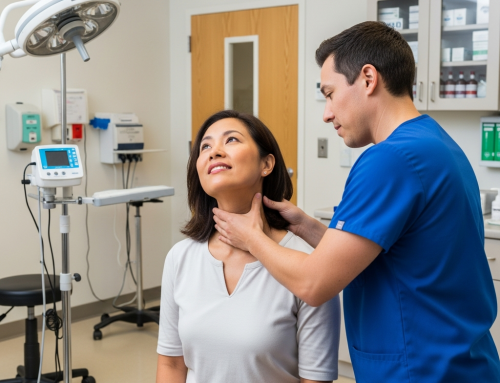
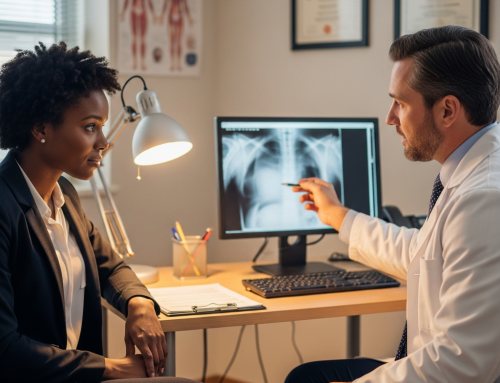
What Happens During Your First Visit After an Auto Accident in Irving?

You’re sitting in your car at the intersection of MacArthur and Irving Boulevard, waiting for the light to change. Your mind’s probably on dinner plans or that work presentation tomorrow – you know, the usual Thursday evening mental shuffle. Then BAM. The world tilts sideways as someone plows into your rear bumper.
In that split second, everything changes. Your neck snaps forward, then back. Your heart’s hammering against your ribs. And honestly? You’re not even sure what just happened.
Sound familiar? If you’ve been in an auto accident here in Irving – or anywhere, really – you know that jarring moment when normal life just… stops. The immediate aftermath is a blur of insurance calls, police reports, and that nagging question: “Am I actually hurt, or am I just shaken up?”
Here’s the thing that catches most people off guard: your body doesn’t always send you the memo right away. You might walk away from the scene feeling okay – maybe a little rattled, but okay. You exchange information, file the report, and figure you dodged a bullet. But then the next morning hits, and suddenly your neck feels like someone’s been using it as a punching bag all night.
Or maybe it’s three days later when that headache that “isn’t that bad” becomes the kind of pain that makes you wince every time you turn your head. Maybe it’s the way your lower back starts talking to you in a language you’ve never heard before – and trust me, it’s not saying anything pleasant.
That’s when most people start wondering: should I see someone about this? And if so… what exactly happens when I walk into a medical office after a car accident? Because let’s be honest – if you’ve never been through this before, the whole process can feel pretty intimidating.
You’re dealing with insurance companies who speak in a foreign language of policy numbers and coverage limits. There might be attorneys involved (which feels way more serious than you bargained for). And somewhere in the middle of all this chaos, you need to figure out if your body actually needs help healing from something you can’t quite put your finger on.
The uncertainty is probably the worst part. You don’t know if that stiffness in your shoulders is going to stick around for weeks… or months. You’re not sure if you should be worried about that weird tingling in your arm, or if it’s just stress manifesting in creative ways. And honestly? You might be wondering if people will think you’re making a big deal out of nothing.
I get it. I’ve been working with auto accident patients here in Irving for years, and I’ve heard these concerns countless times. The truth is, your body is incredibly good at protecting you in the moment of impact – all those muscles tense up, your nervous system goes into overdrive, everything locks down to minimize damage. But that protective response? It doesn’t just magically switch off once the danger’s passed.
Your first medical visit after an accident isn’t just about checking a box for your insurance company (though that’s important too). It’s about understanding what actually happened to your body during those few seconds of chaos – and more importantly, what needs to happen next so you can get back to feeling like yourself again.
We’re going to walk through exactly what you can expect during that first appointment. Not the sterile, clinical version you’d find in a medical textbook, but the real deal – what it actually feels like to sit in that waiting room, what questions you’ll be asked (and why), and what those tests and examinations are really looking for.
Because here’s what I’ve learned: knowledge kills anxiety. When you know what’s coming, when you understand the process, when you can anticipate what’s next – that’s when you stop feeling like a victim of circumstances and start feeling like someone who’s taking control of their recovery.
And that shift? It makes all the difference in how quickly – and how completely – you heal.
Your Body’s Silent Response to Trauma
Here’s something that might surprise you – your body after a car accident is like a smartphone that’s been dropped. Everything looks fine on the outside, the screen isn’t cracked, but there might be some serious internal damage that won’t show up until you try to use certain apps… or in your case, certain movements.
When you’re in an accident, even a seemingly minor one, your body goes into this incredible protective mode. We’re talking milliseconds here – faster than you can even process what’s happening. Your muscles tense up like they’re bracing for impact (because, well, they are), your nervous system floods with adrenaline, and your spine gets subjected to forces it was never designed to handle.
The tricky part? You might walk away feeling absolutely fine. That adrenaline is nature’s painkiller, and it’s surprisingly effective at masking what’s really going on underneath.
The 24-48 Hour Reality Check
This is where things get… interesting. And by interesting, I mean potentially uncomfortable.
Most people don’t realize that the real symptoms often don’t kick in until the next day, sometimes even longer. It’s like your body is on a delayed reaction timer. You go to bed thinking you dodged a bullet, then wake up feeling like you’ve been hit by… well, another car.
Your neck might be stiff as a board. Your lower back could be screaming. Maybe you’ve got this weird headache that won’t quit, or your shoulder feels like it’s full of gravel. This isn’t your imagination – this is your body finally processing what just happened to it.
Think of it this way: if you sprint a mile without warming up, you don’t feel the real impact until the next morning when you can barely walk down stairs. Car accidents are similar, except instead of choosing to sprint, physics chose for you.
Why Irving’s Medical Landscape Matters
Now, here’s something specific to our area that’s worth understanding. Irving sits right in this unique spot where we’ve got everything from major trauma centers to specialized clinics, but – and this is important – not every medical facility is created equal when it comes to auto accident injuries.
Some places are fantastic for everyday health issues but might not have the specific experience with the biomechanics of car crashes. Others specialize in exactly this type of trauma but might have long wait times or require referrals. It’s like having a toolbox full of hammers when you need a screwdriver… the tools are good, they’re just not the right fit for your particular problem.
The Insurance Maze (Yes, It’s Actually a Maze)
Let’s be honest about something that confuses pretty much everyone: dealing with insurance after an accident is about as straightforward as assembling IKEA furniture blindfolded.
You’ve got your insurance, their insurance, maybe PIP coverage (Personal Injury Protection – basically insurance that pays for medical bills regardless of who’s at fault), and possibly medical payments coverage. Sometimes these overlap, sometimes they don’t, and figuring out who pays for what can make your head spin faster than the accident itself.
Here’s what’s particularly tricky in Texas – we’re a “fault” state, which means someone has to be determined responsible for the accident before certain coverages kick in. But here’s the catch: you might need medical care right now, while the insurance companies are still playing detective about who did what.
The Documentation Dance
This part is crucial, even though it feels overwhelming when you’re dealing with pain and insurance calls and everything else life throws at you.
Every interaction, every symptom, every treatment – it all becomes part of this paper trail that could matter months or even years down the road. I know, I know… you just want to feel better, not become a filing clerk. But think of it like taking photos after a fender-bender – you hope you never need them, but you’re really glad you have them if things get complicated later.
The medical professionals you see will be documenting everything anyway, but understanding why they’re asking so many questions (When did the pain start? Rate it on a scale of 1-10. Does it radiate anywhere?) helps you give them the information they need to help you properly.
Your first visit sets the foundation for everything that follows – treatment plans, insurance claims, legal considerations if they become necessary. It’s like the opening chapter of a book… you want to make sure you’re telling the right story from the start.
What to Bring – Your Essential Paperwork Arsenal
You know that sinking feeling when you’re standing at the pharmacy counter and realize you forgot your insurance card? Yeah, we’re avoiding that scenario entirely. Here’s your mission-critical list
Your insurance cards (both health and auto – trust me on this), driver’s license, and any photos you took at the accident scene. Even that blurry shot of the other car’s license plate could be gold later. If police showed up, grab that report number – most docs will want to see it, and it saves everyone time.
Oh, and bring a list of every medication you’re taking. I’m talking everything – that daily vitamin D, your blood pressure meds, even that melatonin you pop occasionally. Some pain medications don’t play well with others, and your doctor needs the full picture.
The Real Talk About Pain Documentation
Here’s something most people don’t realize: how you describe your pain on day one becomes part of your permanent record. So let’s get strategic about this.
Don’t downplay your symptoms because you’re trying to be tough – that’s not helping anyone. But also… don’t exaggerate. Doctors have heard it all, and they can spot inconsistencies from across the room.
Use specific numbers when they ask about pain levels. Instead of “it really hurts,” try “it’s about a 6 out of 10 when I turn my head, but shoots to an 8 when I look over my shoulder to change lanes.” See the difference? You’re giving them something concrete to work with.
And here’s a pro tip: mention how the pain affects your daily life. “I couldn’t sleep last night because rolling over woke me up three times” tells a much clearer story than just “my back hurts.”
Questions That Could Save You Headaches Later
Most people walk into that first appointment ready to answer questions, but the smart ones? They come prepared to ask them. Here are the queries that separate the prepared from the wishful thinkers
“What’s your timeline for my recovery?” This isn’t just curiosity – it’s planning. You need to know if we’re talking two weeks or two months so you can manage work, family, everything.
“Will I need any follow-up treatments, and what might those cost?” Because surprise medical bills are nobody’s friend, especially when you’re already dealing with insurance claims and car repairs.
“Should I be doing anything specific at home?” Some docs want you moving, others prefer rest. Don’t guess – ask outright.
The Insurance Dance – Making It Work for You
Let’s be honest – dealing with insurance after an accident feels like trying to solve a puzzle while blindfolded. But there are ways to make this smoother.
If you’re using your health insurance initially (which is often the smartest move), make sure the medical office knows this is accident-related. They’ll need to code everything correctly for potential reimbursement later. It’s like… think of it as keeping detailed receipts for a business expense. Messy now, but it’ll save you later.
Get everything in writing. When the scheduler tells you “insurance approved this,” ask them to note it in your file. When your adjuster says something’s covered, follow up with an email confirming what you discussed. I know, I know – it feels excessive. But you’ll thank yourself when there’s confusion six months down the road.
Setting Realistic Expectations for Your Recovery
Here’s what nobody tells you: healing isn’t linear. You might feel amazing on Tuesday and terrible on Wednesday, and that’s… completely normal.
Your first visit is really about establishing a baseline and catching anything serious. Don’t expect to walk out feeling like a million bucks – that’s not how this works. Think of it more like the opening chapter of your recovery story, not the happy ending.
Some things your doctor might recommend immediately – physical therapy, imaging, specific exercises. Others might be “let’s see how you feel in a week.” Both approaches are valid, and pushing for faster results usually backfires.
The key is building a relationship with your healthcare provider. This person might be working with you for weeks or months, so being honest, prepared, and realistic from day one sets everyone up for success. Plus, doctors remember patients who make their job easier – and that definitely works in your favor.
When Your Body Doesn’t Match Your Mind
Here’s what nobody tells you – your brain might be screaming “I’m fine!” while your body whispers something entirely different. After an auto accident, there’s this weird disconnect that happens. You walked away from the crash, you’re talking normally, so obviously everything’s okay, right?
Wrong. And this is probably the biggest challenge patients face during their first visit.
Your adrenaline is still pumping days later, masking pain signals. Meanwhile, soft tissue injuries – those sneaky little troublemakers – are just getting started. The doctor asks about your pain level, and you honestly answer “maybe a 3 out of 10” because that’s what it feels like right now. But here’s the thing… tomorrow it might be a 7.
The solution? Be brutally honest about any discomfort, no matter how minor it seems. Mention that weird stiffness when you turn your head, that slight ache in your lower back. Your doctor has seen thousands of these cases – they know what to look for. Think of them as a detective, and every small clue matters.
The Insurance Maze (And Why It Makes You Want to Scream)
Let’s talk about the elephant in the room – dealing with insurance companies. You’re already dealing with car repairs, rental cars, and now you need medical care too. The paperwork feels endless, and half the time you’re not even sure what you’re signing.
Here’s where people get tripped up: they assume their doctor’s office handles everything. Some do, some don’t. And if there’s any confusion about coverage, you might end up with unexpected bills.
Before your appointment, call your insurance company – yes, I know it’s painful – and ask specifically about auto accident coverage. Write down the representative’s name, reference number, and exactly what they tell you. Take photos of your insurance cards. Bring everything to your appointment, including the police report number if you have it.
Pro tip? Many clinics have insurance specialists who deal with auto accidents daily. Don’t be shy about asking them to walk you through the process. It’s literally their job, and they’ve untangled messier situations than yours.
The “I Should Be Tough” Trap
This one hits men particularly hard, but honestly? I see it in everyone. There’s this internal pressure to minimize what happened. “It was just a fender-bender.” “The other person had it worse.” “I don’t want to make a big deal out of nothing.”
But here’s the reality – whiplash can happen at speeds as low as 5 mph. Your body doesn’t care about your pride, and neither should your medical care.
The solution is mindset shifting. You’re not being dramatic by seeking medical attention after an accident. You’re being smart. Think of it like this: if your house had even minor foundation damage, you wouldn’t ignore it and hope for the best, right? Your body deserves the same attention.
When Pain Shows Up Fashionably Late
This might be the most frustrating part of the whole experience. You feel okay during your first visit, maybe even a little silly for being there. Then, two days later? You can barely turn your head without wincing.
This delayed onset happens because inflammation takes time to build up. Your muscles and ligaments are like that friend who seems fine at the party but texts you the next morning asking what happened… they need time to process the trauma.
Don’t panic when this happens. It’s normal – annoying, but normal. Call your doctor’s office and let them know about new or worsening symptoms. Many practices have protocols for follow-up care after auto accidents specifically because of this pattern.
The Documentation Dilemma
Here’s something that catches people off guard – everything needs to be documented. Every symptom, every limitation, every way the accident has impacted your daily life. And you need to be specific.
Instead of saying “my neck hurts,” try “I have sharp pain on the right side of my neck when I look over my shoulder to change lanes.” Instead of “I’m tired,” say “I’m having trouble sleeping because I can’t find a comfortable position.”
Start a simple log on your phone. Nothing fancy – just date, time, and what you’re experiencing. It helps during appointments and might be valuable if insurance disputes arise later.
The key thing to remember? Your first visit isn’t just about immediate treatment – it’s about establishing a baseline and creating a plan for your recovery. Be honest, be thorough, and don’t let pride get in the way of proper care.
Setting Realistic Expectations for Your Recovery
Look, I’m going to be straight with you – healing after an auto accident isn’t like what you see in the movies. There’s no montage where you’re magically better in three weeks while upbeat music plays in the background. Real recovery? It’s more like… well, it’s messier than that.
Most people think they should bounce back quickly, especially if they walked away from the accident. But here’s the thing – your body just went through something traumatic. Even “minor” accidents can leave you feeling like you’ve been put through a blender. And that’s completely normal.
The timeline varies wildly from person to person. Some folks start feeling better within a few days, while others might deal with discomfort for several weeks or even months. Age plays a role, sure, but so does your overall health, stress levels, and honestly? Just plain old genetics. Your coworker might’ve recovered from their fender-bender in a week, but that doesn’t mean you’re doing something wrong if you’re still hurting after three.
Whiplash, for instance – probably the most common injury we see – can be particularly sneaky. You might feel fine initially, then wake up the next morning feeling like you slept wrong for a decade. The pain can come and go in waves, which frankly drives people crazy because they never know if they’re actually getting better or not.
What Those First Few Weeks Actually Look Like
The first 72 hours are usually the worst, pain-wise. Your body’s inflammatory response is working overtime, which means you might feel progressively worse before you start feeling better. This freaks people out, but it’s actually… well, it’s your body doing its job.
During this time, you’ll probably be managing pain with a combination of rest, gentle movement (I know, sounds contradictory), and whatever treatment plan your doctor recommended. Some days you’ll feel optimistic – “Hey, I can turn my neck without wincing!” Other days? You’ll wonder if you’ll ever feel normal again.
This is where having realistic expectations becomes crucial. Progress isn’t linear. You might have a great day followed by two rough ones. That doesn’t mean you’re not healing – it just means healing is complicated.
Your Follow-Up Care Strategy
Your doctor will likely want to see you again within a week or two, depending on your injuries. Don’t skip these appointments, even if you’re feeling better. Sometimes symptoms can evolve or new ones can emerge as the initial shock wears off.
If you’re working with physical therapy – and there’s a good chance you will be – consistency matters more than intensity. Missing sessions here and there might seem harmless, but recovery works best when it’s steady. Think of it like… learning to play piano. You can’t practice for six hours one day and then skip the rest of the week and expect the same results.
Your PT might start you with gentle exercises that seem almost ridiculously easy. Trust the process. They’re rebuilding your body’s confidence as much as they’re addressing the physical damage.
Documentation and Insurance Realities
Here’s something nobody warns you about – the paperwork doesn’t end after your first visit. You’ll need to keep track of every appointment, every treatment, every day you miss work. Insurance companies love details, and if your case gets complicated (legally speaking), you’ll be grateful you kept good records.
Take photos of any visible injuries, even if they seem minor. Bruises fade, swelling goes down, but sometimes these visual records become important later. Keep a simple pain journal too – nothing fancy, just note how you’re feeling each day on a scale of 1-10.
When to Worry (And When Not To)
Some fluctuation in symptoms is normal. What’s not normal? Symptoms that are rapidly getting worse, new neurological issues like numbness or tingling that wasn’t there before, or severe headaches that don’t respond to typical pain management.
Your body’s pretty smart about healing itself, but sometimes it needs help. Don’t try to tough it out if something feels really wrong – that’s what your medical team is there for.
The key is staying connected with your healthcare providers and being honest about what you’re experiencing. Recovery after an auto accident isn’t a race, and there’s no prize for suffering in silence. Give yourself permission to heal at your own pace.
Getting into an accident can leave you feeling like you’re navigating a maze blindfolded – there’s so much information coming at you, and honestly, it’s overwhelming. But here’s what I want you to remember: that first visit to see a healthcare provider isn’t just about checking boxes or satisfying insurance requirements. It’s about taking care of you.
Your body has been through something traumatic, even if it was just a minor fender-bender. Sometimes the adrenaline masks what’s really going on underneath, you know? That soreness that shows up three days later isn’t being dramatic – it’s your body finally having a chance to process what happened. And that’s exactly why getting evaluated early matters so much.
What This Really Means for Your Recovery
Think of that initial appointment as laying the foundation for everything that comes next. Your doctor isn’t just looking for obvious injuries… they’re creating a roadmap. They’re documenting how you’re feeling right now – the good, the bad, and the “I’m not sure if this is related” – so they can track your progress over time.
And let’s be real about something – insurance companies want documentation. They want proof. Having a thorough record from that first visit can make a huge difference down the road if complications arise or if your recovery takes longer than expected (which, by the way, is totally normal sometimes).
The questions might feel repetitive. The forms might seem endless. But every detail you share helps paint a complete picture of your experience. Don’t minimize your symptoms or try to “tough it out” – this isn’t the time to be stoic.
You Don’t Have to Figure This Out Alone
Here’s something that might surprise you: many people walk out of their first post-accident appointment feeling more relieved than when they walked in. There’s something powerful about having someone listen to your concerns, validate what you’re experiencing, and create a plan moving forward.
Whether you’re dealing with obvious injuries or those nagging worries about what might be brewing beneath the surface, getting proper care early can prevent small issues from becoming bigger problems. And honestly? You’ve got enough to worry about right now without wondering if you should have sought medical attention.
The road ahead might feel uncertain, and that’s completely understandable. Between dealing with insurance calls, car repairs, and just getting back to normal life… it’s a lot. But your health shouldn’t be something you have to figure out on your own.
If you’ve been in an accident and you’re still on the fence about seeking care, or if you’re feeling lost about what steps to take next – we get it. We’ve walked alongside countless people through this exact situation, and we’re here to help you navigate not just your physical recovery, but all the questions and concerns that come with it.
You don’t need to have all the answers right now. You just need to take that first step. Give us a call when you’re ready – we’ll handle the rest together, one appointment at a time.