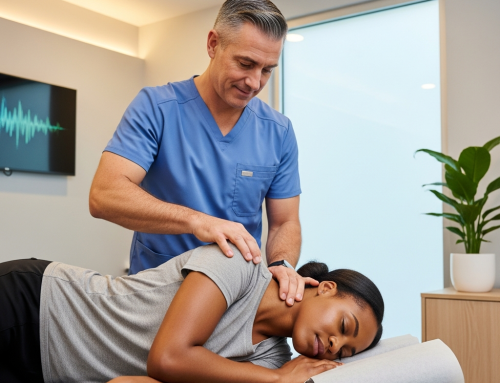
How Long Does Whiplash Treatment Take After a Car Accident?
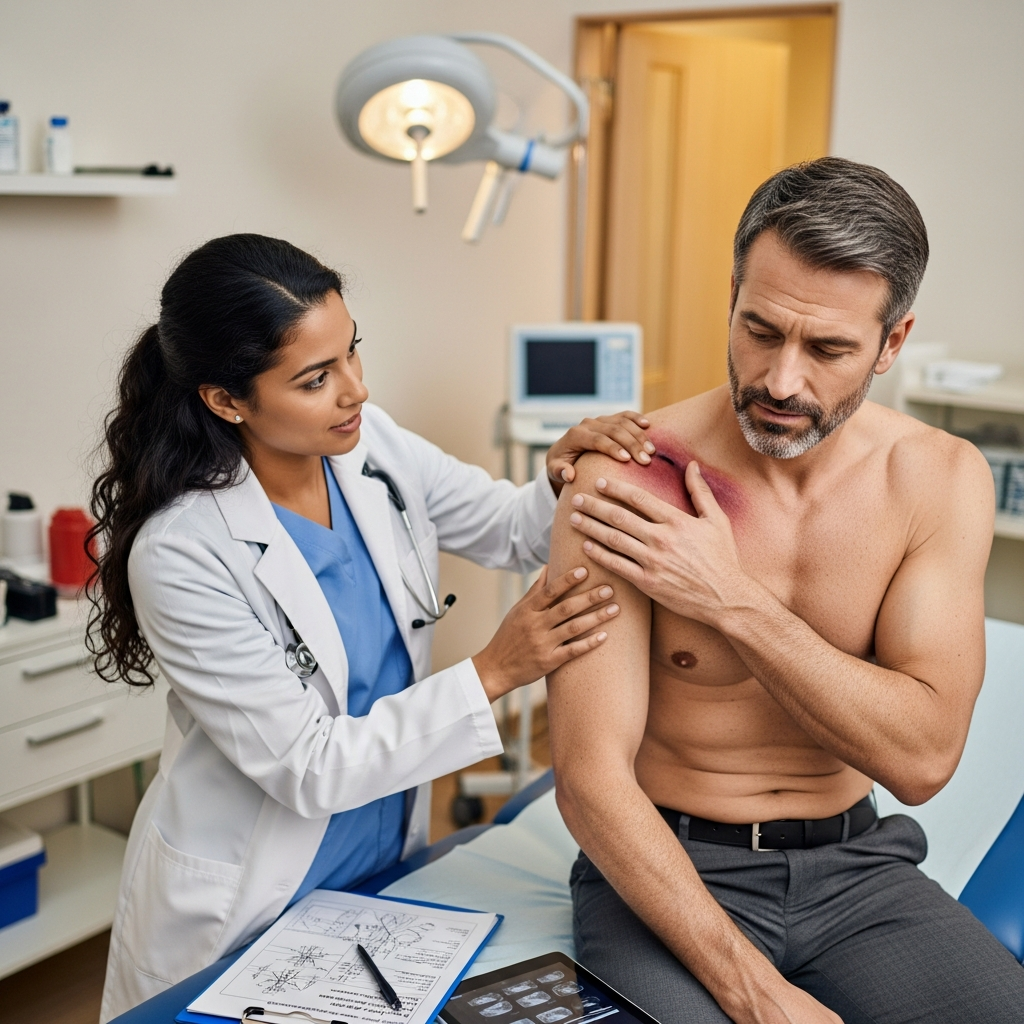
You’re sitting at a red light, scrolling through your phone while waiting for the signal to change. Maybe you’re thinking about dinner plans or that meeting tomorrow. Then – BAM. The world jolts forward, your head snaps back like a rubber band, and suddenly you’re dealing with the aftermath of being rear-ended by someone who was probably doing the exact same thing you were.
Sound familiar? If you’re reading this, chances are you’ve been there. Or maybe you’re there right now, sitting with a sore neck and wondering what the heck comes next.
Here’s the thing about whiplash – it’s sneaky. You might feel fine right after the accident, adrenaline masking what’s really happening in your neck and spine. But then you wake up the next morning feeling like you’ve been hit by a truck… which, well, you kind of were. That’s when the questions start flooding in: How long is this going to hurt? When can I get back to normal? Am I going to need months of treatment?
I get it. The uncertainty is almost worse than the pain itself.
The Reality Check Nobody Talks About
What makes whiplash particularly frustrating is that there’s no neat, tidy timeline. Your coworker might bounce back in two weeks, while your neighbor is still dealing with neck stiffness six months later. It’s not fair, and it definitely doesn’t make sense when you’re trying to plan your life around doctor appointments and wondering if you should cancel that weekend hiking trip.
The truth? Whiplash recovery is about as predictable as your local weather forecast. Sure, there are patterns and general expectations, but every body tells its own story. Your age, overall health, the severity of the accident, even your stress levels – they all play a role in how quickly you’ll heal.
And here’s something that might surprise you: the physical damage isn’t always the biggest factor in recovery time. Sometimes it’s the anxiety about driving again, the financial stress from medical bills, or the frustration of feeling like your body has betrayed you that keeps you stuck in the healing process longer than necessary.
Why This Actually Matters More Than You Think
Look, I’m not going to sugarcoat this – understanding your whiplash timeline isn’t just about managing expectations (though that’s important too). It’s about making smart decisions for your health, your wallet, and your sanity.
When you know what’s normal and what’s not, you can advocate for yourself better. You’ll know when to push through discomfort and when to speak up about concerning symptoms. You’ll understand why your doctor is recommending certain treatments and when it might be time to seek a second opinion.
Plus – and this is huge – you can actually plan your life again. Nothing’s worse than being in limbo, not knowing if you’ll be functional for that work presentation next month or your daughter’s graduation in six weeks.
What We’re Going to Figure Out Together
Throughout this conversation, we’re going to walk through the real timeline of whiplash recovery – not the sanitized medical textbook version, but what it actually looks like when you’re living it day by day. We’ll talk about the different phases you might experience, from those first confusing days when you’re not even sure something’s wrong, to the gradual (and sometimes frustrating) process of getting your strength and range of motion back.
You’ll learn about the factors that can speed up or slow down your recovery… some you can control, others you can’t. We’ll explore different treatment approaches – from the traditional physical therapy route to some newer options you might not have considered. And honestly? We’ll address some of the myths and misconceptions that might be making this whole process more stressful than it needs to be.
Most importantly, you’ll come away with realistic expectations and a clearer sense of what your own recovery might look like. Because while I can’t predict your exact timeline, I can help you understand the journey ahead – and that knowledge? It’s the first step toward taking back control of your healing process.
Ready to figure this out together?
What Actually Happens During Whiplash (It’s Not What Most People Think)
You know that carnival ride where you’re sitting still and suddenly – BAM – the whole thing lurches forward? Your head snaps back against the headrest, then whips forward like you’re nodding “yes” way too enthusiastically. That’s essentially what happens to your neck during a car accident, except instead of screaming with delight, you’re probably screaming for entirely different reasons.
Here’s the thing though – and this might surprise you – the actual “whipping” motion isn’t always the main culprit. Sometimes it’s what happens in those split seconds before impact that really does the damage. Your muscles tense up (thanks, fight-or-flight response), creating this rigid framework around your spine. Then when the collision happens… well, imagine trying to bend a frozen garden hose. Something’s gotta give.
The medical term is “cervical acceleration-deceleration injury,” which sounds way more intimidating than it needs to. But doctors love their fancy names – it basically means your neck got jerked around in ways it definitely wasn’t designed for.
The Players in Your Neck’s Drama
Your cervical spine – that’s the neck portion of your backbone – is honestly pretty remarkable. Seven small vertebrae stacked like irregular Jenga blocks, held together by ligaments (think of them as really strong rubber bands), surrounded by muscles that work overtime to keep your 10-pound head balanced on top.
Between each vertebra, you’ve got these squishy discs that act like shock absorbers. They’re kind of like jelly donuts, actually – tough outer shell, softer center. When whiplash happens, these discs can get compressed, twisted, or even torn. Sometimes the jelly… well, it doesn’t stay put where it should.
The muscles are usually the first responders to injury. They clamp down hard, trying to protect everything else – which is great in theory, but terrible for your comfort level. It’s like having a security system that works too well. Yes, it’s protecting the valuable stuff, but now you can’t move without setting off alarms.
Why Timeline Predictions Are Basically Crystal Ball Reading
Here’s where things get frustrating, and I’m just going to be honest with you – predicting exactly how long your whiplash will take to heal is about as reliable as weather forecasting. We can make educated guesses based on patterns we’ve seen, but your body didn’t read the textbook.
Some people walk away from what looks like a minor fender-bender and feel fine for days… then wake up one morning feeling like they’ve been wrestling with a bear. Others get rear-ended at 35 mph and bounce back in a couple weeks. It’s maddening, really.
The truth is, soft tissue injuries – which is what we’re dealing with here – heal on their own timeline. Unlike a broken bone where we can take an X-ray and say “yep, that’ll be 6-8 weeks,” soft tissues are more mysterious. They don’t show up clearly on standard imaging, and they’re influenced by everything from your stress levels to how well you sleep.
The Sneaky Secondary Effects
What really complicates the healing timeline isn’t always the initial injury – it’s everything that comes after. Your body starts compensating for the pain by changing how you move. You might start holding your head differently, sleeping in weird positions, or tensing your shoulders without realizing it.
It’s like when you hurt your ankle and start limping – pretty soon your hip starts aching because it’s working overtime to compensate. Before you know it, you’ve got this whole cascade of issues that weren’t there originally.
Plus – and this is something doctors are finally starting to talk about more openly – there’s often an emotional component to car accidents that affects physical healing. Your nervous system goes through trauma too, not just your tissues. Sometimes your brain keeps sending “danger!” signals long after the actual threat is gone, keeping those muscles locked up tight.
Actually, that reminds me of something my physical therapist once told me: “The body keeps the score.” It’s not just about the mechanical damage – it’s about teaching your entire system that it’s safe to relax and heal again.
Understanding all this doesn’t make the waiting any less frustrating, but at least it explains why your neighbor’s whiplash story might be completely different from yours.
Getting the Right Team Together (Because You Can’t Do This Alone)
Look, I get it – you’re probably thinking you can tough this out on your own. But here’s the thing about whiplash recovery… it’s like trying to fix a car engine while you’re still driving it. You need the right people in your corner, and you need them fast.
Your primary care doctor is great for the initial diagnosis, but they’re not going to be your MVP here. You want a physical therapist who actually specializes in neck injuries – not just someone who throws a heating pad at you and calls it treatment. Ask specifically: “How many whiplash cases do you see per month?” If they can’t give you a number, keep looking.
And here’s something most people don’t know… chiropractors and physical therapists work differently. PTs focus on strengthening and mobility, while chiropractors work on alignment. You might need both – actually, you probably do. The key is finding ones who talk to each other, not practitioners who think their way is the only way.
The Movement Timeline That Actually Works
Forget what you’ve heard about complete rest. That’s old-school thinking that’ll keep you stuck longer than necessary.
Days 1-3: Yes, take it easy, but don’t become a statue. Gentle neck rotations – think of it like you’re slowly checking if anyone’s watching you. Ice for 15 minutes every few hours, but don’t fall asleep with it on (learned that one the hard way).
Week 1-2: This is where people mess up. They either push too hard or do nothing at all. Start with what I call “turtle movements” – slow, deliberate, within your comfort zone. Your range of motion exercises should feel like a gentle stretch, not a wrestling match with your neck.
Weeks 3-6: Now we’re building. This is when physical therapy really kicks in. You’ll be doing exercises that feel almost too easy – trust the process. Those tiny resistance band movements? They’re rewiring your muscle memory.
Here’s the secret sauce: consistency beats intensity every single time. Fifteen minutes of gentle exercises daily will get you further than one aggressive hour-long session per week.
The Sleep Solution Nobody Talks About
Your pillow situation is probably making everything worse. I know, I know – you love that fluffy cloud you’ve been sleeping on for years. But whiplash changes the game entirely.
You want your neck in neutral alignment – imagine a straight line from your ear to your shoulder when you’re lying on your side. Too many pillows? Your head tilts up. Too few? It drops down. Both spell trouble for healing neck muscles.
Memory foam contour pillows aren’t just marketing hype here – they actually maintain that alignment while you sleep. And if you’re a stomach sleeper… well, this might be the universe telling you it’s time to change. Stomach sleeping forces your neck to twist for hours at a time.
Try this tonight: lie on your back with a small rolled towel under your neck (right at the curve) and a regular pillow under your head. It might feel weird at first, but your neck will thank you in the morning.
Managing the Invisible Symptoms That Drive You Crazy
The headaches, the brain fog, the weird dizzy spells when you turn your head too fast – these aren’t “all in your head,” and they’re not permanent either. But they require their own strategy.
Dehydration makes everything worse with whiplash. Your injured muscles need extra fluids to heal properly, and even mild dehydration can trigger those tension headaches. I’m talking about actual water here – not coffee, not energy drinks, not even that fancy vitamin water.
The brain fog is real, and it’s exhausting. Your brain is working overtime to compensate for mixed signals from your injured neck muscles. Give yourself permission to take mental breaks. Those moments when you feel scattered? That’s your cue to step away from whatever you’re doing.
The Return-to-Normal Reality Check
Here’s what nobody tells you about getting back to your regular activities: it’s not a light switch, it’s a dimmer. You don’t just wake up one day completely healed.
Start with your easiest activities first – maybe it’s checking emails or doing light household tasks. Then gradually work up to things like driving longer distances or returning to your workout routine. Your neck will tell you when you’re pushing too hard… listen to it.
And please, for the love of all things holy, don’t use “feeling better” as permission to skip your exercises. That’s like stopping antibiotics because your infection seems gone – you’re just setting yourself up for problems down the road.
When Your Body Fights the Healing Process
Here’s something nobody warns you about – your neck might feel worse before it feels better, and that’s completely normal. I’ve seen patients panic three weeks into treatment because they’re having a flare-up, thinking they’re somehow broken beyond repair.
Your muscles have been through trauma, and they’re holding tension like a protective shield. When we start loosening things up with physical therapy, sometimes that shield fights back. It’s like when you finally stretch after sitting hunched over your computer for hours – that first stretch can actually hurt a bit.
The solution? Don’t abandon ship during these rough patches. Talk to your treatment team about what you’re experiencing. They can adjust your therapy intensity or add heat/ice protocols to help you through the bumpy parts. And please, don’t compare your week three to someone else’s week three – healing isn’t a competition.
The Insurance Maze (And Why It Makes Everything Harder)
Let’s be real about insurance for a minute. You’re dealing with pain, fatigue, and probably some anxiety about the accident… and then you have to become a part-time insurance detective? It’s exhausting.
I’ve watched patients skip necessary treatments because they’re scared of hitting coverage limits, or they spend hours on hold with adjusters when they should be resting. Some people even rush back to work too early because they’re worried about medical bills piling up.
The thing is, inadequate treatment now often means longer recovery times later – which actually costs more in the long run. It’s like trying to save money by buying cheap tires… you’ll end up spending more when they wear out faster.
Here’s what actually helps: Document everything from day one. Keep a simple log of your symptoms, treatments, and how you’re feeling. Take photos if you have visible bruising or swelling. When you talk to insurance, ask for reference numbers and the names of whoever you speak with. And don’t be afraid to ask your clinic’s billing department for help – they deal with this stuff daily and know the tricks.
The Emotional Rollercoaster Nobody Talks About
You know what’s really hard about whiplash? The mental game. One day you’re feeling optimistic because your range of motion improved, and the next day you can barely turn your head to check your blind spot. It messes with your confidence in ways that go far beyond the physical pain.
A lot of patients develop what I call “car anxiety” – that tense feeling every time they get behind the wheel, or when they see another car approaching an intersection. Your nervous system is still on high alert from the accident, and that actually interferes with healing. Stress hormones keep your muscles tight and your inflammation higher.
Then there’s the isolation factor. When you can’t exercise like you used to, can’t sleep well because of pain, and have to cancel social plans because of fatigue… it takes a toll. Friends who’ve never dealt with chronic pain might not understand why you’re “still dealing with this” months later.
The reality check: This is all normal, and it doesn’t make you weak or dramatic. Consider talking to a counselor who understands accident trauma – many clinics can refer you to someone. Some people find that addressing the emotional side actually speeds up their physical recovery. Go figure.
When Progress Stalls (And You Feel Like Giving Up)
Around the two to three-month mark, a lot of people hit what feels like a plateau. You’ve been doing your exercises religiously, showing up to appointments, and then… nothing. No improvement for weeks. This is where I see people get frustrated and sometimes give up on treatment altogether.
But here’s the thing about healing – it’s not linear. Your body might be doing important repair work that you can’t feel yet. Sometimes we need to switch up the approach entirely. Maybe you’ve gotten as far as you can with traditional PT and need to try dry needling, or massage therapy, or even look at whether stress is keeping your muscles locked up.
What works: Schedule a frank conversation with your treatment team about adjusting your plan. Sometimes we need to take a step back and try a completely different approach. And please, be honest about what you’re doing (or not doing) at home. If those exercises are too painful or time-consuming, say so – we can modify them.
Recovery isn’t just about time passing – it’s about finding the right combination of treatments that work for your specific injury and your life circumstances. Sometimes that takes some trial and error, and that’s okay.
What’s Actually Normal (And What Isn’t)
Here’s the thing about whiplash recovery – it’s not like a broken bone where you get a nice, neat six-week timeline. Your neck is complicated, with layers of muscles, ligaments, and nerves all doing their own thing. Some people feel better in a few weeks, others take months. Both can be completely normal.
Most folks with mild whiplash start feeling human again within 2-6 weeks. You know – when turning your head to check your blind spot doesn’t make you wince anymore. But here’s where it gets tricky… some symptoms like to hang around longer than others. That nagging headache? The stiffness that shows up on rainy days? Sometimes they’re the last to leave the party.
If you’re still dealing with significant pain after 3-6 months, don’t panic – but do pay attention. This is when your doctor might start using terms like “chronic whiplash” or “whiplash-associated disorders.” Sounds scary, but really it just means your body needs a different approach to healing.
Red Flags That Need Immediate Attention
Look, I don’t want to scare you, but there are some symptoms that mean “drop everything and call your doctor right now.” We’re talking about
– Severe headaches that keep getting worse (not the usual post-accident headache, but the kind that makes you nauseous) – Numbness or tingling in your arms or hands that doesn’t go away – Weakness in your arms – like you suddenly can’t grip things properly – Dizziness that makes you feel like you’re on a boat – Memory problems or confusion that seems to be getting worse
These could signal something more serious than typical whiplash – maybe nerve damage or a concussion that got missed initially. Better safe than sorry, right?
Your Recovery Roadmap
The first few days? Ice, rest, and gentle movement when you can tolerate it. Those old-school rigid neck braces? Most doctors skip them now unless there’s something more serious going on. Movement – even tiny amounts – usually helps more than staying completely still.
Week 1-2 is often when you’ll start physical therapy if your doctor recommends it. Don’t be surprised if you feel worse before you feel better – that’s actually pretty normal. Your therapist is basically teaching your muscles how to work together again after they’ve been in protective mode.
By week 3-4, you should notice some improvement. Maybe you can look over your shoulder without that sharp catch, or you wake up with less stiffness. If you’re not seeing any progress by this point, definitely check back with your doctor.
The 6-12 week mark is where things can get frustrating. You might feel about 80% better, but that last 20% seems to drag on forever. This is when some people give up on their exercises or skip physical therapy appointments. Don’t be that person – this phase is crucial for preventing long-term problems.
When to Consider Additional Help
Sometimes standard treatment isn’t enough, and that’s okay. If you’re 8-12 weeks in and still struggling, your doctor might suggest things like massage therapy, chiropractic care, or even psychological support. That last one isn’t because the pain is “in your head” – chronic pain genuinely affects your mental health, and addressing that often helps the physical healing too.
Some people benefit from injections – trigger point injections or nerve blocks – especially if specific muscles or nerves are being particularly stubborn. Others find relief through alternative approaches like acupuncture. The key is finding what works for your specific situation.
Managing Expectations (The Real Talk)
Here’s what I wish more people understood: recovery isn’t always linear. You might have a great week followed by a rough few days. Weather changes, stress, poor sleep, or even something as simple as sleeping wrong can cause temporary flare-ups.
Most people do get back to their normal activities within 2-3 months. But “normal” might look slightly different than before – maybe you’re more aware of your posture now, or you’ve learned some neck stretches that help when things get tight.
The goal isn’t necessarily to pretend the accident never happened. It’s to get you back to living your life without pain calling the shots. And honestly? Most people get there, even if the path isn’t exactly what they expected.
Look, I know this feels overwhelming right now. You’re sitting there with a sore neck, maybe some headaches, wondering when you’ll feel normal again… and that’s completely understandable. The truth is, healing doesn’t follow a neat timeline – your body has its own rhythm, and that’s okay.
What I’ve seen work best for people is taking it one day at a time while staying actively engaged in your recovery. Some days you’ll feel great, others might have you reaching for the ice pack again. That’s not failure – that’s just how healing works. Your body is doing incredible repair work behind the scenes, even when progress feels frustratingly slow.
Remember, those two to twelve weeks we talked about? They’re not set in stone. I’ve worked with people who bounced back in three weeks (lucky them!) and others who needed six months to really feel themselves again. Neither path is wrong. Your injury is as individual as your fingerprint, influenced by everything from how the accident happened to how well you sleep at night.
The key is not to suffer in silence or try to tough it out alone. That whole “walk it off” mentality? It doesn’t serve you here. Getting the right support early – whether that’s physical therapy, massage, or even just having someone who understands what you’re going through – can make such a difference in how you heal.
And please don’t let insurance timelines pressure you into thinking you should be “fixed” by some arbitrary date. I’ve seen too many people rush back to normal activities before they’re ready, only to find themselves dealing with lingering issues months later. Your timeline is your timeline.
Here’s something else worth mentioning… the mental side of this matters too. Car accidents shake us up in ways we don’t always expect. Feeling anxious about driving, being hyperaware of every little twinge – that’s all normal. Healing includes your peace of mind, not just your physical symptoms.
If you’re reading this and nodding along, thinking “yes, that’s exactly how I feel,” you don’t have to figure this out alone. Whether you’re just starting to deal with whiplash symptoms or you’ve been struggling for weeks, there’s help available. Good help. The kind that actually listens to what you’re experiencing instead of rushing you through some cookie-cutter treatment plan.
You know what? Give us a call. Not because I’m trying to sell you something, but because you deserve to have someone in your corner who understands exactly what you’re dealing with. We’ve helped hundreds of people work through whiplash recovery, and we’d be honored to help you too.
Your recovery matters. You matter. And while I can’t promise it’ll be quick or easy, I can promise you won’t have to face it alone. Sometimes that makes all the difference in the world.
Take care of yourself – you’re doing better than you think you are.