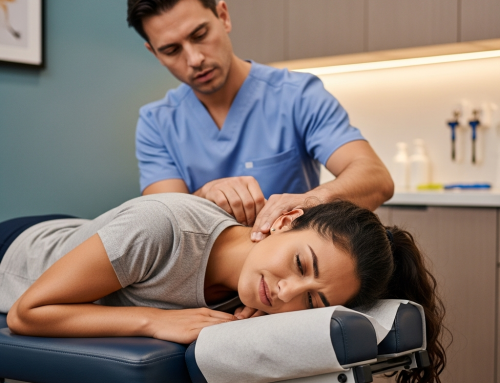
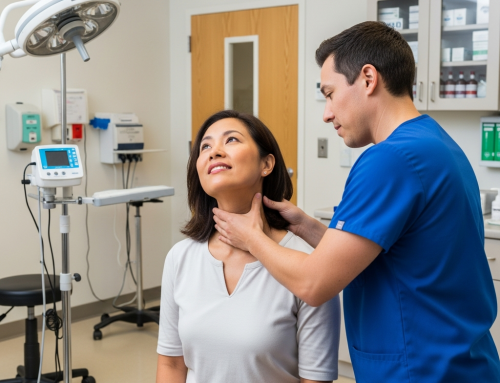
Should I See an Automobile Accident Doctor After Minor Symptoms in Irving?

You’re sitting at a red light, scrolling through your phone (we’ve all been there), when *THUNK* – someone rear-ends you. Your coffee spills a little, you exchange insurance info, and honestly? You feel fine. Maybe your neck’s a tiny bit stiff, but nothing a hot shower won’t fix, right?
Fast-forward three days. You wake up and your neck feels like it’s been twisted into a pretzel. Your lower back is screaming every time you bend over to pick up your keys. And that headache that’s been lurking since yesterday? It’s now pounding like a construction crew decided to renovate your skull.
Sound familiar? Here’s the thing – and this might surprise you – what you’re experiencing is incredibly common. Actually, it’s so common that emergency room doctors have a saying: “The real injuries show up later.”
I know, I know. You’re probably thinking, “But I felt fine right after the accident!” Here’s why that doesn’t mean much… Your body is basically a walking pharmacy when it comes to stress response. The moment that other car kissed your bumper, your system flooded with adrenaline, endorphins, and a cocktail of other chemicals designed to help you handle the crisis. It’s like nature’s own pain medication – except it wears off.
And when it does? That’s when you really feel what happened to your body.
Now, here’s where Irving residents face a particular challenge. You’ve got options – lots of them. Your regular doctor (if you can get an appointment sometime next month), urgent care centers scattered around DFW, the ER at Irving’s medical facilities, or… and this is where it gets interesting… doctors who specifically focus on automobile accident injuries.
But here’s what nobody tells you in those chaotic moments after a fender-bender: not all medical care is created equal when it comes to car accident injuries. Your family doctor is fantastic for your annual checkup and that weird rash you got from your garden. But automobile accident injuries? They’re a different beast entirely.
Think about it like this – you wouldn’t take your car to a bicycle mechanic, even though they both involve wheels and metal parts. The mechanics (sorry, the medicine) are just… different.
So what makes automobile accident injuries so special? Well, they’re sneaky little devils. Whiplash doesn’t show up on standard X-rays. Soft tissue damage loves to play hide-and-seek with typical medical tests. And the symptoms – oh, the symptoms – they can masquerade as everything from stress headaches to “sleeping wrong” neck pain.
Plus, there’s this whole other layer that most people don’t think about until they’re knee-deep in it: the insurance maze. Regular doctors often avoid car accident cases like they’re radioactive. Why? Because dealing with auto insurance companies requires specific documentation, particular terminology, and honestly, more patience than most physicians have time for.
But here’s where automobile accident doctors come in – they speak both languages fluently. Medical and insurance-ese.
Now, I can practically hear what you’re thinking: “This all sounds expensive and complicated. Can’t I just tough it out?” Look, I get it. We’re all busy. Medical appointments are a hassle. And maybe you’re one of those people who’d rather walk off a broken leg than admit something’s wrong.
But here’s the reality check – ignoring car accident injuries is like ignoring a small leak in your roof. Sure, it might not seem like a big deal now, but six months from now when you’re dealing with chronic pain, limited mobility, or worse… well, let’s just say prevention is a whole lot easier than trying to fix something that’s been broken for months.
Throughout this article, we’re going to walk through the signs that you actually need medical attention (spoiler alert: they’re more subtle than you think), what makes automobile accident doctors different from your regular physician, and how to navigate the Irving healthcare landscape when you’re dealing with post-accident symptoms.
We’ll also tackle the insurance questions that keep people up at night, and honestly? Share some real talk about when you’re probably overthinking things versus when you really need to get checked out.
Because here’s the thing – knowledge is power, especially when your body’s trying to tell you something important.
Why Minor Symptoms After Car Accidents Are Trickier Than They Seem
Here’s the thing about car accidents – they’re like that friend who seems totally fine at the party but texts you the next morning saying they feel awful. Your body can be surprisingly good at hiding what’s really going on, especially when adrenaline is coursing through your system like you just chugged three energy drinks.
Think about it this way: when your car gets rear-ended, you might walk around checking for dents and scratches on the bumper. Everything looks fine from the outside, so you figure you dodged a bullet. But what you can’t see is that the frame might be slightly bent, or there’s damage to internal components that won’t show up until later. Your body? Pretty much the same deal.
The Adrenaline Mask – Nature’s Temporary Band-Aid
Right after an accident, your body floods with adrenaline and endorphins – it’s like nature’s own pain management system kicking into high gear. You know that feeling when you stub your toe really hard but don’t feel it until a few seconds later? Same concept, except this natural numbing can last hours or even days after a crash.
I’ve seen people walk away from accidents feeling completely normal, maybe just a little shaken up… then wake up three days later feeling like they got hit by a truck. (Well, technically they did, but you know what I mean.) That stiff neck you’re brushing off? The slight headache you’re attributing to stress? Your back feeling “just a little off”? These seemingly minor symptoms can be your body’s way of waving a tiny flag before it starts waving a much bigger one.
The Domino Effect – How Small Problems Become Big Ones
Your body is basically an intricate chain of moving parts – kind of like those elaborate domino setups you see on YouTube. When one piece gets knocked out of alignment, it doesn’t just affect that one spot. That slight neck strain from whiplash can throw off your posture, which affects your shoulders, which changes how you walk, which eventually has your lower back screaming at you.
What makes this particularly frustrating is that these changes happen gradually. You adapt without realizing it – compensating here, favoring that side there. Before you know it, you’re dealing with pain that seems completely unrelated to that “minor” fender-bender from two weeks ago.
The 72-Hour Window – Why Timing Matters
Here’s where things get a bit counterintuitive. While some symptoms show up immediately, soft tissue injuries – the kind you can’t see on a regular X-ray – often take 24 to 72 hours to really make themselves known. It’s like when you have an intense workout and feel fine that day, but the next morning you can barely move.
During those first few days, inflammation is building up in damaged tissues. Your muscles are tightening as they try to protect injured areas. Microscopic tears in ligaments and tendons are starting to swell. All of this happens below the radar until suddenly… it doesn’t.
Why “Wait and See” Can Backfire
I get it – nobody wants to be that person who rushes to the doctor over every little ache and pain. We’re all trying to tough it out, especially when the symptoms seem manageable. But here’s the tricky part about accident-related injuries: they have this sneaky way of becoming chronic if they’re not addressed early.
Think of it like a small leak in your roof. Sure, you could put a bucket under it and call it good. But that water is still getting into places it shouldn’t be, potentially causing damage you won’t see until it’s much harder and more expensive to fix.
The Insurance Clock Is Always Ticking
And then there’s the practical side – something that’s honestly pretty frustrating about how the whole system works. Insurance companies have their own timelines for when they consider symptoms “related” to an accident. Wait too long, and suddenly that connection becomes much harder to prove, even if your pain is absolutely real and absolutely connected to your crash.
It’s not that they don’t believe you… well, actually, sometimes it is exactly that. But mostly it’s about documentation and establishing clear timelines between cause and effect.
The 24-48 Hour Rule That Could Save You Years of Pain
Here’s something most people don’t know – and honestly, it drives me a bit crazy that nobody talks about it. Your body has this sneaky way of masking serious injuries for the first day or two after an accident. It’s like your nervous system is in shock mode, pumping out natural painkillers and keeping you functional.
So here’s my rule: Wait 24-48 hours, then reassess everything. I’m talking about a proper body scan – not just “do I hurt?” Actually move each joint, stretch your neck in all directions, test your range of motion. That slight stiffness you brushed off yesterday? It might be screaming at you now.
If anything – and I mean *anything* – feels different than it did before the accident, that’s your cue to make that appointment. Don’t wait for it to “get worse.” Prevention beats treatment every single time.
Documentation: Your Future Self Will Thank You
This is where people mess up constantly, and I’ve seen it cause huge problems down the road. You need to document everything – even the stuff that seems silly.
Start a simple voice memo or notes app entry right now. Record the date, time, weather conditions, exactly what happened, and every single symptom you’re experiencing. Did you hit your knee on the dashboard? Write it down. Feel a little dizzy getting out of the car? Document it. Think you’re fine but your shoulder feels “weird”? That goes in the notes too.
Take photos of your vehicle damage from multiple angles. I know it seems unrelated to your health, but the correlation between vehicle damage and potential injury severity is something insurance companies (and doctors) pay close attention to.
Here’s the thing though – don’t just do this once and forget about it. Update your notes daily for at least a week. Symptoms have this annoying habit of playing hide and seek.
Finding the Right Doctor (It’s Not Just About Location)
Not all doctors understand car accident injuries. Harsh truth? Your family doctor might be amazing at treating your allergies but completely miss the subtle signs of a concussion or whiplash-associated disorders.
Look for physicians who specifically mention auto accident or personal injury experience. In Irving, you’ve got options – but do your homework. Check their reviews, but read between the lines. You want someone who takes time during appointments, not someone who rushes you through in 10 minutes.
Ask these specific questions when you call
– Do you have experience with motor vehicle accident injuries? – How soon can I be seen? (Ideally within 72 hours) – Do you work with personal injury attorneys if needed? – What diagnostic tools do you have on-site?
The Insurance Maze – What You Need to Know Right Now
Here’s where things get tricky, and honestly, it’s where most people get taken advantage of. Your auto insurance might cover medical expenses through Personal Injury Protection (PIP) – but you need to understand your coverage limits and requirements.
Call your insurance company today. Not tomorrow, not next week – today. Ask specifically about
– Your PIP coverage limits – Which doctors you can see without pre-authorization – What documentation they require – Time limits for filing claims
Some policies require you to see specific doctors or get pre-approval. Finding this out after you’ve already had treatment can be… well, let’s just say it’s not fun.
Red Flags That Mean “Get Help Now”
Forget waiting 24-48 hours if you experience any of these symptoms – some things need immediate attention
Cognitive issues: Having trouble concentrating, feeling foggy, or finding yourself more forgetful than usual. These can be early concussion signs that people often dismiss as stress.
Sleep disturbances: Either sleeping way more than usual or having trouble staying asleep. Your brain might be trying to heal from trauma you’re not even aware of yet.
Mood changes: Feeling unusually irritable, anxious, or emotional? Post-accident psychological responses are real and treatable – but only if you acknowledge them.
Vision problems: Any changes in your vision, even subtle ones like difficulty focusing or increased light sensitivity.
The bottom line? Trust your instincts. You know your body better than anyone else. If something feels off – even if you can’t quite put your finger on what – that’s valuable information. Don’t let anyone (including yourself) talk you out of getting checked out.
Remember, addressing these issues early isn’t about being dramatic or seeking attention. It’s about taking care of your future self and making sure a minor accident doesn’t turn into a major life disruption.
When Insurance Companies Make You Feel Like a Criminal
Here’s the thing nobody warns you about – insurance adjusters are going to question everything. They’ll ask why you didn’t see a doctor immediately (even though you felt fine), then question why you’re seeing one now. It’s like being caught in some bizarre catch-22 where you can’t win.
The solution? Document everything from day one. Take photos of your vehicle, write down exactly how you’re feeling each day – even if it’s “totally fine” – and keep all correspondence with insurance companies. When you do see that automobile accident doctor, be honest about the timeline. Doctors understand that adrenaline masks pain, but insurance companies… well, they’re not exactly known for their medical expertise.
The “Am I Being Dramatic?” Mind Game
You know that voice in your head? The one that whispers you’re overreacting to a little neck stiffness? Yeah, that one’s not your friend right now. We’ve all been conditioned to “tough it out,” especially when the accident seemed minor. Your car barely has a scratch, you exchanged insurance info like civilized adults, everyone walked away… so why does your shoulder feel weird three days later?
Here’s what I’ve learned from talking to countless patients: your body doesn’t care how dramatic the accident looked. Sometimes the most devastating injuries come from the most unremarkable crashes. That gentle rear-ender while you were stopped at a light? Your neck muscles were completely unprepared for that sudden jolt, and now they’re staging a protest.
The fix isn’t to silence that inner critic – it’s to gather information. Schedule a consultation with an automobile accident doctor in Irving. You’re not committing to months of treatment; you’re getting a professional assessment. Think of it like checking the foundation of your house after an earthquake. Even a small tremor can cause invisible damage that gets worse over time.
The Paperwork Avalanche (And Why It Matters More Than You Think)
Let’s be honest – medical paperwork after an accident is a nightmare. Insurance forms, medical history questionnaires, treatment records… it feels endless. And here’s the kicker: one small mistake or missing piece of information can derail your entire claim.
I’ve seen people lose coverage because they didn’t properly document their symptoms or forgot to mention a previous injury from years ago. The insurance company will dig up that old sports injury from high school and try to blame everything on that.
Your best defense? Create a simple system from day one. Get a dedicated folder (physical or digital) for all accident-related documents. Include a timeline of symptoms, photos of injuries (even if they seem minor), and copies of all medical visits. When you see your automobile accident doctor, bring everything. Don’t assume they’ll connect the dots – spell it out clearly.
The Treatment Guilt Trap
This one’s sneaky. You start feeling better after a few visits to the doctor, and suddenly you feel guilty about continuing treatment. “Maybe I’m fine now,” you think. “Maybe I’m taking advantage of the system.”
Stop right there. Feeling better doesn’t mean you’re healed – it often means the treatment is working. Would you stop taking antibiotics halfway through the prescription because you feel better? Of course not.
Car accident injuries are notorious for seeming better, then flaring up weeks later. Your doctor isn’t trying to milk the system; they’re trying to prevent you from dealing with chronic issues down the road. That shoulder that feels “mostly fine” now could turn into a nightmare if the underlying muscle tension isn’t properly addressed.
Finding the Right Doctor When Everyone’s an Expert
Every friend, family member, and coworker becomes a medical expert after your accident. “My cousin’s neighbor went to this amazing chiropractor…” or “You don’t need a doctor for that – just take some ibuprofen.” The noise can be overwhelming.
Here’s the truth: you need someone who specializes in automobile accident injuries specifically. General practitioners are wonderful, but they might not catch the subtle signs of whiplash or understand how crash dynamics affect your body. Look for doctors who regularly work with car accident patients and understand the insurance process.
Don’t be afraid to ask potential doctors about their experience with automobile accidents during your initial consultation. A good accident doctor won’t be offended – they’ll appreciate that you’re being thorough. After all, this isn’t just about feeling better; it’s about protecting your health and your legal rights for years to come.
What to Expect During Your First Visit
Walking into that first appointment, you’re probably wondering what you’ve gotten yourself into. Will they think you’re overreacting? Are they going to find something terrible… or nothing at all?
Here’s the thing – most accident-related visits start pretty simply. Your doctor will want to hear your story first. Not just the medical stuff, but the whole picture. What happened in those crucial seconds before impact? How did your body move? Sometimes the details you think are irrelevant – like whether you were reaching for your coffee or turned to check your blind spot – actually matter quite a bit.
The physical exam comes next, and it’s usually more thorough than what you’d get for a regular checkup. They’re looking for subtle signs your body might be compensating for an injury. You know how you might favor one leg after stepping on a rock? Your body does similar things after accidents, even minor ones.
Don’t be surprised if they order imaging – X-rays, maybe an MRI if there’s concern about soft tissue. And honestly? Sometimes these come back completely normal. That doesn’t mean you’re imagining things or wasting everyone’s time. Soft tissue injuries, muscle tension, and early inflammation don’t always show up on scans right away.
The Reality of Recovery Timelines
I wish I could tell you that everything gets better in two weeks with some ibuprofen and rest. Sometimes it does – lucky you if that’s your story. But here’s what’s more typical…
Most minor accident-related symptoms follow what we call the “valley pattern.” You might feel okay immediately after (adrenaline is powerful stuff), then worse over the next 24-48 hours as inflammation peaks. Week one is usually the roughest. Then things start improving, but it’s rarely a straight line up.
Realistic timelines for common issues: – Muscle tension and soreness: 1-3 weeks with proper care – Minor whiplash symptoms: 2-6 weeks (yes, that range is frustratingly wide) – Headaches related to neck tension: These can linger longer than you’d expect – sometimes 4-8 weeks – Sleep disruption: Often the last thing to resolve, unfortunately
Some people bounce back in days. Others deal with lingering effects for months. It’s not about being tough or weak – it’s about how your particular body responds to that particular incident.
Your Treatment Plan Moving Forward
Treatment usually starts conservatively, which might feel anticlimactic if you’re expecting dramatic interventions. Physical therapy, targeted exercises, maybe some massage therapy or chiropractic care. Sometimes muscle relaxants or anti-inflammatories for a short period.
The goal isn’t just getting you back to where you were – it’s making sure your body doesn’t develop compensatory patterns that cause problems down the road. You know how favoring that twisted ankle can make your hip hurt three weeks later? Same principle applies here.
Your doctor might recommend follow-up appointments even if you’re feeling better. Don’t skip these. They’re checking to make sure you’re healing properly and not developing those sneaky compensation patterns I mentioned.
When to Be Concerned (And When Not to Panic)
Some ups and downs are completely normal. Having a good day followed by a rough one? Par for the course. Feeling stiff in the morning but better by afternoon? Also typical.
Call your doctor if: – Pain becomes significantly worse instead of gradually improving – You develop new symptoms weeks after the accident – Headaches become more frequent or severe – You’re having trouble sleeping for more than a week – Simple activities become increasingly difficult
Don’t panic about: – Feeling different from day to day – Some stiffness in the morning – Being more tired than usual (your body’s working hard to heal) – Occasional twinges or reminder pains
Documentation Matters (Even for Minor Accidents)
Keep notes about your symptoms, even if they seem trivial. Not for legal reasons necessarily, but because patterns emerge over time that you might forget. “My neck feels tight” on day three becomes more meaningful when you realize it’s been consistent for two weeks.
Take photos of any visible bruising or swelling. Our brains have this funny way of minimizing past pain once we start feeling better.
And yes, keep all your medical records. Even if this feels like much ado about nothing right now, you’ll want that paper trail if symptoms persist or evolve. Trust me on this one – I’ve seen too many people scramble to recreate their medical history months later.
You Don’t Have to Figure This Out Alone
Here’s the thing about car accidents – they’re sneaky. You walk away feeling okay, maybe a little shaken up, and think you’ve dodged a bullet. But your body? It’s got its own timeline for processing what just happened. Those “minor” symptoms you’re brushing off… they’re not always so minor.
I’ve seen too many people who waited – and I get it, I really do. You don’t want to be dramatic. You don’t want to make a big deal out of something that might be nothing. But here’s what I’ve learned over the years: your body is incredibly good at telling you when something’s wrong. That nagging headache? The stiffness that won’t go away? The weird tingling in your fingers? These aren’t just random inconveniences – they’re messages.
And honestly, the peace of mind alone is worth getting checked out. There’s something almost magical about having a professional look you over and either catch something early or give you the all-clear. It’s like… remember when you were a kid and your mom would check for monsters under the bed? Sometimes you just need that expert reassurance that everything’s actually okay.
The medical professionals here in Irving who specialize in auto accident injuries – they’ve literally seen it all. They know exactly what to look for, which tests to run, and how to spot the things that might not show up for days or weeks. Plus, they understand the whole insurance maze, which… let’s be honest, nobody wants to navigate alone.
I think about my friend Sarah a lot when I talk about this. She had what seemed like a tiny fender-bender last year. Felt fine, went about her day, figured she was lucky. Three weeks later, she could barely turn her head. Turns out she had some soft tissue damage that would’ve healed so much faster with early treatment. Now she jokes about being the poster child for “get checked out immediately” – but I know she wishes she’d listened to her body sooner.
Your symptoms might resolve on their own, sure. But they might not. And if they don’t, catching things early can mean the difference between a few weeks of treatment and months of complicated recovery. It’s like that old saying about fixing a small leak before it becomes a flood… except this flood is happening in your body.
The bottom line? You deserve to feel your absolute best. Not “good enough” or “manageable” – but truly, completely well. Those minor symptoms don’t have to be something you just live with or work around.
Take That Next Step
If you’re reading this and thinking “maybe I should get this checked out…” – trust that instinct. Seriously. Your future self will thank you for taking care of this now rather than waiting and wondering.
Why not give us a call today? Our team specializes in post-accident care, and we’re genuinely here to help you feel like yourself again. We’ll listen to what you’re experiencing, do a thorough evaluation, and create a plan that makes sense for your specific situation. No pressure, no judgment – just expert care when you need it most.
You’ve already been through enough stress. Let us help you take care of the rest.