subtle signs like persistent headaches and sleep problems, getting proper evaluation and care isn’t being overdramatic – it’s being smart.
Taking the Next Step
Look, I get it. Maybe you’re worried about costs, or you think it’s “not that bad,” or you’re just tired of dealing with medical stuff. But think about it this way – would you ignore a strange noise your car started making after an accident? Probably not, because you know small problems can become big, expensive problems if left unchecked.
Your neck deserves at least as much attention as your car.
If any of those signs we talked about sound familiar – if you’re nodding along thinking “yeah, that’s me” – consider reaching out to someone who specializes in these kinds of injuries. A good provider will listen to your concerns, take your symptoms seriously, and help you understand what’s happening in your body.
You don’t have to live with the pain, the stiffness, or the worry. And you definitely don’t have to figure it all out on your own. Sometimes the bravest thing you can do is ask for help – especially when your body is asking for it too.