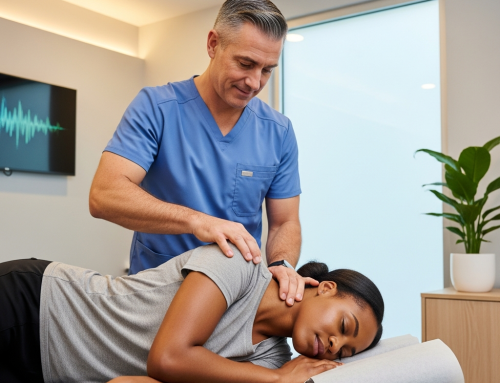
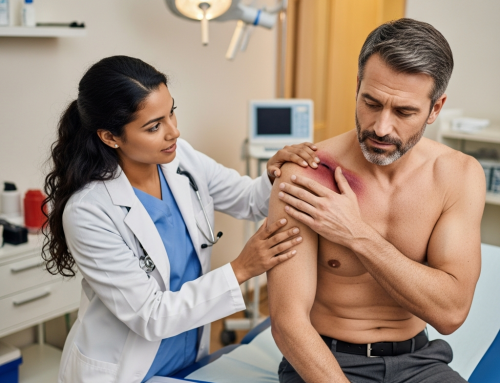
How Personal Injury Physicians Treat Auto Injury and Car Accident Trauma
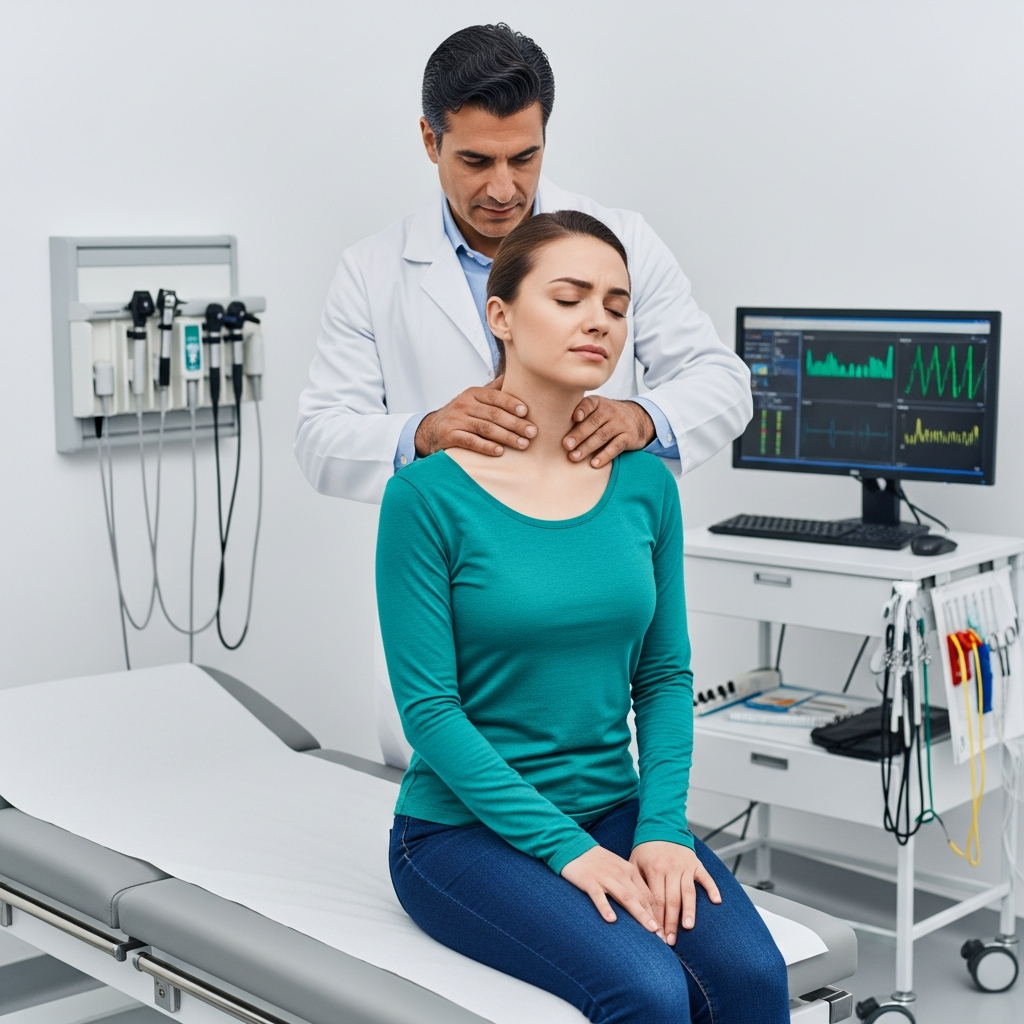
You’re driving through your neighborhood – the same route you’ve taken a thousand times. Maybe you’re thinking about what to make for dinner, or mentally reviewing tomorrow’s meeting. Then it happens. That split second when time seems to freeze, when you see the other car running the red light, when you realize there’s nothing you can do to avoid it.
The impact jolts you back to reality. Your heart pounds. Your hands shake. And in those first confusing moments, you’re asking yourself the same question millions of people face every year: “Am I hurt?”
Here’s the thing about car accidents – they’re sneaky. Sure, if you’ve got a broken bone jutting out at an odd angle, that’s pretty obvious. But most auto injuries? They hide. They whisper instead of scream. Your adrenaline is pumping so hard that you might not feel that pulled muscle in your neck, that compressed disc in your back, or the way your shoulder now sits just a little differently than it did this morning.
You exchange insurance information, maybe get checked out at the ER (where they thankfully tell you nothing’s broken), and you think you’ve dodged a bullet. But then… three days later, you wake up and can barely turn your head. Or maybe it’s two weeks later when that “minor” back twinge becomes a constant, nagging ache that’s making it hard to sleep.
Sound familiar? You’re definitely not alone in this.
The uncomfortable truth is that emergency rooms are fantastic at ruling out life-threatening injuries – and that’s exactly what they’re designed to do. But they’re not equipped to catch the subtle soft tissue damage, the microscopic tears in ligaments, or the inflammation that’s just getting started. Think of it this way: the ER is like a smoke detector – it’ll tell you if there’s a fire, but it won’t notice if your foundation is slowly settling.
That’s where personal injury physicians come in, and honestly, most people have no idea they exist until they really need them.
These doctors – they’re like medical detectives who specialize in the aftermath of trauma. They understand that a 25-mph fender bender can absolutely wreck your neck (physics is weird that way), and they know how to spot injuries that might not show up on standard X-rays. More importantly, they get that your pain is real, even when everyone around you keeps saying, “But the cars barely have a scratch!”
I’ve been writing about health and wellness for years, and I keep coming back to this topic because I see the same pattern over and over again. Someone gets hurt in an accident, tries to “tough it out” for weeks or months, and then finally seeks help when the pain becomes unbearable. By then, what could have been a straightforward recovery has turned into a chronic condition that affects their work, their relationships, their sleep… basically, their entire life.
Here’s what we’re going to explore together: how personal injury physicians actually approach auto accident trauma differently than your regular doctor (spoiler alert: it’s all about understanding the mechanics of what happens to your body during impact). We’ll talk about the detective work they do to uncover hidden injuries, the treatment approaches that actually work for accident-related trauma, and – this is important – how working with the right physician can make or break your insurance claim.
You’ll learn about the timeline of injury recovery (because yes, there’s a method to the madness), what red flags to watch for that mean you need specialized care, and how to advocate for yourself when insurance companies start asking uncomfortable questions about your treatment.
Look, nobody plans to need a personal injury physician. But if you’re reading this because you’re dealing with lingering pain from an accident, or you’re worried about someone you care about, or you just want to be prepared (smart thinking, by the way), then you’re in the right place.
Because here’s the thing – your body deserves better than “just wait and see if it gets better.” Sometimes, it needs an expert who really understands what it’s been through.
Your Body’s Hidden Alarm System
When you’re in a car accident – even what seems like a minor fender-bender – your body basically hits the panic button before your brain even processes what happened. It’s like having a smoke detector that goes off when you burn toast… except this alarm system affects every muscle, joint, and nerve in your body.
The thing is, adrenaline is sneaky. You might walk away from an accident feeling totally fine, maybe even a little proud of how well you handled everything. But adrenaline is basically nature’s pain medication, masking injuries that won’t announce themselves until hours or even days later. I’ve seen patients who felt great at the scene, exchanged insurance information like champs, and then woke up the next morning feeling like they’d been hit by a truck. Which, well… they kind of were.
The Whiplash Web (It’s More Complicated Than You Think)
Here’s where things get interesting – and honestly, a bit frustrating for patients. When people hear “whiplash,” they usually picture their head snapping back and forth like a bobblehead doll. That’s part of it, but whiplash is actually more like a domino effect that can ripple through your entire body.
Your spine isn’t just one solid piece – it’s made up of 33 individual vertebrae stacked like Jenga blocks, held together by ligaments, tendons, and muscles. During an accident, these structures get stretched, compressed, and twisted in ways they’re definitely not designed for. Even a 5 mph collision can generate forces that exceed what your neck muscles can handle.
And here’s the kicker: the pain doesn’t always show up where the actual damage occurred. You might have neck trauma but feel it in your shoulders, back, or even get headaches. It’s like having a kink in a garden hose – the blockage might be in one spot, but it affects water flow throughout the entire system.
The Invisible Injury Problem
This is probably the most frustrating part for accident victims (and honestly, sometimes for doctors too). Unlike a broken bone that shows up clearly on an X-ray, soft tissue injuries – damage to muscles, ligaments, and tendons – often don’t appear on standard imaging right away.
Think about it like this: if you sprain your ankle, it swells up immediately and you can see the damage. But when the same type of injury happens to tissues in your neck or back during an accident, the swelling and inflammation might be happening deep inside where you can’t see it. The pain is real, the injury is real, but proving it becomes this whole complicated thing.
That’s why personal injury physicians have developed specialized approaches that go way beyond just looking at X-rays and saying “you’re fine.”
Why Your Regular Doctor Might Miss Things
I don’t want to throw anyone under the bus here, but there’s a real difference between how emergency room doctors and personal injury specialists approach car accident trauma. ER docs are amazing at what they do – they’re looking for life-threatening injuries that need immediate attention. Broken bones, internal bleeding, head trauma… the big, scary stuff.
But they’re not really equipped to evaluate the subtle, complex injuries that might not show symptoms for days or weeks. It’s like asking a heart surgeon to fix your watch – they’re both highly skilled, but they have different specialties and different tools.
The Inflammation Factor Nobody Talks About
Here’s something that surprised me when I first learned about auto injury treatment: inflammation plays this huge role that extends way beyond the obvious stuff. When your body experiences trauma, it floods the injured areas with inflammatory chemicals. This is actually a good thing initially – it’s your body’s way of protecting damaged tissue and starting the healing process.
But sometimes this inflammatory response gets stuck in “on” mode, creating chronic pain and stiffness that can last for months or even years if not properly treated. It’s like having a car alarm that won’t shut off… eventually, you need someone who knows how to properly reset the system, not just temporarily muffle the sound.
The good news? Personal injury physicians understand this cascade effect and have specific tools and techniques designed to interrupt this cycle before it becomes a long-term problem.
What to Expect During Your First Visit
Let me tell you what really happens when you walk into a personal injury physician’s office – because honestly, most people have no clue what they’re getting into.
First off, plan for at least 90 minutes. I know, I know… you’re thinking “seriously?” But here’s the thing – these doctors actually *listen*. They’re not rushing you out the door after five minutes like your regular GP might. They’ll ask about everything: how you were sitting in the car, which direction you were facing, whether you saw the impact coming (that fight-or-flight response makes a huge difference), and even what you ate that morning. It might seem excessive, but trust me – those details matter more than you’d think.
Bring your accident report, insurance cards, and – this is crucial – write down your symptoms beforehand. I’m talking everything. That weird tingling in your pinky finger? Write it down. The headache that only hits around 3 PM? Document it. Your brain’s still processing trauma, and you’ll forget half of what’s bothering you once you’re sitting in that exam room.
The Hidden Symptoms They’re Really Looking For
Here’s where it gets interesting. While you’re focused on your obvious injuries – the whiplash, the back pain – these physicians are detective-hunting for the sneaky stuff that shows up later.
They’re checking your eyes for signs of mild traumatic brain injury. Those tracking tests where you follow their finger? They’re not just going through the motions. Concussions from car accidents often get missed because, well, you didn’t hit your head on anything obvious. But your brain? It bounced around inside your skull like a pinball.
They’re also watching how you walk, how you turn your head, whether you favor one side without realizing it. I’ve seen patients who swore they felt “fine” discover they’d been unconsciously compensating for injuries they didn’t even know they had.
Treatment Plans That Actually Work (Not Just Band-Aids)
Forget what you think you know about auto injury treatment. These aren’t “take two aspirin and call me” doctors.
Most personal injury physicians use what I call the layered approach. Week one might be all about inflammation control – ice, specific positioning techniques, maybe some gentle manipulation. But here’s the secret sauce: they’re not just treating your spine. They’re looking at how your injury affects your sleep, your digestion, even your mood.
Physical therapy usually starts around week two, but not the generic kind. We’re talking targeted exercises that retrain your muscles to support your healing spine properly. And chiropractic care – when it’s done right – focuses on restoring normal movement patterns, not just cracking your back until you feel better temporarily.
The really good clinics also incorporate things like massage therapy (the therapeutic kind, not the spa kind), acupuncture for nerve pain, and sometimes even cognitive therapy to help process the trauma. Because let’s be real – car accidents mess with your head as much as your body.
Working with Insurance (Without Losing Your Mind)
Okay, this part’s a bit of a chess game, but here’s how to play it smart.
Document everything. I mean *everything*. Take photos of your car damage from multiple angles. Keep a daily symptom journal – even when you’re feeling better, note that too. Insurance companies love to argue that you’re not really injured, and your detailed records become your best defense.
Most personal injury physicians handle insurance paperwork directly, which is honestly a lifesaver. But stay in the loop. Ask for copies of all reports they send to your insurance company. Sometimes there are discrepancies, and catching them early saves massive headaches later.
Here’s an insider tip: if your insurance company requests an “independent medical exam” (IME), don’t panic, but do prepare. These doctors work for the insurance company, not you. Stick to the facts, don’t downplay your symptoms, but don’t exaggerate either. Consistency is key.
When to Consider Legal Help
Look, I’m not saying you need a lawyer for every fender-bender. But if your medical bills are climbing, you’re missing work, or the other driver’s insurance company is giving you the runaround… well, that conversation might be worth having.
The thing is, once you settle with insurance, you can’t go back for more money if complications arise later. And with auto injuries – especially soft tissue damage – complications can show up months down the road.
When Your Body Doesn’t Bounce Back Like You Expected
You thought you’d be fine by now. Maybe it’s been three weeks since the accident, or three months – and you’re still waking up with that same nagging neck pain. Your friends keep asking when you’ll be “back to normal,” and honestly? You’re starting to wonder the same thing.
This is probably the biggest shock for most people after a car accident. We see crashes in movies where people walk away, dust themselves off, and carry on. Real life doesn’t work that way. Your body might take months to fully heal, not days or weeks. And that’s completely normal, even if it feels anything but.
The solution isn’t to push through the pain or pretend it’s not there. It’s to adjust your expectations and work with your physician to create a realistic timeline. Some injuries – especially soft tissue damage – take time to show their full extent, and even longer to heal properly.
The Insurance Company Runaround That Nobody Warns You About
Let’s talk about something that catches almost everyone off guard: dealing with insurance while you’re trying to heal. You’re already exhausted from pain and medical appointments, and then you have to become a part-time claims adjuster, tracking down paperwork and justifying why you need that third physical therapy session.
Insurance companies… well, they’re not exactly incentivized to make this easy for you. They might question your treatment plan, delay approvals, or make you feel like you’re somehow exaggerating your symptoms. It’s frustrating, and it can actually slow down your recovery when you’re stressed about coverage.
Here’s what actually helps: Ask your physician’s office about their experience with auto injury claims. Most personal injury docs have staff who know exactly which forms to fill out and how to present your case to insurance. Don’t try to navigate this alone – you’ve got enough on your plate.
When Pain Shows Up Fashionably Late
Maybe you felt okay right after the accident. Adrenaline’s a powerful thing. But now, days or even weeks later, you’re dealing with symptoms that seem to come out of nowhere. Your shoulder aches when you reach for something. Your lower back seizes up when you get out of bed. What gives?
This delayed onset thing trips up so many people because it doesn’t match what we expect from an injury. If you cut your finger, it hurts immediately. But car accidents create forces that can cause micro-tears in muscles and ligaments – damage that takes time to develop into full-blown symptoms.
The key is not to dismiss new pain just because it didn’t show up right away. Keep a simple log of what hurts and when. Your physician needs this information to understand how your injuries are evolving. And please – don’t let anyone (including yourself) minimize these symptoms just because they appeared later.
The Treatment That Feels Like It’s Going Nowhere
Physical therapy can feel like… well, like you’re paying someone to make you do exercises that hurt. Especially in those first few sessions when you’re sore and everything feels harder than it should be. You might wonder if it’s actually helping or if you’re just wasting time and money.
This is where patience becomes your best friend (easier said than done, I know). Progress in physical therapy often happens in tiny increments that are hard to notice day-to-day. Think of it like watching grass grow – you can’t see it happening, but suddenly one day you realize your lawn looks different.
Ask your therapist to help you track measurable improvements. Maybe it’s how far you can turn your head without pain, or how many minutes you can sit comfortably. These concrete markers help you see progress when it feels like you’re stuck.
The Mental Game Nobody Prepared You For
Here’s something that catches people completely off guard: the emotional aftermath of a car accident can be just as challenging as the physical injuries. You might find yourself anxious about driving, or jumping at unexpected sounds. Some people develop what feels like hypervigilance – constantly scanning for potential dangers.
This isn’t weakness or being dramatic. It’s your brain trying to protect you after a traumatic event. But it can interfere with healing when you’re constantly in fight-or-flight mode.
Talk to your physician about this – many personal injury docs work with counselors who specialize in accident trauma. Sometimes a few sessions can make a huge difference in your overall recovery. Your mental health and physical healing aren’t separate processes; they’re deeply connected.
What to Expect During Your Recovery
Let’s be honest – you’re probably wondering how long this is going to take. And that’s completely normal. After a car accident, everyone wants the same thing: to feel like themselves again, and preferably yesterday.
The truth is, healing from auto injuries isn’t like following a recipe where you can set a timer and know exactly when you’ll be done. Your body has its own timeline, and it’s rarely the same as your mind’s timeline (which, let’s face it, wanted you better last week).
Most soft tissue injuries – things like whiplash, muscle strains, and minor joint sprains – start showing improvement within the first few weeks of treatment. You might notice less morning stiffness, or realize you turned your head without wincing. These small victories? They matter more than you think.
For more complex injuries involving multiple areas or nerve involvement, we’re typically looking at several months of treatment. I know that sounds daunting when you’re in pain right now, but here’s what I’ve learned after years of working with accident patients: the people who do best are those who focus on the week-to-week progress rather than watching the calendar.
Some days will be better than others – and that’s not a sign that treatment isn’t working. Your body is literally rebuilding damaged tissues, and that process has natural ups and downs. Think of it like renovating a house while you’re still living in it… there’s going to be some chaos before everything comes together.
Working With Your Treatment Team
Your personal injury physician isn’t working in isolation – you’re likely going to have a small team of people helping you get back to normal. This might include physical therapists, massage therapists, maybe a chiropractor or pain management specialist.
It can feel overwhelming at first, keeping track of all these appointments. (Pro tip: put everything in your phone calendar with reminders. Your brain has enough to deal with right now without trying to remember if PT is Tuesday or Thursday.)
Don’t be shy about asking questions. If something doesn’t make sense, speak up. If a treatment isn’t helping after several sessions, mention it. Your feedback helps your doctor adjust your care plan – think of yourself as a partner in this process, not just a passenger.
The Insurance Maze (Unfortunately, We Have to Talk About This)
Here’s something nobody warns you about: dealing with insurance after an auto accident can sometimes feel more exhausting than the actual injuries. Your personal injury physician’s office will typically handle most of the insurance communication, but you’ll still need to stay informed.
Keep a simple folder – physical or digital – with all your accident-related documents. Medical bills, insurance correspondence, police reports… it sounds tedious, but you’ll thank yourself later when you’re not frantically searching for that one form your lawyer needs.
Most personal injury practices are experienced with auto insurance claims, so they know which treatments are typically covered and how to document everything properly. Still, don’t assume anything – ask about coverage before starting new treatments if you’re concerned about costs.
Signs You’re Improving (Even When It Doesn’t Feel Like It)
Recovery isn’t always dramatic. You won’t wake up one morning completely pain-free with angels singing. Instead, you might notice you slept through the night without waking up sore. Or that you reached for something on a high shelf without thinking about it first.
Pay attention to these subtle improvements: less reliance on pain medication, better sleep, improved mood, increased activity tolerance. Your doctor will track objective measures too – range of motion, strength tests, functional assessments – but your day-to-day experience is equally important.
When to Be Concerned
Most people heal predictably, but sometimes you need to speak up. If your pain suddenly worsens significantly, if you develop new symptoms that weren’t there before, or if you’re not seeing any improvement after several weeks of consistent treatment – these are conversations to have with your doctor.
You know your body better than anyone else. Trust that instinct when something doesn’t feel right.
Moving Forward
Recovery from auto injuries requires patience – with your body, with the process, and honestly, with the whole situation. But here’s what I can promise: most people do get better. They return to work, to their hobbies, to feeling confident in their bodies again.
Your healing might not look exactly like someone else’s, and that’s okay. Focus on your progress, communicate openly with your treatment team, and remember that taking care of yourself after an accident isn’t selfish – it’s necessary.
Your Recovery Matters More Than You Think
Look, I get it. After a car accident, you’re dealing with insurance calls, vehicle repairs, maybe even legal stuff – and the last thing you want is another appointment on your calendar. But here’s what I’ve learned from working with countless patients who’ve been exactly where you are right now: ignoring those aches and pains, hoping they’ll just… disappear? That’s like putting a band-aid on a broken pipe.
Your body is incredibly smart – it’s been keeping you alive this whole time, after all – but trauma from car accidents creates this perfect storm of inflammation, muscle tension, and structural misalignment that honestly needs professional attention. Not because you’re weak or dramatic (trust me, I’ve heard every self-doubt story), but because that’s literally how healing works.
The physicians who specialize in auto injuries? They’ve seen it all. That weird pain that shoots from your shoulder to your fingers… the headaches that seem to come out of nowhere… the way your back locks up when you try to get out of bed in the morning. None of this surprises them. Actually, they’re probably nodding along thinking, “Yep, classic whiplash pattern” or “Textbook soft tissue damage.”
What really gets me is how many people suffer in silence, thinking they should just “tough it out.” Listen – you wouldn’t try to fix a complex car problem with duct tape and hope, would you? Your body deserves that same level of care and expertise.
These specialized doctors don’t just throw medications at symptoms and send you on your way. They’re looking at the whole picture: how the accident affected your spine, your muscles, your nervous system… even how it’s impacting your sleep and stress levels. Because – and this might sound obvious but it bears repeating – everything in your body is connected.
The treatment approaches we’ve talked about aren’t just temporary fixes either. Sure, you might feel some relief right away (and honestly, that’s pretty amazing when you’ve been hurting), but the real magic happens over time. Your body starts remembering how it’s supposed to move. Those compensatory patterns you developed – you know, favoring one side or hunching your shoulders – gradually fade away.
And here’s something that might surprise you: most people actually feel better than they did *before* their accident once they complete treatment. Not just back to baseline, but genuinely stronger and more resilient. There’s something about addressing those underlying issues – the ones that were probably brewing long before that fender-bender – that creates this ripple effect of wellness.
If you’re sitting there reading this, still on the fence about getting help… maybe your accident was weeks ago, maybe it was yesterday… either way, your pain is real, and you deserve to feel good in your own body again.
We’re here when you’re ready. No judgment, no pressure – just experienced professionals who understand exactly what you’re going through and know how to help you get back to feeling like yourself. Because that person you were before the accident? They’re still there, just waiting to feel comfortable and confident again.