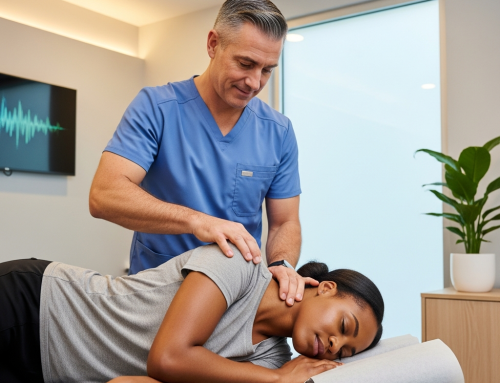
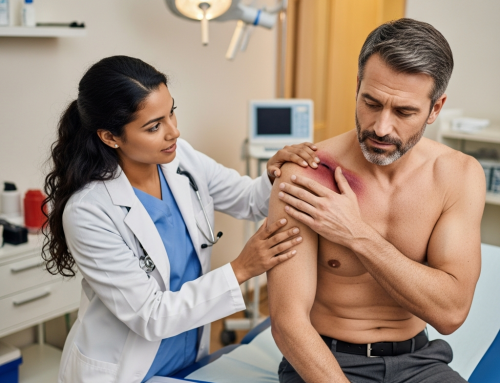
What a Personal Injury Clinic Treats After a Motor Vehicle Accident

The light turns green, you glance down at your phone for just a second, and then… *crunch*. Your world tilts sideways as your car lurches forward from the impact behind you. Your heart’s hammering, your hands are shaking, and honestly? You’re not even sure what just happened.
Sound familiar? If you’ve never been in a car accident, well… you’re lucky. But if you’re reading this, chances are you’re dealing with the aftermath of one right now – or you’re smart enough to want to know what you’d face if it ever happens to you.
Here’s the thing about car accidents – they’re like icebergs. What you see on the surface (the dented bumper, the broken headlight) is just the tip of what’s really going on. The real damage? That’s often happening inside your body, and it might not show up for hours, days, or even weeks.
I remember talking to Sarah, a patient who came to our clinic three weeks after what she called a “minor fender bender.” She kept saying, “It wasn’t even that bad – I was only going 15 miles per hour!” But there she was, struggling to turn her head without wincing, her lower back screaming every time she tried to get out of bed. That’s the sneaky truth about motor vehicle accidents… your body doesn’t care how “minor” it looked from the outside.
You might be sitting there right now, thinking you’re fine. Maybe you walked away from the accident, exchanged insurance information, and drove home. Your adrenaline was pumping, you felt okay in the moment – heck, you might have even declined the ambulance. But now, a few days later, you’re starting to notice things. That stiffness in your neck. The headaches that won’t quit. The way your shoulder catches when you reach for something.
Or maybe you’re on the other end of the spectrum – you know something’s wrong, but you’re not sure where to go. Your regular doctor says to give it time. Your insurance company is asking a million questions. And you’re caught in this weird limbo, dealing with pain that’s very real but somehow feels… dismissed.
That’s where personal injury clinics come in, and honestly, most people don’t really understand what they do until they need one. They’re not just about treating the obvious stuff – the cuts and bruises you can see. They specialize in the hidden injuries, the ones that make you feel like you’re going crazy because everyone keeps telling you that you “look fine.”
These clinics understand something crucial: your body is an intricate machine, and when it gets jolted around in a car accident – even at low speeds – things can go wrong in ways that aren’t immediately obvious. Think about it like this… if you shook a snow globe really hard and then tried to see what was damaged while all the snow was still swirling around, you’d miss a lot, right? That’s your body after an accident. The “snow” needs to settle before you can see the real damage.
What you’re about to learn might surprise you. We’re going to talk about injuries you probably never considered – things like how a seemingly minor rear-end collision can mess with your vision, or why your ribs might hurt weeks after an accident even though they weren’t directly hit. You’ll discover why that nagging headache isn’t just stress (though heaven knows, dealing with insurance companies is stressful enough), and why ignoring certain symptoms now could lead to chronic problems down the road.
More importantly, you’ll understand what personal injury clinics actually do – not just the treatments they offer, but how they approach your recovery differently than your regular doctor might. Because here’s what I’ve learned after years in this field: treating car accident injuries isn’t just about fixing what’s broken. It’s about understanding how everything in your body is connected, and how one injury can create a domino effect that impacts your entire well-being.
Your body is trying to tell you something. Let’s figure out what that is – and more importantly, what you can do about it.
Your Body’s Not-So-Silent Alarm System
Think of your body like a perfectly tuned orchestra – everything works together in harmony until suddenly, BAM. A car accident is like someone throwing a wrench into the middle of that symphony. Even what seems like a “minor” fender-bender can send shockwaves through systems you didn’t even know were connected.
Here’s the thing that catches most people off guard: your body doesn’t always scream when something’s wrong. Sometimes it whispers. Or worse – it stays completely silent for days, even weeks, before the real problems show up.
The adrenaline rush from an accident is basically nature’s version of really strong painkillers. Your body floods itself with these chemicals to help you deal with the immediate crisis. You might walk away feeling fine, maybe even a little superhuman… until three days later when you can barely turn your neck.
The Domino Effect Nobody Warns You About
Motor vehicle accidents don’t just hurt one thing – they create this cascade of issues that ripple through your entire body. It’s like when you throw a stone in a pond, except the pond is your musculoskeletal system and that stone just hit at 35 mph.
Your spine, for instance, isn’t just one solid piece (though wouldn’t that make things simpler?). It’s this intricate tower of 33 vertebrae, all cushioned by discs and held together by ligaments and muscles. When your car stops suddenly but your body keeps moving forward – well, that’s when things get complicated.
Whiplash is probably the most famous accident injury, and honestly, the name makes it sound almost cartoonish. But there’s nothing funny about what happens when your head snaps forward and backward faster than your neck muscles can react. It’s not just your neck, either – that violent motion can affect everything from your shoulders down to your lower back.
The Sneaky Stuff That Shows Up Later
Here’s where it gets really frustrating – some injuries are like that friend who shows up to the party fashionably late. Soft tissue injuries can take 24-72 hours to really announce themselves. Your muscles, tendons, and ligaments might be damaged, but they’re still in shock mode, kind of like when you burn your finger and don’t feel it right away.
Then there are the headaches. Oh, the headaches. These aren’t your garden-variety “I need more coffee” headaches. We’re talking about tension headaches from muscle strain, or even more concerning issues if there was any head trauma involved. Your brain, after all, is basically a three-pound bowl of jello sitting in a hard shell – it doesn’t love sudden stops any more than the rest of you does.
When Your Body Compensates (And Why That’s Actually Bad)
Your body is incredibly smart – sometimes too smart for its own good. When one part hurts, other parts jump in to help… except they’re not really designed for that extra work.
Say your neck is injured and you start holding your head differently to avoid pain. Suddenly your shoulders are working overtime, which makes your upper back tight, which changes how you walk, which can eventually affect your hips and knees. It’s like a really expensive game of Jenga where every piece you move affects the whole tower.
This is why that “I’ll just tough it out” mentality can backfire spectacularly. What starts as a manageable injury can snowball into chronic pain patterns that are way harder to fix later.
The Invisible Injuries
Not everything that hurts after an accident shows up on an X-ray. Muscle strains, ligament sprains, nerve irritation – these are all very real, very painful problems that can significantly impact your life, but they’re essentially invisible to traditional imaging.
It’s frustrating, actually. You know something’s wrong, but an X-ray shows your bones are fine, so everyone (including sometimes yourself) starts wondering if you’re imagining things. You’re not. Soft tissue injuries are notoriously tricky to diagnose and treat, which is exactly why specialized personal injury clinics exist.
The goal isn’t just to make the pain go away – though that’s obviously important. It’s to restore normal function and prevent those compensation patterns from turning into long-term problems. Because trust me, your future self will thank you for addressing this stuff properly now rather than hoping it just… disappears.
What to Expect During Your First Visit
Here’s what they don’t tell you about walking into a personal injury clinic for the first time – you’re probably going to feel overwhelmed. And that’s completely normal.
Most clinics will start with a detailed intake form that feels like it’s asking about every ache you’ve had since childhood. Don’t skip questions or downplay symptoms because you think they’re “not that bad.” That slight headache? Write it down. The weird tingling in your pinky? Mention it. I’ve seen too many patients minimize symptoms only to have them become major issues later.
Bring everything – your insurance cards, the police report, photos of the accident scene, and a list of any medications you’re taking (including that random vitamin D supplement you sometimes remember to take). If you have a smartphone, take photos of all your documents before the appointment. Trust me on this one.
The 48-Hour Rule That Could Save Your Case
Most people don’t realize there’s a critical window after an accident. Even if you feel “fine” initially – and I mean genuinely fine, not just telling yourself you’re fine – your body might be hiding injuries from you.
Adrenaline is sneaky. It can mask pain for hours, sometimes even days. That’s why personal injury clinics always stress the importance of getting evaluated within 48 hours, even if you think you don’t need it. Insurance companies love to argue that delayed treatment means your injuries weren’t “real” or weren’t caused by the accident.
Here’s a pro tip: if you’re reading this more than 48 hours after your accident and haven’t been seen yet, don’t panic. Just get in as soon as possible and be honest about why you waited. Maybe you were dealing with car repairs, or work was crazy, or you genuinely felt okay initially. Life happens – clinics understand this.
Questions Your Doctor Won’t Think to Ask (But You Should Bring Up)
Doctors are great at diagnosing obvious injuries, but sometimes the subtle stuff slips through the cracks. Before your appointment, spend some time really thinking about how you feel compared to before the accident.
Are you sleeping differently? Maybe you’re waking up in weird positions because certain sleeping positions hurt now. Has your mood changed? Post-accident depression and anxiety are incredibly common but often overlooked. Are you avoiding certain activities – not because they hurt, but because you’re anxious about them now?
And here’s something that catches people off guard: cognitive changes. If you’re having trouble concentrating at work, forgetting things more often, or feeling mentally “foggy,” that could be related to your accident. Don’t assume it’s just stress.
Documentation That Actually Matters
Everyone tells you to “document everything,” but what does that really mean? Let me get specific.
Keep a daily symptom diary – not just pain levels (though those matter), but everything. How did you sleep? What activities were harder today? Did you need help with anything you normally do yourself? The insurance adjuster doesn’t care that your pain was “a 7 out of 10,” but they do care that you couldn’t load your dishwasher or had to ask your neighbor to carry in your groceries.
Take photos, but make them meaningful. A bruise that looks minor in a photo might feel significant to you, and that’s valid. Date everything. If you’re using apps to track symptoms, great – but also keep a backup written record.
Working With Insurance (Without Losing Your Mind)
Here’s the thing about insurance companies – they’re not the enemy, but they’re definitely not your friend either. They have a job to do, and that job is to minimize their payouts.
Never, and I mean never, give a recorded statement to the other party’s insurance company without talking to your clinic first. They’ll call you when you’re tired, stressed, and just want this whole thing to go away. They’ll ask leading questions designed to get you to downplay your injuries.
Keep detailed records of every conversation with insurance – dates, times, who you spoke with, what was discussed. If they promise you something, get it in writing. Email is your friend here.
The Recovery Timeline Reality Check
Recovery isn’t linear, and anyone who tells you otherwise is selling something. You’ll have good days and bad days, sometimes without any obvious reason why.
Don’t let anyone – not your doctor, not your family, not your own inner critic – pressure you into feeling “better” on a timeline. Soft tissue injuries can take months to fully heal. Some people feel better in weeks; others need much longer. Both are normal.
The key is staying engaged with your treatment plan, even when you’re having good days. Skipping appointments because you feel better that day can actually slow your overall recovery.
When Insurance Companies Play Hard to Get
Let’s be real – dealing with insurance after an accident can feel like trying to solve a Rubik’s cube while blindfolded. You’re already dealing with pain, missed work, and a car that looks like it went through a blender, and then some adjuster starts questioning whether your neck pain is “really that bad.”
Here’s what actually helps: Get everything documented from day one. I know, I know – you’re thinking about a million other things right now. But that first visit to a personal injury clinic? It creates a paper trail that insurance companies can’t argue with. When a medical professional notes your range of motion, pain levels, and specific symptoms within days of your accident… that’s golden.
Don’t try to be a hero, either. If something hurts, say it hurts. If you’re having trouble sleeping because your back seizes up every time you roll over, mention that too. Insurance companies love to point to gaps in treatment or minimize symptoms that weren’t properly documented early on.
The “I Feel Fine” Trap That Gets Everyone
You know what’s wild? Sometimes you’ll walk away from an accident feeling completely normal. Adrenaline is one heck of a drug – it can mask injuries for hours, even days. Then Tuesday morning hits, and you wake up feeling like you got hit by… well, a car.
This delayed onset thing trips up so many people. They decline medical attention at the scene, go home, tough it out for a week, and then panic when the pain gets worse instead of better. By then, establishing a clear connection between the accident and your symptoms becomes more complicated.
The solution isn’t to rush to the ER for every minor fender-bender, but don’t ignore your body’s signals either. If you’re experiencing new aches, headaches, or that weird stiffness that wasn’t there before – get checked out. Personal injury clinics see this pattern constantly, and they know how to properly assess and document these delayed symptoms.
When Your Regular Doctor Just Doesn’t Get It
Here’s something that frustrates people endlessly – you go to your family doctor expecting help, and they basically shrug and tell you to take some ibuprofen. Or worse, they act like you’re exaggerating because your X-rays look “normal.”
Your family doctor is probably great at managing your blood pressure and annual checkups, but motor vehicle injuries? That’s a whole different beast. Soft tissue injuries, whiplash, and the complex cascade of problems that can develop after an accident – these require specialized knowledge and experience.
Personal injury clinics eat, sleep, and breathe this stuff. They understand that normal X-rays don’t rule out significant soft tissue damage. They know which symptoms cluster together and what treatments actually work for accident-related injuries. Most importantly, they document everything with the level of detail that makes lawyers and insurance companies take notice.
The Money Anxiety That Keeps You Up at Night
Let’s talk about the elephant in the room – you’re worried about medical bills piling up while you’re not even sure how badly you’re hurt or what your insurance will cover. Maybe you’re thinking, “What if this isn’t serious enough to justify all these appointments?”
Here’s the thing: most personal injury clinics work on a lien basis for motor vehicle accidents. Translation? You don’t pay upfront. They get paid when your case settles. This removes that immediate financial pressure and lets you focus on actually getting better instead of doing mental math about copays.
But – and this is important – don’t let financial relief turn into treatment overdose. Some clinics will keep scheduling appointments because, frankly, more visits mean more money when the case settles. Ask questions. Understand your treatment plan. You want to get better, not become a walking medical bill.
When Everyone Expects You to “Bounce Back”
The hardest part might be the people in your life who don’t understand why you’re still dealing with this “minor” accident weeks later. Your boss starts making comments about time off. Your spouse wonders why you can’t do household tasks you used to handle easily. Friends stop asking how you’re feeling because they assume you’re fine by now.
Recovery isn’t linear, and it’s rarely fast. Be honest with your support system about what you’re experiencing. Sometimes people just need education about how these injuries actually work – that whiplash can cause months of headaches, that back injuries can flare up randomly, that your brain might still be processing the trauma of the accident itself.
Don’t minimize your experience to make others comfortable. Your healing timeline is your healing timeline.
What to Expect During Your Recovery
Let’s be honest here – healing from a motor vehicle accident isn’t like recovering from a common cold. Your body’s been through trauma, and it needs time to repair itself properly. I know you probably want to feel better tomorrow (who wouldn’t?), but realistic expectations will actually help you heal faster and avoid setbacks.
Most soft tissue injuries – think whiplash, muscle strains, minor sprains – start showing improvement within the first few weeks. You might notice less morning stiffness, better sleep, or the ability to turn your head without wincing. But here’s the thing… improvement doesn’t mean you’re done healing. It’s more like your body saying, “Hey, we’re making progress here.”
More significant injuries? They’re playing the long game. Herniated discs, complex joint injuries, or anything requiring surgery – we’re talking months, not weeks. And that’s completely normal. Your body is literally rebuilding tissue, and that takes time. Think of it like renovating a house – you wouldn’t expect the contractor to finish in a weekend, right?
The Treatment Timeline Reality Check
During your first few visits, we’re in detective mode. We need to understand exactly what’s going on before we can map out your treatment plan. Some injuries are obvious right away, but others… well, they like to play hide and seek.
Week one through three is typically about reducing pain and inflammation. You might be doing gentle exercises, getting manual therapy, maybe using ice or heat (your therapist will guide you on which and when). Don’t be surprised if you feel a bit worse some days – that’s often part of the process, especially as we start mobilizing areas that have been guarding themselves.
Around week four to eight, if things are progressing well, we usually shift gears. Less focus on just managing pain, more emphasis on rebuilding strength and mobility. This is where patience becomes your superpower. You might feel like you should be doing more, pushing harder… but slow and steady really does win this race.
Some folks need ongoing care for several months. Actually, let me rephrase that – some folks *benefit* from ongoing care. There’s a difference between needing treatment because you’re broken and wanting treatment because it helps you feel your best.
Creating Your Personal Recovery Plan
Every treatment plan we create is like a fingerprint – unique to you. We consider your specific injuries, sure, but also your lifestyle, your goals, even your personality. Are you someone who needs detailed explanations of every exercise, or do you prefer the “just tell me what to do” approach?
Your plan might include physical therapy, chiropractic care, massage therapy, or a combination. We might refer you to specialists – orthopedic surgeons, pain management doctors, or psychologists who specialize in trauma recovery. Yes, the mental side matters too. Car accidents can mess with your head in ways you might not expect.
We’ll also talk about what you can do at home. Simple exercises, lifestyle modifications, even stress management techniques. Because here’s what I’ve learned after years in this field – the patients who do best are the ones who become active participants in their recovery, not passive recipients of treatment.
When to Expect Improvements (And When to Worry)
You should start noticing *something* positive within the first few weeks of treatment. Maybe it’s sleeping better, or being able to sit at your desk for longer periods. Small wins count – actually, they’re huge.
If you’re not seeing any improvement after 4-6 weeks of consistent treatment, that’s worth a conversation with your care team. Not panic mode, just… a conversation. Sometimes we need to adjust our approach or look deeper into what’s going on.
Red flags? Symptoms that are getting worse despite treatment, new symptoms that seem unrelated to your original injury, or pain that’s spreading to new areas. These don’t necessarily mean something terrible is happening, but they do mean we need to reassess.
The Long View
Most people return to their normal activities within a few months. But “normal” might look a little different than before – and that’s okay. You might discover you need to take breaks more often, or that certain movements require more attention.
The goal isn’t just to get you back to where you were before the accident. It’s to get you there stronger, more aware of your body, and with tools to prevent future problems. Because honestly? That’s better than just “back to normal.”
Your Recovery Matters – And So Do You
The thing about car accidents is that they don’t just mess with your schedule for a day or two. They have this sneaky way of affecting everything – your morning routine (can you even lift that coffee pot?), your work performance, even how you sleep at night. And honestly? That’s completely normal.
You might be sitting there right now, three weeks post-accident, wondering why your shoulder still aches when you reach for something, or why you get these weird headaches that weren’t there before. Maybe your family keeps asking if you’re “better yet” and you’re not quite sure how to answer because… well, you’re not sure yourself.
Here’s what I want you to know: healing isn’t linear. It’s more like a messy zigzag where some days feel amazing and others remind you that your body went through something traumatic. That whiplash that seemed minor at first? It can take weeks to fully show itself. Those lingering muscle spasms? They’re your body’s way of protecting itself, even when the immediate danger has passed.
Personal injury clinics understand this timeline – they’ve seen it thousands of times. They know that your pain is real, even when X-rays look “normal.” They get that you might need different types of care as you heal, maybe starting with pain management and gradually moving toward strengthening and mobility work.
What makes these clinics different is their whole-person approach. They’re not just treating your injured neck or bruised ribs – they’re treating *you*. The person who needs to get back to work, who has kids to pick up from soccer practice, who wants to sleep through the night without waking up stiff and sore.
And let’s talk about something that doesn’t get mentioned enough: the emotional side of recovery. Car accidents can shake you up in ways that have nothing to do with physical injuries. You might find yourself more anxious when driving, or replaying the accident over and over. Quality personal injury clinics often have counselors or can connect you with mental health resources because they understand that true healing addresses both body and mind.
You don’t have to figure this out alone. Actually, you shouldn’t have to. Your insurance likely covers treatment at personal injury clinics, and many work directly with your provider to handle the paperwork hassle. Because honestly, the last thing you need when you’re trying to heal is wrestling with insurance forms.
If you’re reading this and thinking, “Maybe I should get checked out,” – listen to that voice. Even if your accident was “minor,” even if you walked away feeling okay, even if it’s been weeks and you’re just now noticing issues. Your body deserves proper care, and you deserve to feel like yourself again.
Getting help doesn’t mean you’re weak or dramatic – it means you’re taking your recovery seriously. And that’s exactly what you should be doing.
Why not give us a call? We’d love to chat about what you’re experiencing and how we might be able to help. No pressure, no sales pitch – just real people who understand what you’re going through and want to see you get better. Because you will get better. Sometimes you just need the right support to get there.